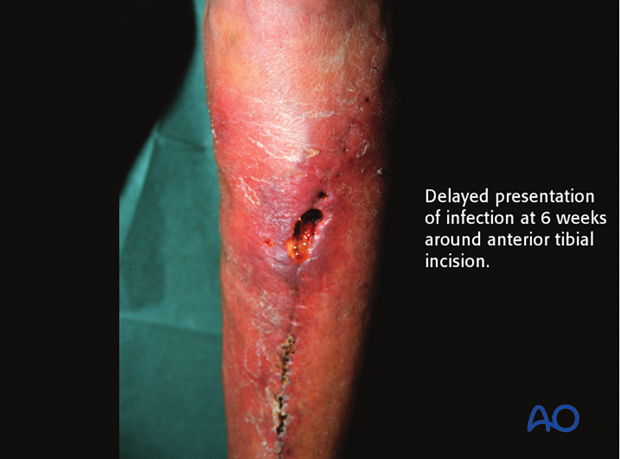
Delayed presentation of infection
1. Delayed presentation of infection
Clinical signs
Some fracture wound infections present more than 2 weeks after fracture surgery. Often, there are mild systemic, or local, symptoms, such as low-grade fever, or slight local skin reddening. Ultimately, increasing pain, redness and swelling, etc., become evident. Sometimes, late onset of wound breakdown, or drainage (formation of a sinus), is the first indication that an indolent infection is present.
An infection that presents more than 2 weeks after fracture surgery should be considered differently, with the need for more extensive and intensive treatment.
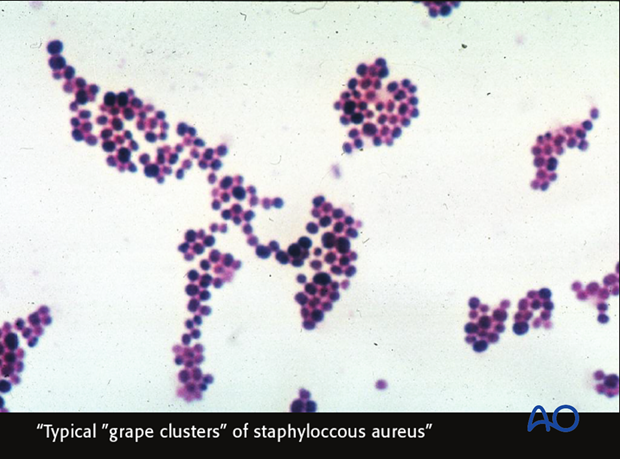
Microbiology and surgical treatment
The microorganisms that cause delayed presentation infection are usually of lower virulence (e.g., coagulase-negative staphylococci). Infecting bacteria have often been present long enough to have formed a protective biofilm, adherent to a metallic implant and dead bone, and are consequently more inaccessible to antibiotics.
Débridement of all dead, or infected, tissue is required, and provides the opportunity for fracture and wound assessment. Hardware may need to be removed, although if it still provides absolutely stable fixation, an attempt may be made to retain it, until the fracture has healed. This requires surgical removal of allinfected tissues, staged wound coverage and appropriate antibiotics.
If more extensive excision, including substantial bone removal, is needed, or internal fixation has to be removed, external fixation will be required, together with more complex reconstruction of bone and/or soft tissue.