ORIF - Lag screw with protection plate
1. Principles
Lag screw and protection plate
Intact wedge fractures can be reduced and fixed with lag screws. An additional lateral protection plate is always needed.
This procedure can only be carried out as an open one but without periosteal elevation.
The positions of the lag screws depend on the fracture pattern. If possible at least one lag screw should be placed through the plate.
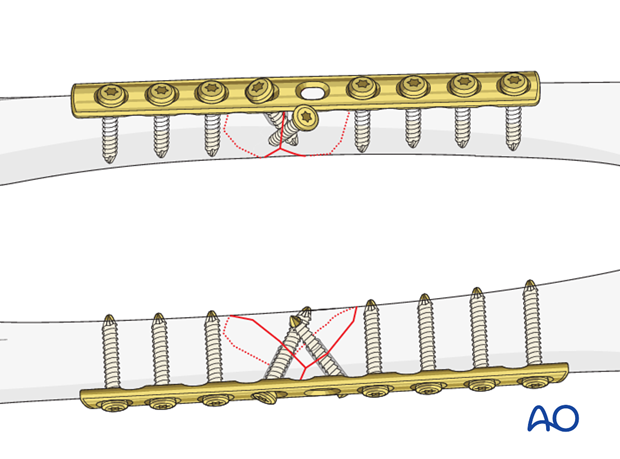
If necessary, both lag screws may be inserted outside the plate.
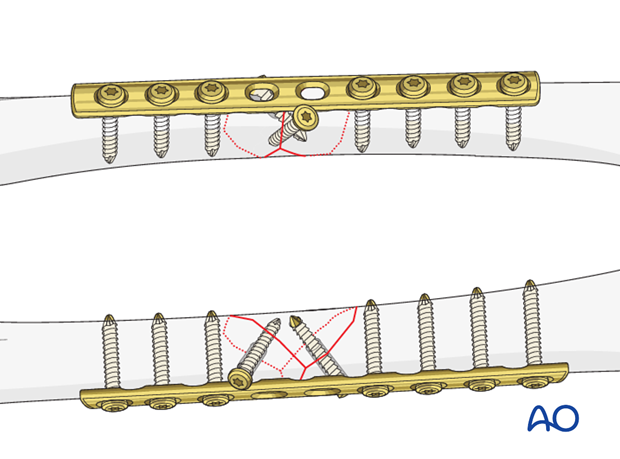
Plate length
It is crucial to use a plate that is long enough so that at least three bicortical screws can be inserted into each main fragment.

2. Patient preparation
The patient may be placed in one of the following positions:
3. Approach
For this procedure a lateral approach is used.
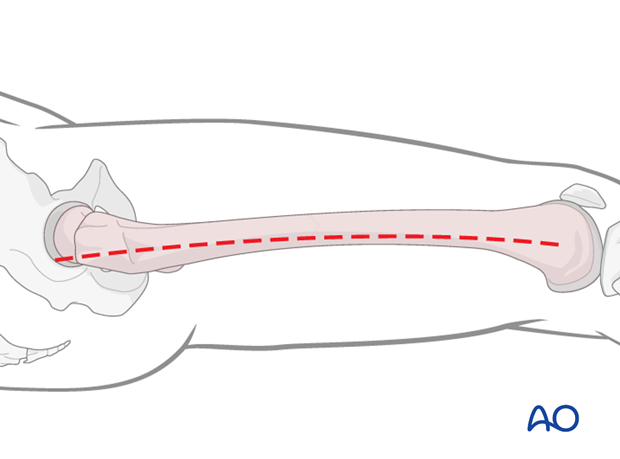
4. Reduction and Fixation
Wedge fixation to a main fragment
As a first step, the wedge fragment is reduced to a main fragment using a pointed reduction forceps and secured in this position by a lag screw. To preserve the vascularity of the wedge fragment, its soft-tissue attachments must not be violated.
Smaller gauge lag screws may be used if needed to avoid comminution of small fragments.
The gliding holes of the lag screws should be in the main fragments and the threaded holes in the wedge fragment, whenever possible.
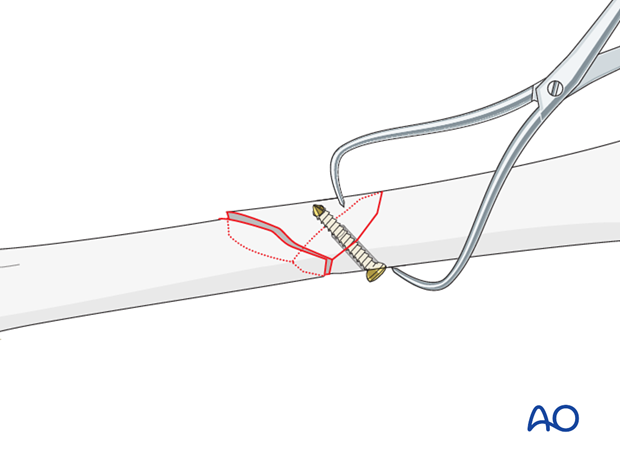
Reduction and plate contouring
After reducing the second main fragment using another pointed forceps, precise contouring of the plate must be undertaken.
