Nonoperative treatment
1. General considerations
Nonoperative treatment is based on immobilization of the DIP joint in extension, leaving the PIP joint free.
Nail bed injuries may need repair and reduction of the nail plate into the nail fold.
2. Release of subungual hematoma
Closed injuries, especially crush injuries, are often accompanied by a tense subungual hematoma. They can be exceedingly painful due to the pressure within the closed space.
Before further treatment, the hematoma can easily be released by puncturing the nail with a heated needle.
Apply a simple splint and cool the finger with the judicious use of an ice pack.

3. Repair of the nail bed and reinsertion of the nail
It is advisable precisely to repair the nail bed or the germinal zone. Otherwise, permanent deformity of the nail growth can result.
These procedures are challenging to conduct successfully without the help of magnifying loupes.
Use separate fine absorbable sutures.
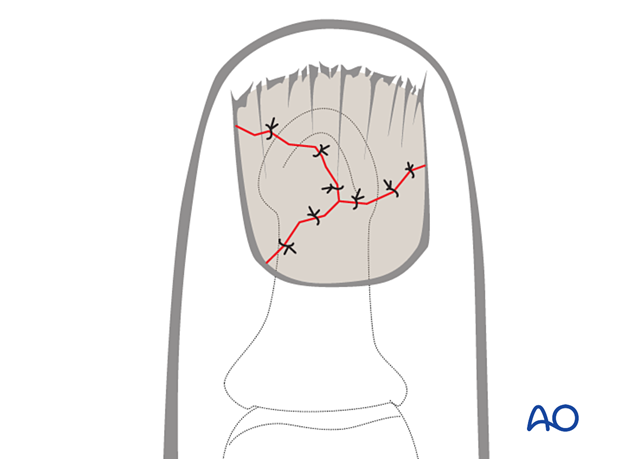
In simple transverse or oblique lacerations of the nail bed, a running suture may be used.
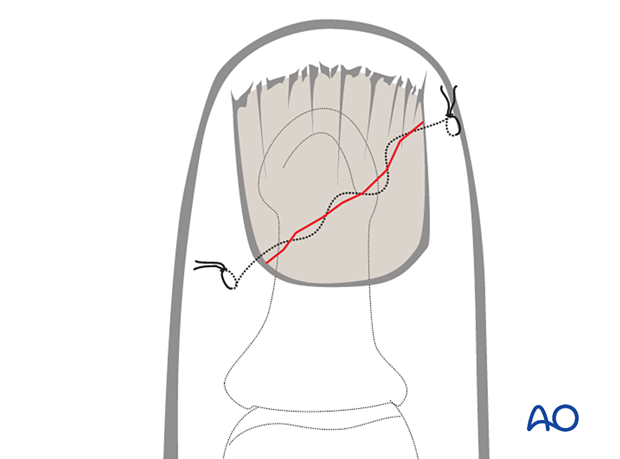
Pitfall: Eversion or inversion of nail bed edges
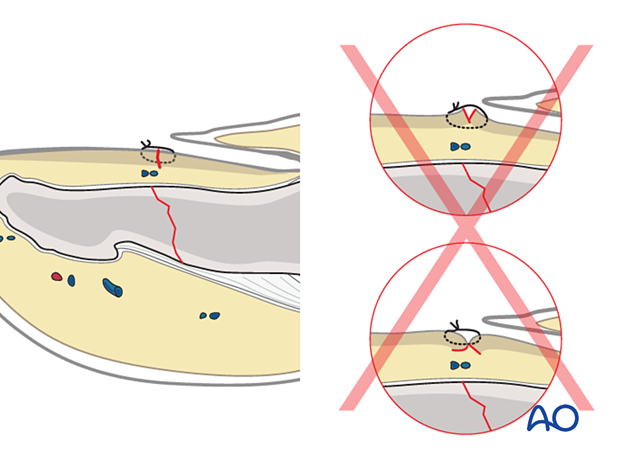
Nail reinsertion
There are four main reasons for nail reinsertion:
- Preventing scarring between the eponychium and the germinal matrix
- Stabilization of the fracture (external splinting)
- Nail acts as a biological barrier and protection
- Nail acts as a template for the growth of a new nail
Insert a needle with a 5-0 nonresorbable nylon suture from the dorsal aspect into the sinus, exiting the sinus distally to the eponychium.
Pass the needle through the proximal edge of the nail plate.
Then pass the needle back through the nail plate and the sinus of the nail so that it exits level with the first pass of the suture, separated from it by approximately 5 mm.
Draw the nail plate back into the sinus with gentle traction on both suture ends.
Tie the suture over a cotton, or foam, ball to avoid skin pressure injury.

