Assessment of reduction of type C distal tibial pilon fractures
1. Principles
During the different steps of the operation, the reduction has to be assessed repeatedly using visual and fluoroscopic control. Angulation, length of both tibia and fibula, and rotation need to be considered, as does the integrity of the ankle mortise. With complete articular fractures of the distal tibia, both the articular surface and the overall alignment must be addressed. For the joint, careful direct inspection and well positioned radiographs are essential.
Rotation is difficult to assess radiographically. By physical exam, one should confirm rotational symmetry with the opposite side.
There is a considerable variation of anatomy in the ankle region, regarding tibial shaft alignment, length of the fibula in relation to the medial malleolus, and width of the syndesmosis. Therefore, reference should be made to radiographs of the intact opposite side. Intraoperative fluoroscopy of the opposite (uninjured) leg may also be helpful.
Acceptable reduction:
Joint surface: <1 mm intraarticular step and <2 mm intraarticular gap.
Axial alignment: <5º of varus or valgus and <10 degrees of anterior or posterior angulation.
Fibular length and width of syndesmosis: <2 mm difference to the opposite, uninjured side.
2. Articular surface
The tibiotalar joint lines should be parallel on the entire length in the AP as well as in the lateral view.
Larger intraarticular gaps can lead to a widened ankle mortise resulting in a side-to-side unstable talus with early cartilage degeneration and osteoarthritis. Intraarticular steps of more than 1-2 mm will lead to a talar tilt or shift which is demonstrated in the two examples with malreduction below.

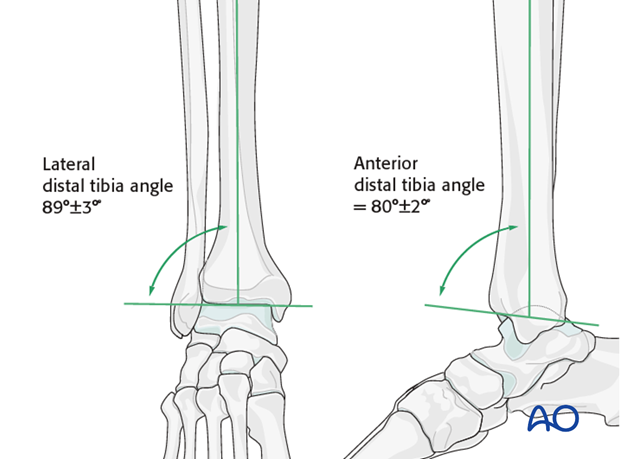
3. Axial alignment
Tibial shaft alignment varies considerably. The medial distal tibia joint angle varies between 88 to 94° in the AP, and the anterior distal tibial joint angle between 78 to 82° in the lateral view. Tibial shaft alignment depends also on the length of the fibula. A shortened fibula usually leads to a valgus malalignment of the tibia due to the mostly intact syndesmotic ligaments.
Therefore, a comminuted fibula is better addressed as last step of the operation to prevent a malposition of the fibula / tibia.
4. Pitfalls - Malreduction
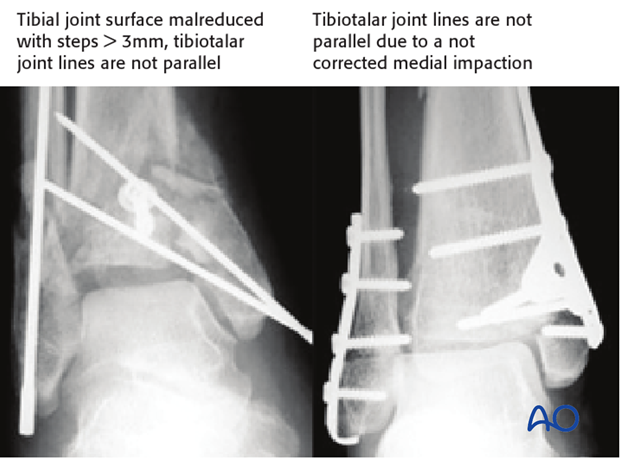
Pitfall: intraarticular gaps
Larger intraarticular gaps can lead to a widened ankle mortise resulting in a side-to-side unstable talus with early cartilage degeneration and osteoarthritis. Intraarticular steps of more than 1-2 mm will lead to a talar tilt or shift.
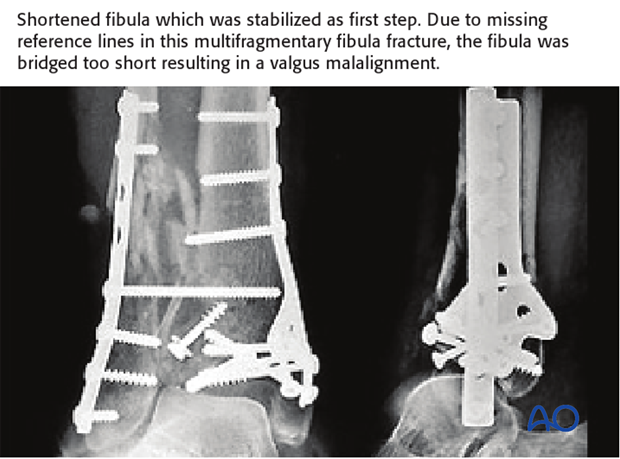
Pitfall: caused by shortened fibula
In the illustrated case, the complex fibular fracture was stabilized as first step. Due to missing reference lines, the fracture was bridged too short, resulting in a valgus malalignment.