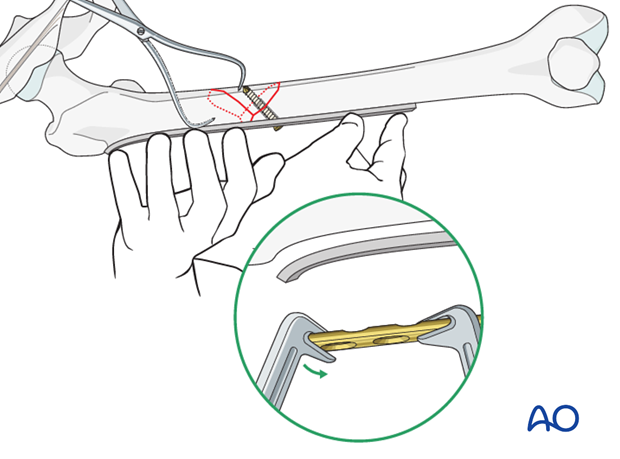
Pitfall: risk of displaced fracture
It is important to contour the plate to fit the bone perfectly so that by tightening the plate screws the fracture is not displaced and the lag screws pulled out.
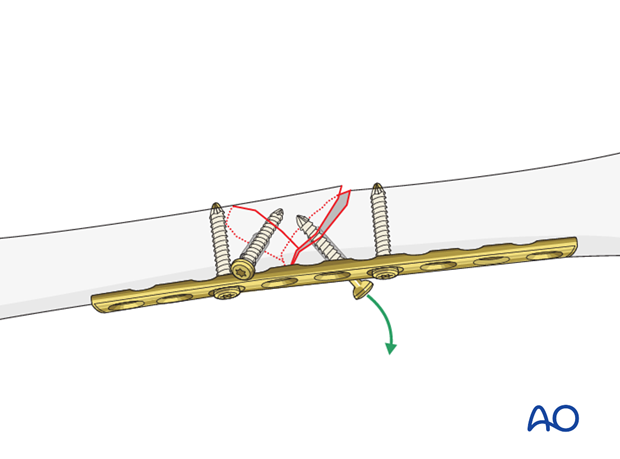
A second lag screw is placed perpendicular to the fracture plane through the plate if fracture configuration allows for it.
The fracture should be handled with caution during plate application.
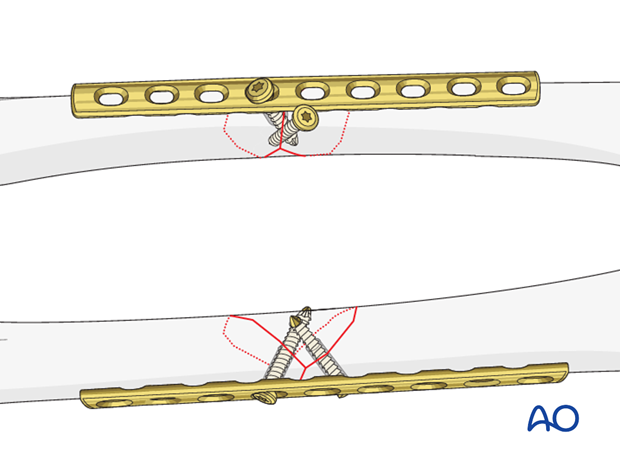
Insertion of bicortical screws
The plate should be fixed to each main fragment with a minimum of three bicortical screws inserted in neutral mode.

5. Aftercare
Compartment syndrome and nerve injury
Close monitoring of the femoral muscle compartments should be carried out especially during the first 48 hours, in order to rule out compartment syndrome.
Postoperative assessment
In all cases in which radiological control has not been used during the procedure, a check x-ray to determine the correct placement of the implant and fracture reduction should be taken within 24 hours.
Functional treatment
Unless there are other injuries or complications, mobilization may be started on postoperative day 1. Static quadriceps exercises with passive range of motion of the knee should be encouraged. If a continuous passive motion device is used, this must be discontinued at regular intervals for the essential static muscle exercises. Afterwards special emphasis should be placed on active knee and hip movement.
Weight bearing
Full weight bearing may be performed with crutches or a walker.
Follow-up
Wound healing should be assessed regularly within the first two weeks. Subsequently a 6 and 12 week clinical and radiological follow-up is usually made. A longer period may be required if the fracture healing is delayed.
Implant removal
Implant removal is not mandatory and should be discussed with the patient, if there are implant-related symptoms after consolidated fracture healing.