Open fractures
1. Diagnosis
General considerations
Open fractures of the calcaneus are devastating injuries for patients in the short term as well as in the long term. Frequently, the patients have either been involved in major motor vehicle trauma, or have fallen from considerable heights. They not only have major foot injuries, but frequently many fractures of the long bones as well as spine.
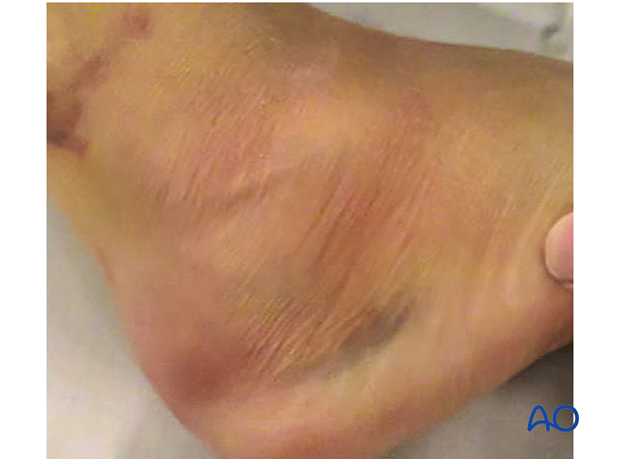
Some open fractures are simple grade 1 injuries, involving only the calcaneus, but others (like in this image) are accompanied by multiple long bone fractures and severe hindfoot injuries.
In patients who have open calcaneal fractures, the surgical team must assess carefully the severity of soft-tissue injury, especially to the heel pad. Occasionally, soft-tissue trauma to the hindfoot heel pad is so bad that primary amputation is the only solution.
As with other severe injuries around the body, the treatment is based upon injuries to the patient, injuries to the limb, and the specific fracture, here an open calcaneal fracture.
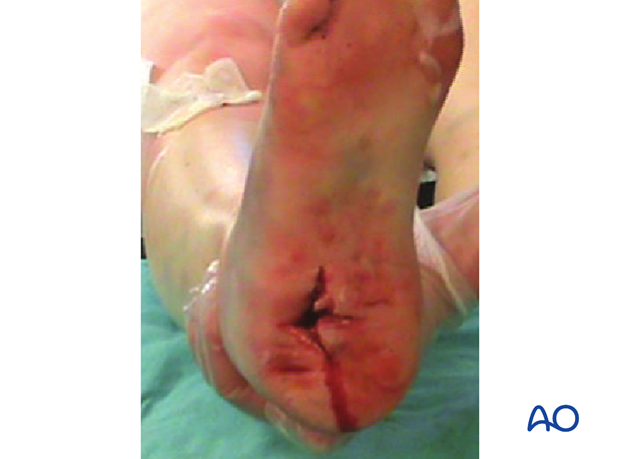
The most common open fracture of the calcaneus occurs on the medial side of the hindfoot. The strongest bone of the calcaneus is on the medial side and with severe trauma, this sharp medial cortical edge will lacerate the medial hindfoot from inside out. This occurs because the sustentaculum and the overlying talus and the rest of the patient descend medially while the os calcis is pushed upwards and laterally. This sudden widening of the foot causes the soft tissues on the medial side to come under tremendous tension until they finally burst.
Emergency management
As in all open injuries, the patient must receive anti-tetanus prophylaxis and appropriate antibiotic coverage. One then proceeds on an emergency basis to an irrigation and debridement.
Once the wounds are clean, temporizing methods such as external fixation, pin fixation, or antibiotic bead pouch technique can be used. If possible, primary closure of the wounds may be considered, but only if the soft-tissue damage is minimal, such as in simple Gustilo grade 1 or 2 injuries.
