- 1/7 – Principles
- 2/7 – Indications
- 3/7 – Approach
- 4/7 – Reduction
- 5/7 – Drilling
- 6/7 – Lag screw fixation
- 7/7 – Aftertreatment
1. Principles
Lesion classification
There is a number of lesions produced by a hyperflexion mechanism.
All of these are characterized by detachment of the central slip of the extensor apparatus. They are considered as acute boutonnière injuries.
Lesions without dislocation
- Hyperflexion with detachment of the central slip (no fracture)
- Simple avulsion fracture of the central slip with a small nonarticular fragment
- Simple avulsion fracture of the central slip with a larger articular fragment
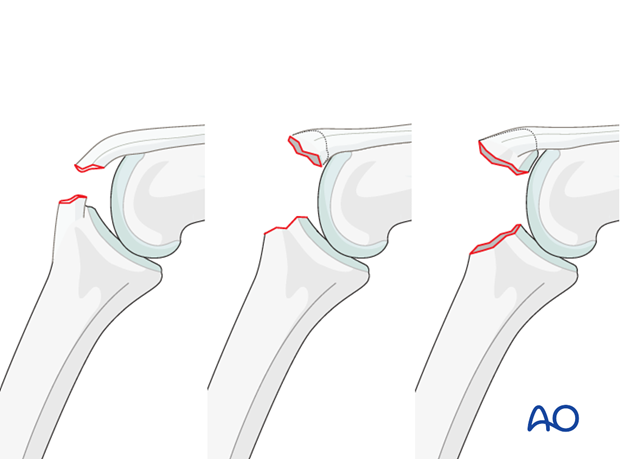
Sometimes, lesions such as these are considered minor injuries by traumatologists, and often they are confused with simple ligament sprains. However, if not treated early and correctly, boutonnière deformity, which is difficult to treat at a later stage, is a common consequence.
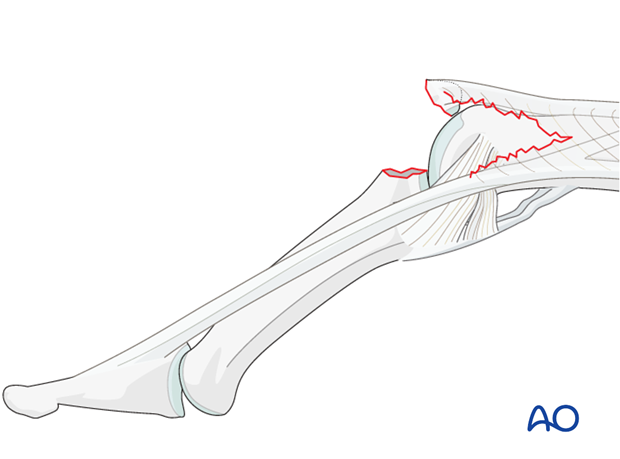
Lesions with palmar dislocation
If palmar dislocation of the PIP joint is present, a rupture of the collateral ligament and detachment of the central slip are involved. In injuries of this kind, a swan-neck deformity is present, and the finger cannot be flexed.
