Multifragmentary fracture of the diaphysis and distal end segment
Definition
Wedge and multifragmentary fractures of the shaft and tuft are classified by the AO/OTA as 78.2–5.3.2B/C, where 2–5 indicates the finger involved.
In multifragmentary fractures, the comminution may be limited to the tuft or extend into the diaphysis.
Shaft fractures may be wedge or comminuted.
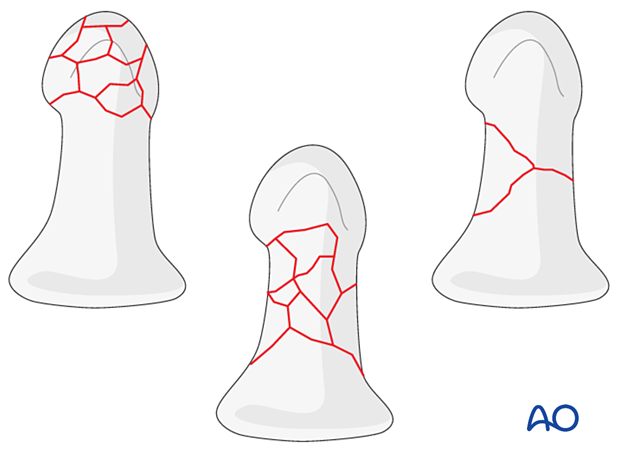
Further characteristics
Fractures of the distal phalanx are the most common fractures in the hand.
Most of these fractures result from direct impact or crush injuries with associated soft-tissue (nail bed or pulp) lacerations. Most frequently, there is a comminuted tuft fracture.
Common complications of these injuries are:
- Altered sensibility (numbness, hyperesthesia, tenderness)
- Cold hypersensitivity (cold intolerance)
- Restriction of DIP joint movement
- Nail growth abnormalities
Classification of distal phalangeal fractures (after Schneider)
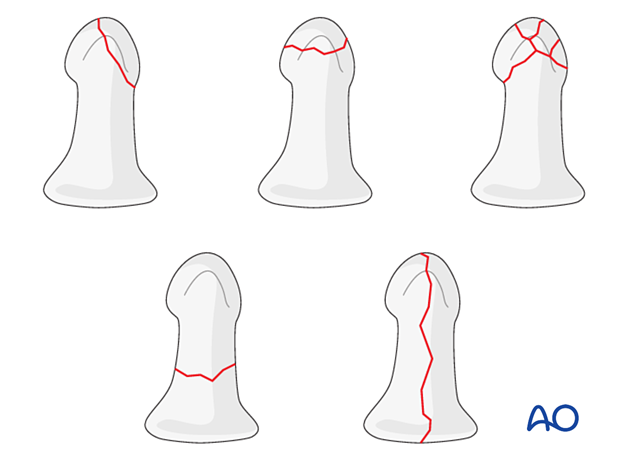
Schneider divides distal phalangeal fractures into tuft, shaft, and articular fractures.
Tuft fractures include
- Simple fractures
- Comminuted fractures
Shaft fractures include
- Transverse fractures
- Longitudinal fractures (may extend to involve the DIP joint)
Articular fractures include
- Palmar (flexor digitorum profundus avulsion fractures)
- Dorsal (extensor avulsion, mallet fractures)
Imaging
AP and lateral view x-rays should be taken.