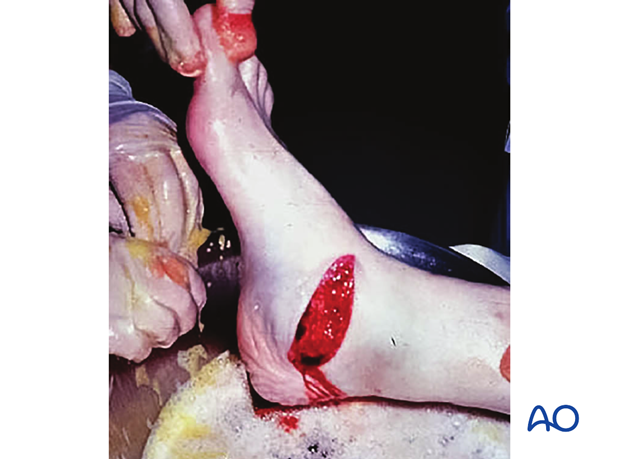
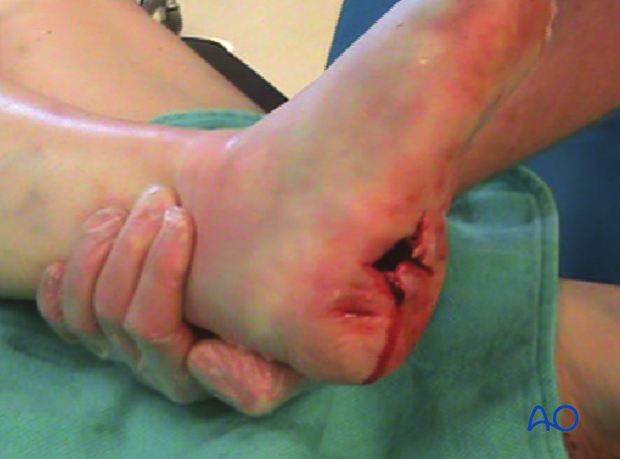
This image shows severe hindfoot trauma after a motor vehicle crash. The surgeon’s finger is in the soft-tissue defect left from the injury. Fortunately, the injury to the heel pad was not too severe as well as the fracture itself, and the situation could be salvaged with appropriate treatment.
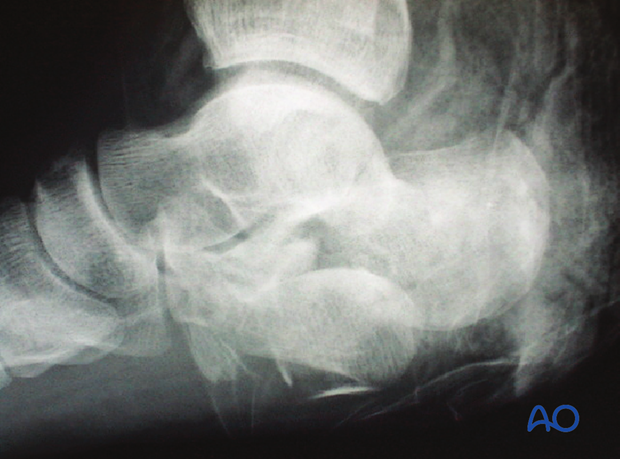
This x-ray image shows an open calcaneal fracture with the posterior facet nearly out through the sole of the foot.
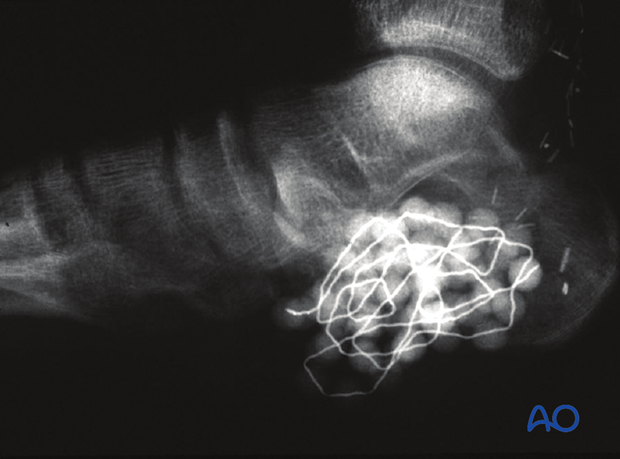
This image shows a severe open calcaneal fracture which was irrigated and debrided, and then the antibiotic beads were implanted as a temporizing measure before definitive fixation was undertaken.
2. Preliminary fixation
In open fractures, the soft-tissue injury is often severe and temporizing measures are necessary before definitive fixation. The temporizing measures refer to methods of achieving stability before definitive treatment can be undertaken. This means achieving stability of the hindfoot. The fracture is irrigated, debrided, reduced and likely stabilized provisionally with percutaneous pins.