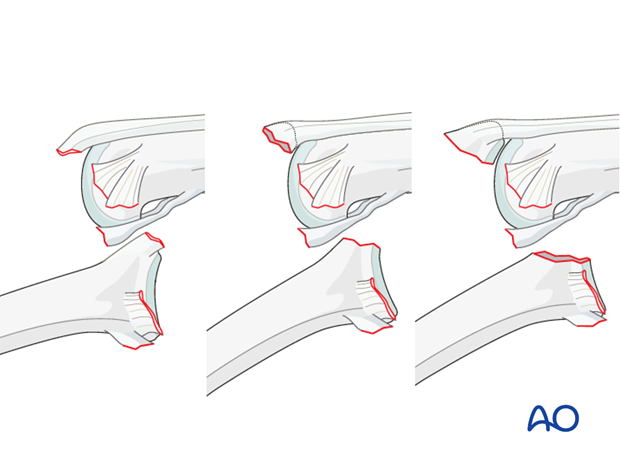
Lesions with dislocations
- Detachment of the central slip without a fracture
- Avulsion fracture of the central slip with a small nonarticular fragment
- Avulsion fracture of the central slip with a larger articular fragment
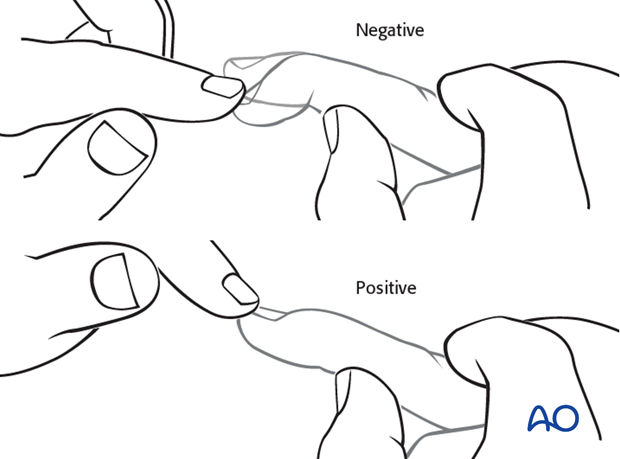
Undislocated lesions: Early diagnosis by Stark maneuver
Early diagnosis of injuries without dislocation is important. This is not always easy due to the swelling and often inconclusive x-rays.
Keep the PIP joint hyperextended. Passively flex the DIP joint.
If passive movement of the DIP joint is limited, this is a strong indication for the presence of a central slip detachment.
Compare with the uninjured hand.
Recognizing detachment of the central slip
In order to recognize detachment of the central slip, ask the patient to extend the PIP joint with the MP joint in hyperextension.
If the PIP joint can be fully extended in this position, the central slip is still attached, and nonoperative treatment may be indicated.
Pitfall: MP joint not hyperextended
If the MP joint is not hyperextended, extension of the PIP joint may still be possible, even with a detached central slip. In this case, the intrinsic muscles will extend the joint.
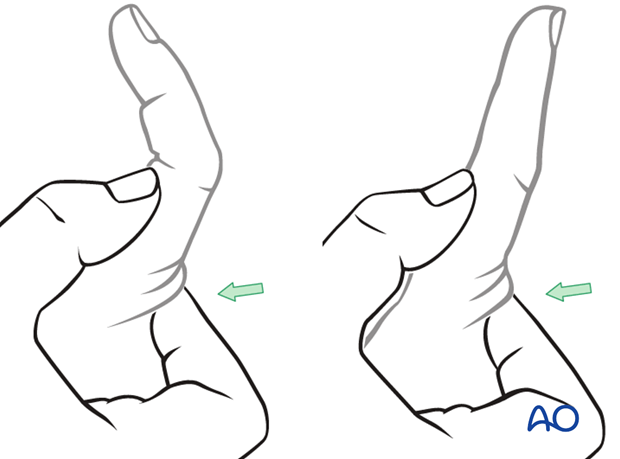
Mechanism of the injury
These injuries are commonly caused by sporting accidents, often in ball games such as cricket, volleyball, basketball, etc.
Typically, hyperflexion of the finger causes an avulsion lesion of the central slip.
Often, in addition to hyperflexion, impact on the finger tips causes longitudinal compression forces on the middle phalanx towards the proximal phalanx, leading to an additional impaction fracture.

Deforming forces
Boutonnière deformity
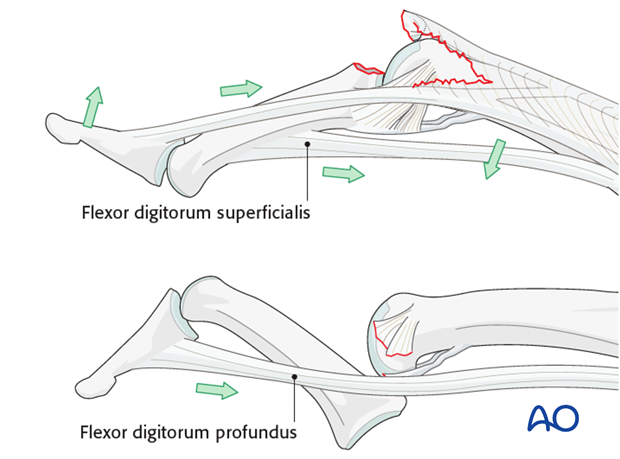
When the central slip is detached, the lateral bands are palmarly displaced and pull the DIP joint into hyperextension.
