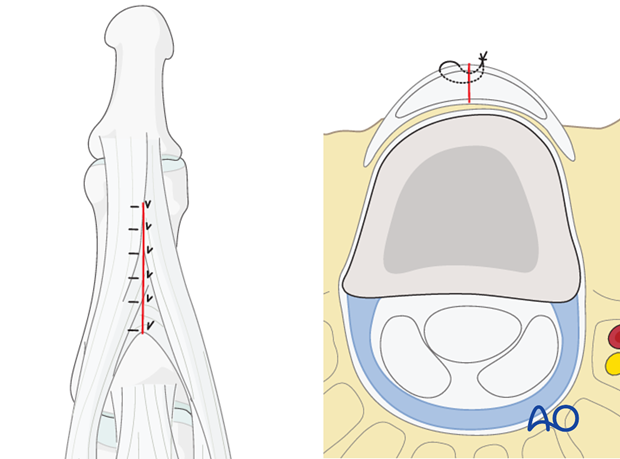
Dorsal approach to the middle phalanx
1. Indications
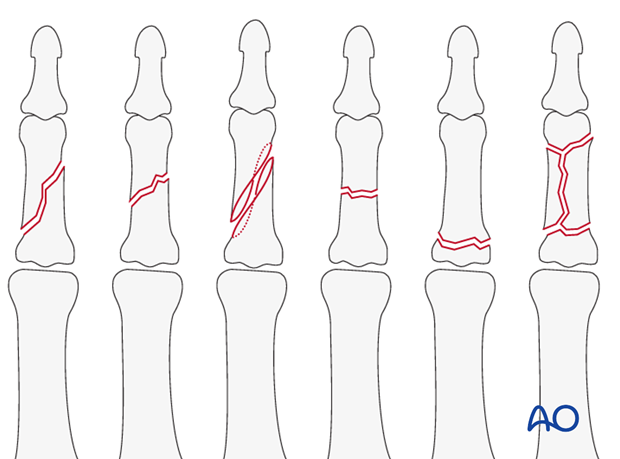
The dorsal approach is indicated for oblique, spiral, comminuted, or transverse fractures of the diaphysis, or metaphysis of the middle phalanx.
It can also be used for corrective osteotomies of malunited fractures.
2. Nerve identification
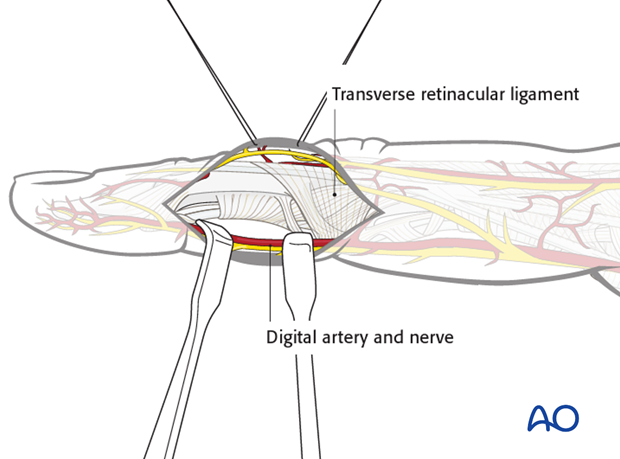
Blunt dissection extends the approach through the thin subcutaneous tissue, taking care to identify and protect the dorsal sensory branches of the radial, ulnar, and median nerves.
3. Vein identification
The dorsal venous system of the fingers has longitudinal and transverse branches. Be careful to preserve the longitudinal branches. The transverse branches may be ligated, or cauterized with a bipolar cautery, for better exposure, but preserve as many dorsal veins as possible to avoid venous congestion and swelling.
4. Skin incision
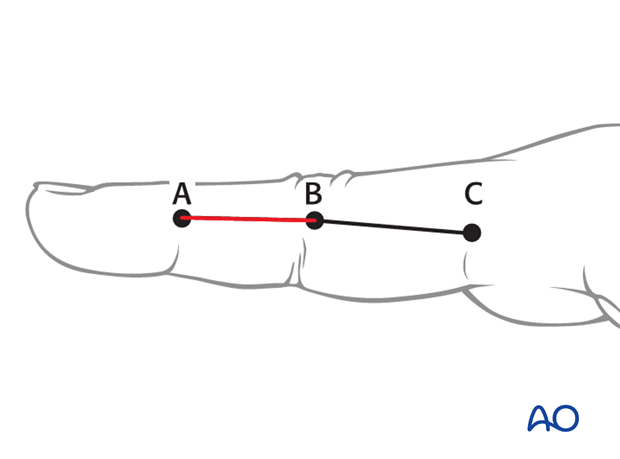
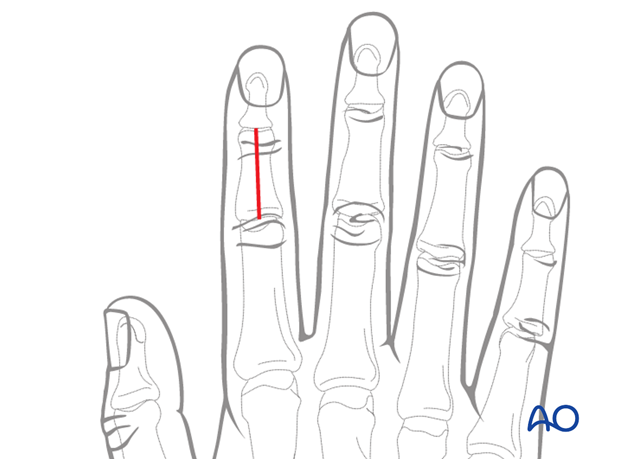
Make a straight, midline, dorsal skin incision, starting at the proximal interphalangeal (PIP) joint and ending at the distal interphalangeal (DIP) joint. Depending on the fracture geometry, the incision may be shorter.