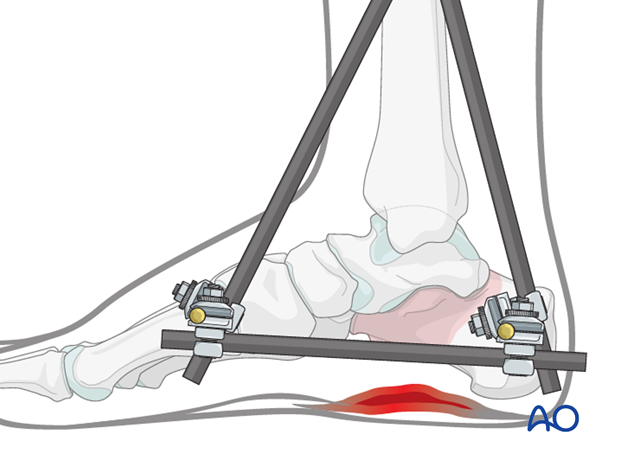
If stability is not enough, one can then add a triangularly-shaped external fixator which will maintain length, height and alignment of the foot and protect the K-wire fixation. In more severe injuries, a primary external fixation may be the first step before any reduction of the fracture is undertaken.
3. Investigations
With severe injury, soft tissue and bone is badly deformed until the limb has been reduced, debrided and preliminarily fixed.
With external fixation or pins in place, x-rays and CT scans demonstrate what surgical procedures need accomplish. Without reduction and preliminary fixation, it is difficult to see exactly what deformities and bone loss needs to be reconstructed. With preliminary fixation in place, exact deformities and bone loss can be estimated. Preplanned definitive surgical fixation is then performed.
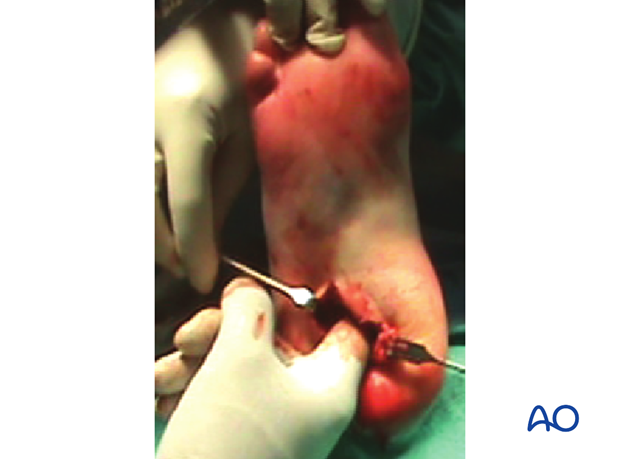
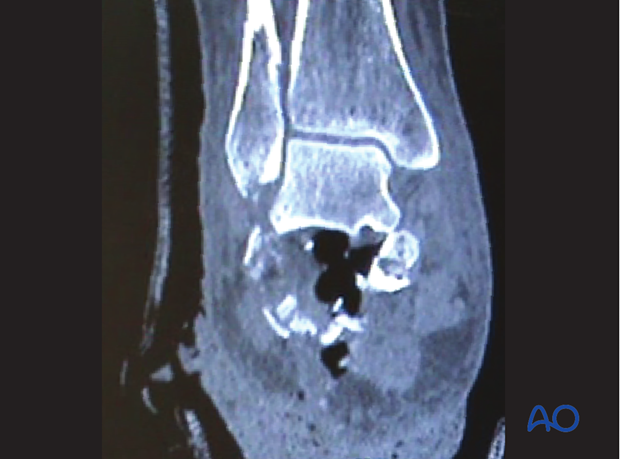
This image demonstrates a severe open calcaneal fracture, now reduced and debrided.
Preoperative planning can take place based on what bone stock is available for definitive fixation.
4. Timing of surgery
Once all risk to the foot has been diminished due to vascular, infective, or soft-tissue problems, definitive surgery can be undertaken. Soft tissues must be amenable to surgery and this is manifest by the “wrinkle sign” in the soft tissues where surgery will take place. The “wrinkle sign” usually will appear by 10-14 days.
With definitive surgery planned, primary calcaneal fixation, or primary subtalar fusion can take place. Bone stock, soft-tissue condition and patient factors will determine definitive hindfoot surgery.
Occasionally, flap procedures are required for soft-tissue deficits combined with definitive hindfoot reconstruction.