The flexor digitorum superficialis (FDS) pulls proximally on the middle phalanx, forcing the PIP joint into flexion.
Swan-neck type deformity
If the middle phalanx is palmarly dislocated at the PIP joint by the energy of the trauma, the flexor digitorum profundus (FDP) pulls the DIP joint into flexion.
2. Indications
Nonoperative treatment
The majority of these lesions can be treated by closed reduction and splinting for 6 weeks, leaving the DIP joint free for active mobilization. Encourage the patient actively to flex and extend the DIP joint, which allows healing of the lateral band in the right position.

Large fragment avulsion fracture
An avulsion fracture of the central slip can usually be reduced by full extension. Confirm using image intensification.
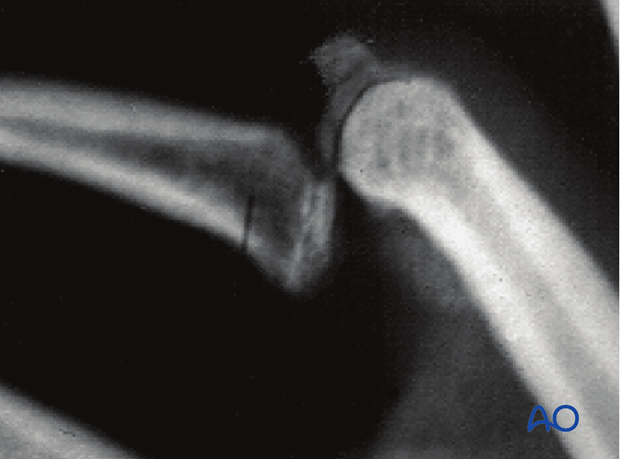
If the fracture does not reduce, usually this is an indication of soft-tissue interposition. In such cases, surgical treatment is indicated.
Possible treatments include lag screw fixation, or percutaneous K-wire fixation. Cerclage compression wiring is another option.
This form of fixation was referred to as “Tension band wiring”. We now prefer the term “Cerclage compression wiring” because the tension band mechanism cannot be applied consistently to each component of the fracture fixation. An explanation of the limits of the Tension band mechanism/principle can be found here.
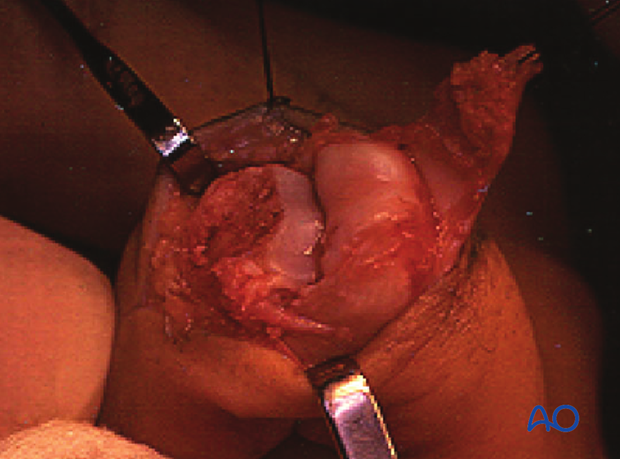
3. Approach
For this procedure a dorsal approaches to the PIP joint is normally used.