After reinsertion and proximal fixation, the nail tends to tilt upwards distally.
To prevent this, use a small nonabsorbable suture at the nail’s distal tip to secure it to the nail bed.
This can be removed after 10 days.

4. Splinting
The DIP should be splinted distally from the PIP joint.

Dorsal splint vs palmar splint
Using a dorsal splint has the advantage of leaving the patient with the ability to pinch while the digit is immobilized.
However, proponents of palmar splinting argue that the palmar aspect is better cushioned than the dorsal and, thereby, can tolerate the splint better.
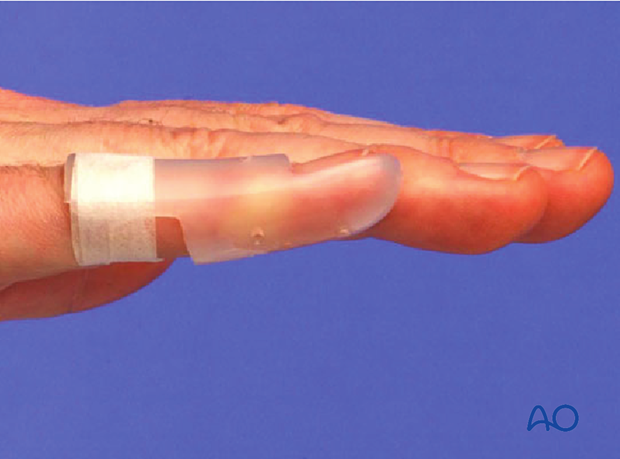
Contoured custom thermoplastic splint
The advantage of a custom thermoplastic splint is that it is adapted better to the shape of the finger and is easier to change.
5. Aftercare
Postoperative phases
The aftercare can be divided into four phases of healing:
- Inflammatory phase (week 1–3)
- Early repair phase (week 4–6)
- Late repair and early tissue remodeling phase (week 7–12)
- Remodeling and reintegration phase (week 13 onwards)
Full details on each phase can be found here.
Management of swelling
The arm should be actively elevated to help reduce any swelling.
Cleaning
Removal of the splint and skincare must be performed by the patient at weekly intervals.
Mobilization
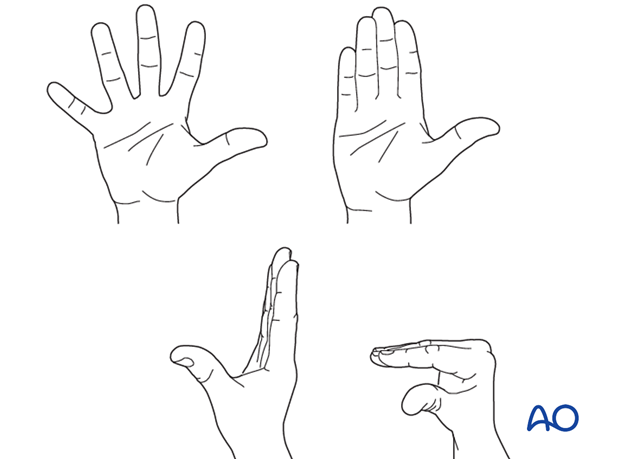
Hand therapy is recommended to prevent soft-tissue atrophy and joint contracture (typically extension of MCP joint and flexion of PIP joint), which leads to a poor outcome, and subsequent treatment is difficult.
Functional exercises of the nonimmobilized joints should be started immediately to keep uninjured joints mobile.
Follow-up
In tuft fractures, splinting is mainly performed for pain treatment, and usually, after 3 weeks, the splint can be discontinued.
In shaft fractures, x-ray controls must be performed immediately after the splint has been applied. After 4 weeks, an x-ray without the splint is taken to confirm healing. Splinting can then usually be discontinued, and active mobilization is initiated.
If, after 8 weeks, x-rays confirm healing and the patient is painless, full loading can be permitted.