With this incision, vascularity and venous drainage are well preserved. Early postoperative motion will prevent scarring between skin, tendon and bone.
The disadvantage of this incision is that any skin and tendon scarring will be in the same line.
5. Alternative: curved skin incision
Alternatively, make a curved skin incision extending from the PIP joint to the DIP joint. The convexity of the incision is planned so that the scar does not involve the radial border of the index, or the ulnar border of the little finger. The fracture configuration and implant placement must be taken into account when planning the incision.
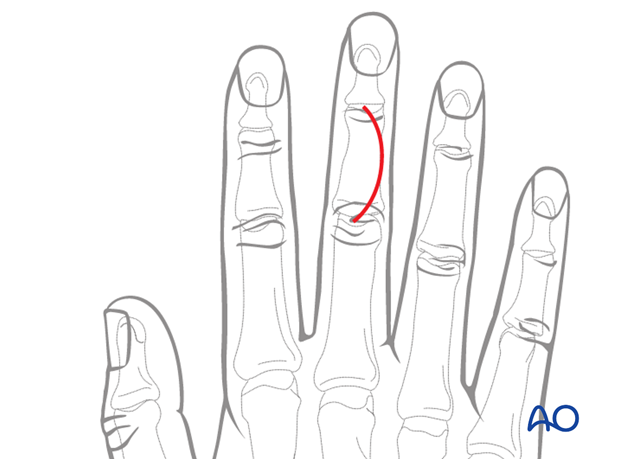
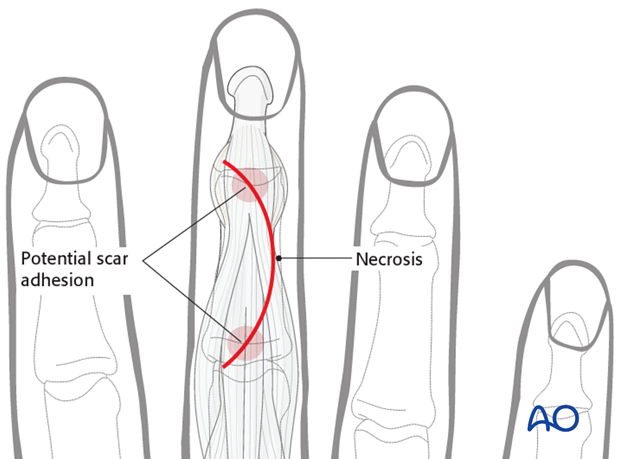
The advantage of the curved incision is that the scarring of skin and tendon is not in line.
The disadvantage is reduced vascularity at the apex of the curve with a risk of necrosis and delayed skin healing.
6. Expose terminal extensor tendon
The approach is extended by blunt dissection through the thin subcutaneous tissues.
Keep in mind, when developing the flaps, that the layers must be elevated together, in order to avoid devascularization.
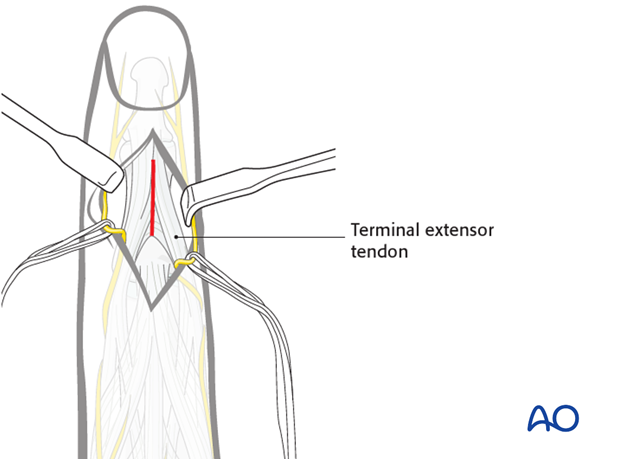
Expose the terminal extensor tendon with its triangular ligament.
Make a longitudinal incision through both the terminal extensor tendon and its triangular ligament, taking care to preserve the periosteum.
7. Bone exposure
After incising the terminal extensor tendon and its triangular ligament, two small retractors are used to expose the bone.
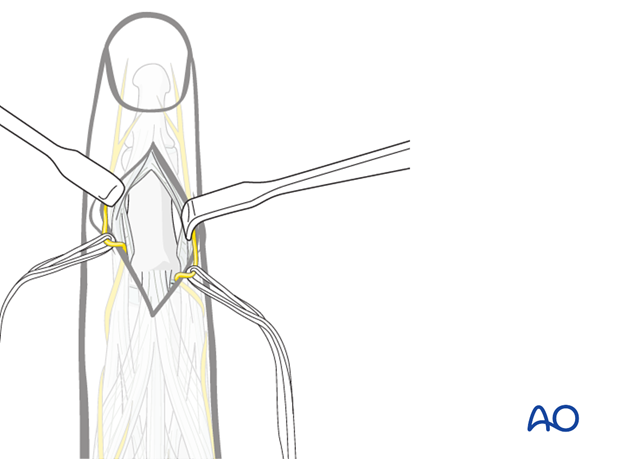
8. Wound closure
The terminal extensor tendon and its triangular ligament should be repaired with fine interrupted mattress sutures.