4. Reduction
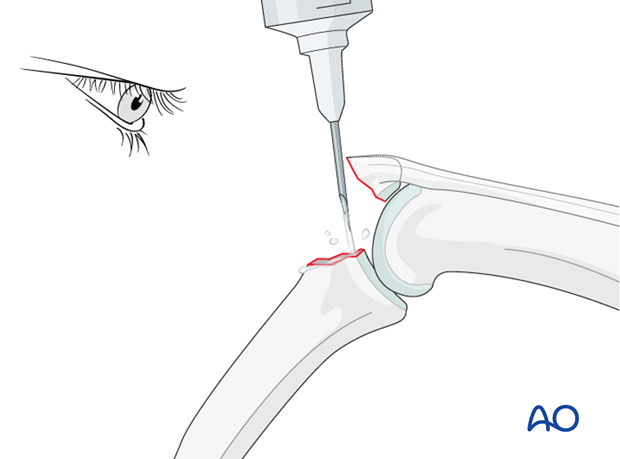
Clean the fracture site
Flex the PIP joint. In order to gain a better view of the fracture and the joint, use a syringe to clear out blood clot with a jet of Ringer lactate.
Often the presence of comminution is not apparent from the x-rays, and can only be determined under direct vision.
Use a dental pick carefully to free interposed tissues, and to remove blood clot and other debris.
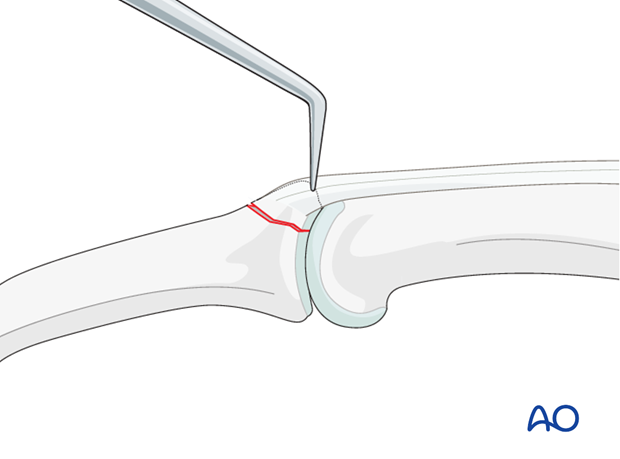
Reduce the fracture
Extend the PIP joint and apply traction. Put manual pressure on the palmar side of the middle phalanx.
Complete the reduction with help of a dental pick.
5. Drilling
Choosing screw size
The maximal permitted diameter of the screw head is one third of the diameter of the avulsed fragment.
Screw length needs to be adequate for the screw just to penetrate the opposite cortex.
Most commonly, a 1.0 mm, or 1.3 mm screw is used. The use of a 1.0 mm screw will be illustrated.
Pitfall: causing comminution
Be very careful when drilling, lest comminution of the fragments be caused.
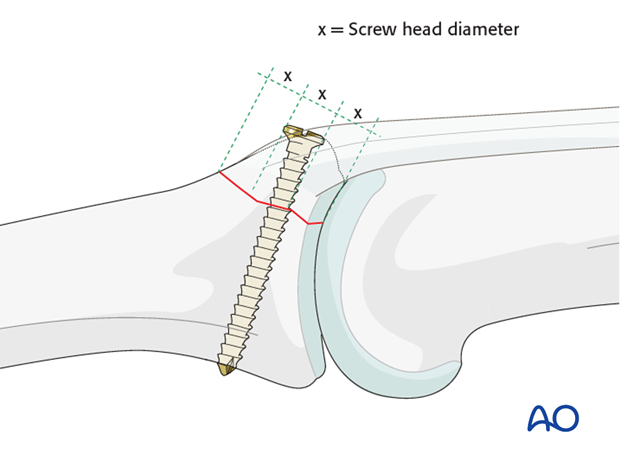
Drill a gliding hole
Maintaining the reduction with a drill guide, drill a gliding hole using a 1.0 mm drill bit.
