Assessment of elbow stability
1. Identification of elbow subluxation or dislocation
Generally, elbow subluxation and dislocation are identified on x-rays taken for pain, deformity, swelling and ecchymosis, or crepitation.
2. Subtle radiographic signs of subluxation
Subluxation can be subtle.
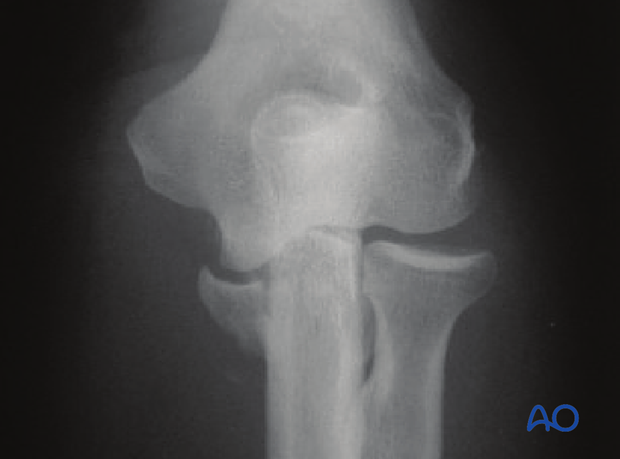
On an AP x-ray, either the medial ulnotrochlear or the radiocapitellar articulation may be gapped more than expected.
The case shows radiocapitellar gapping due to fracture of the coronoid allowing associated ulnohumeral subluxation. In this case, the ulna and radius remain associated. Therefore, there is rotatory subluxation.
On a lateral x-ray, a line bisecting the radial shaft may not pass through the middle of the capitellum, and there may also be a slight gap or “drop sign” in the ulnohumeral joint (arrow).
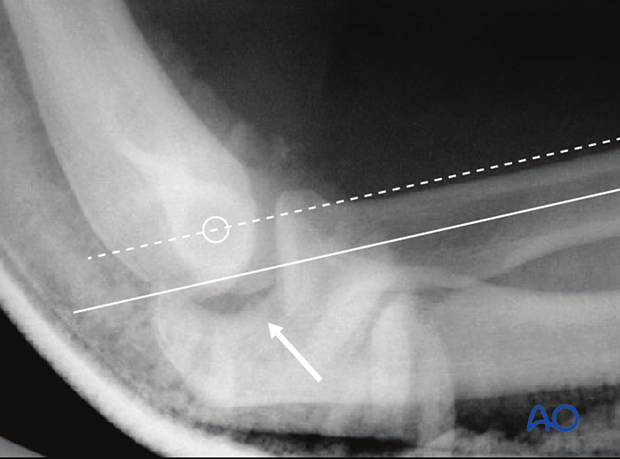
3. After reduction: physical examination for dislocation
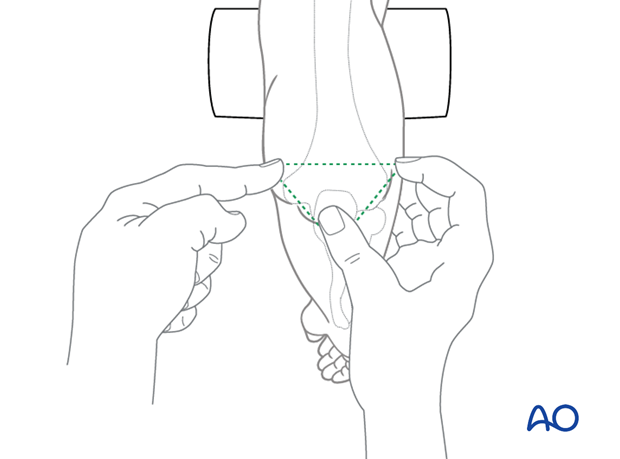
The medial and lateral epicondyles and the tip of the olecranon should form a triangle in the plane parallel to the shaft of the humerus with the elbow flexed. When the elbow is extended, all three points should lie on a straight line.
If the tip of the olecranon is anterior to the plane with the elbow flexed, the elbow is likely dislocated.
4. After reduction: stability check
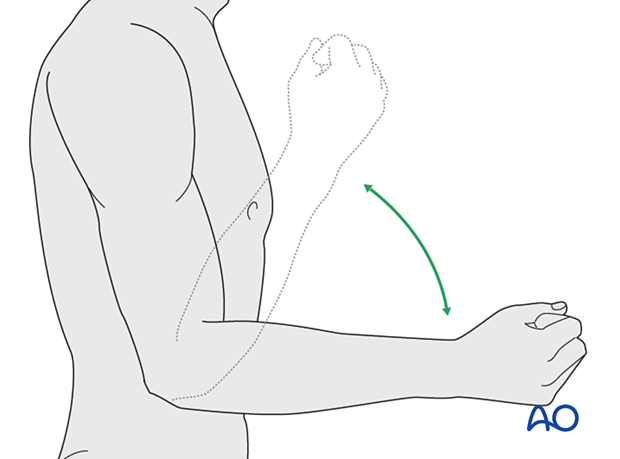
After reduction of simple elbow dislocations, the patient is encouraged to move the elbow, as pain allows, through an arc of flexion from 30° to 90° to confirm that the elbow is located and maintains stability during this movement.
Since most elbow dislocations result in complete or near-complete capsuloligamentous disruption, varus and valgus instability are expected and should not be tested.
5. After surgery: stability check
After surgery, to stabilize the elbow, place the elbow in full gravity extension with the forearm in neutral to see if it subluxates (check with image intensifier) or dislocates (feel for a clunk as it is relocated). There is no need to test an unrepaired medial collateral ligament as we expect valgus instability.














