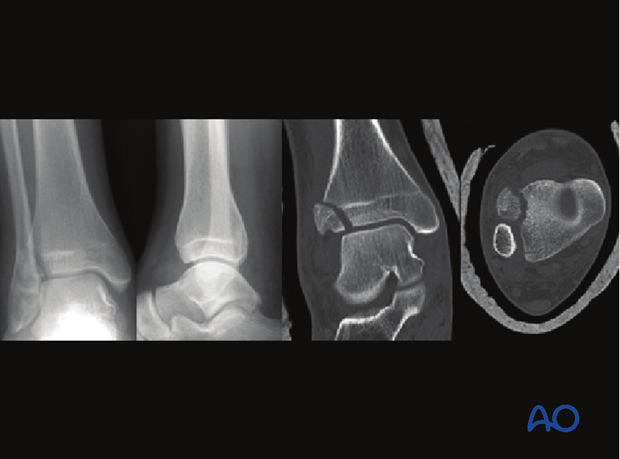
Partial articular, split fracture
These fractures of the distal tibia are usually caused by low energy traumas with rotational or pure bending forces. In some cases, it is difficult or even impossible to distinguish between a malleolar and a pilon fracture (“pilonoid” fracture). The larger the fractured piece is, the more likely it is classified as a pilon fracture.
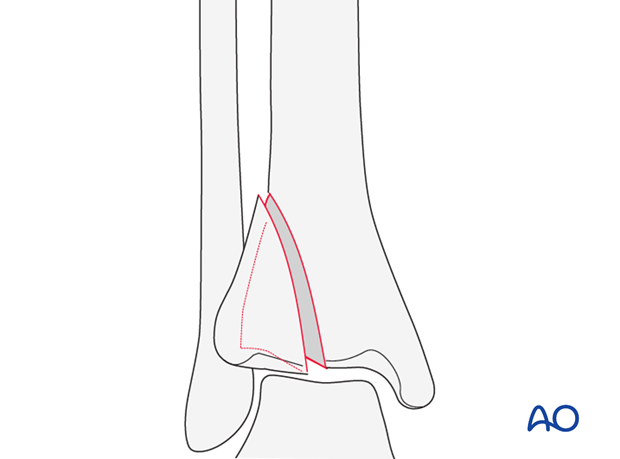
Depending on the mechanism of injury, the split fracture may be:
- In the frontal/coronal plane (classified by AO/OTA as 43B1.1)
- In the sagittal plane (classified by AO/OTA as 43B1.2)
- Fragmentary metaphyseal fracture (classified by AO/OTA as 43B1.3)
Clinical assessment must include the condition of the soft tissues as well as the sensory and motor function of the foot structures. Special attention is given to any signs of a compartment syndrome. Standard AP and lateral x-rays are taken. In case of doubt, CT-scans may be helpful to detect or exclude involvement of the articular surface. For all distal tibia fractures, the fibula must be classified as intact, or fractured into two or multiple fragments. The syndesmotic ligaments usually remain intact. If they are torn or avulsed from the tibia with minor or major fragments (Tillaux-Chaput and Volkmann's Triangle), correct diagnosis and subsequent repair is mandatory. The talofibular ligaments may be torn. The deltoid ligament is nearly always intact. This permits indirect reduction by ligamentotaxis in selected cases.