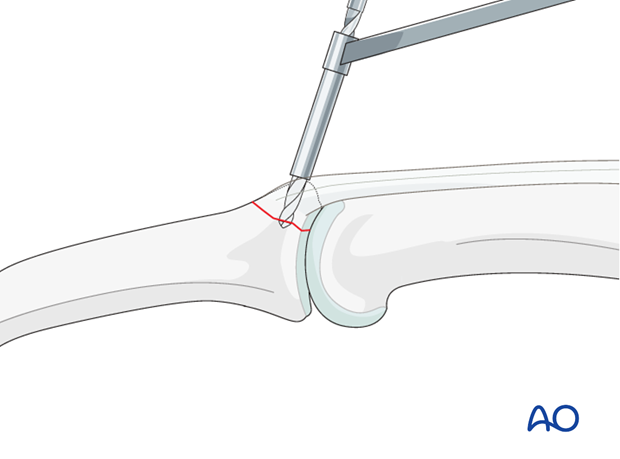
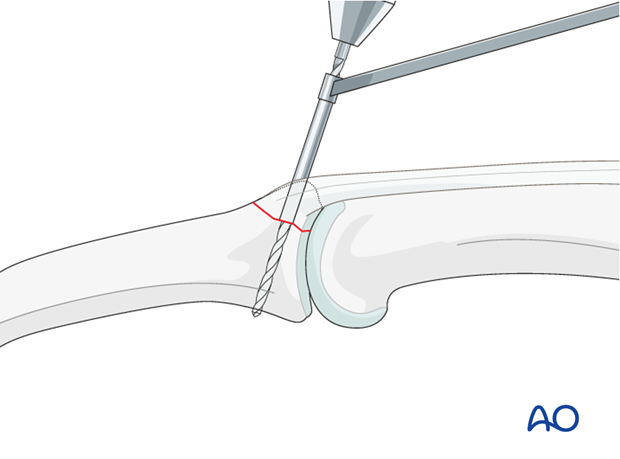
Drill threaded hole
Now use a corresponding drill bit (0.8 mm drill) to drill a thread hole into the opposite fragment, penetrating the far (trans) cortex.
Use a depth gauge to measure for accurate screw length.
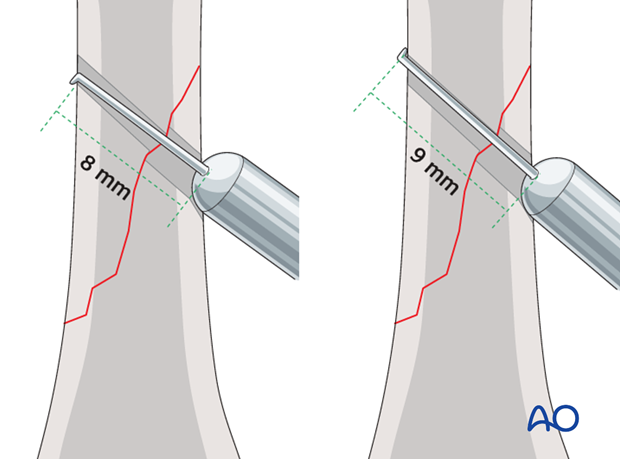
Pitfall: Oblique measuring
Use a depth gauge to measure for screw length.
When measuring for screw length in oblique drill holes, the measurement to the acute angle is different from the measurement to the obtuse angle. This problem increases with the degree of obliquity.
Always measure both angles and use the longer measurement. However, keep in mind that too long a screw can protrude to the extent that it puts the soft tissues at risk.
6. Lag screw fixation
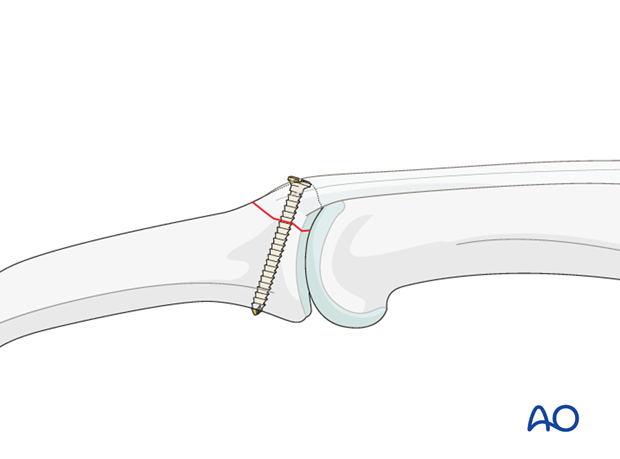
Screw insertion
Insert a self-tapping lag screw and tighten it. The screw should just penetrate the opposite cortex.
Check using image intensification. Reduction must be anatomical.
Pitfall: Overtightening the screw
Be careful not to overtighten the screw as this may result in comminution of the fragment.
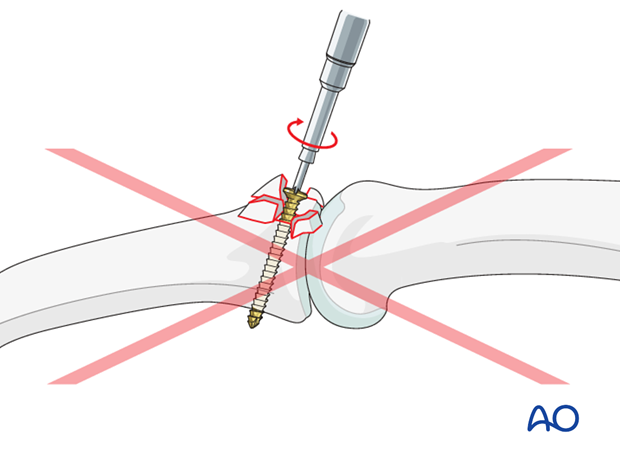
Check stability of the fixation.
If there is any doubt about the stability of the fixation, insert a K-wire obliquely crossing the PIP joint. Be careful to avoid conflict with the lag screw.
The K-wire can be removed after 2-3 weeks.
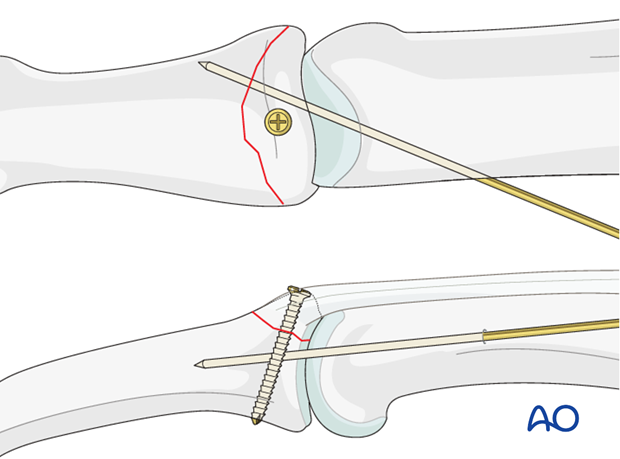
7. Aftertreatment
Aftertreatment depends on the size of the fragment, the quality of the bone, and the stability gained by the fixation.
The PIP joint is immobilized in extension in a palmar splint, leaving the DIP joint free.
DIP ...

Casting, splints, and support bandages
More than 50 instruction videos
... and MP joint movement is encouraged immediately to avoid extensor tendon adhesion.
If the fixation is strong enough, the patient is encouraged to take off the splint 2-3 times daily, and to begin with gentle active exercises, provided no transarticular K-wire has been used.
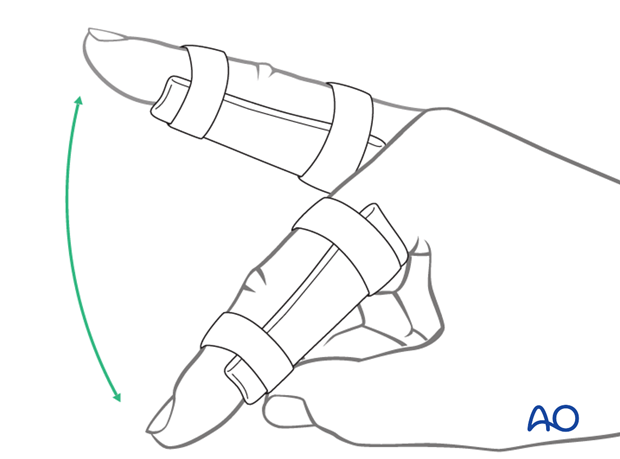
Functional exercises
After 3 weeks, the splint (and any K-wire) is removed, and unrestricted active flexion and extension are permitted. Passive motion is only permitted after 4 weeks.












