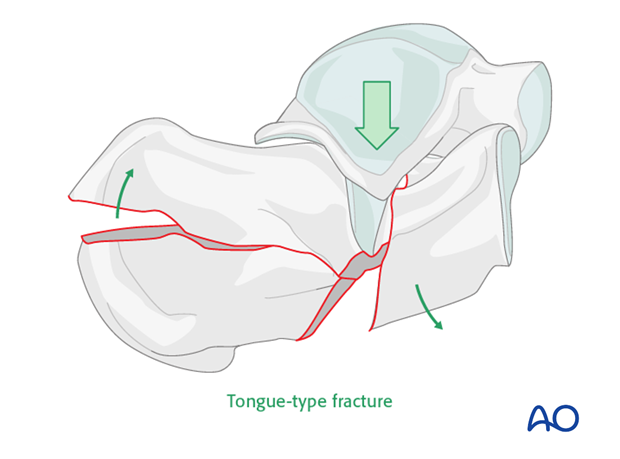
Extreme tongue-type (beak) fracture of the calcaneus body
General considerations
This unusual displaced calcaneal fracture can be intra- or extraarticular. The most important feature of this fracture is its association with significant soft-tissue injury and potential soft-tissue complications. Because of marked disruption of the posterior soft tissues, if it does not present as an open fracture at the time of admission to hospital, the pressure from within on the posterior skin will soon cause it to break down and convert it into an open fracture.
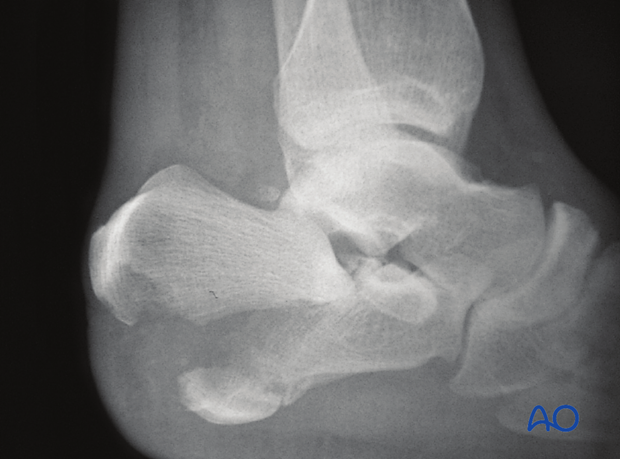
Fractures of the calcaneus are common and account for approximately 60% of tarsal injuries. They result from an axial load and may demonstrate varying severity, type and location of fracture type.
The type of fracture is determined by position of the foot, direction and magnitude of the force and the quality of the bone. Patients will present with pain and swelling, with the inability to bear weight.
Bilateral fractures of the calcaneus occur approximately 10% of the time.
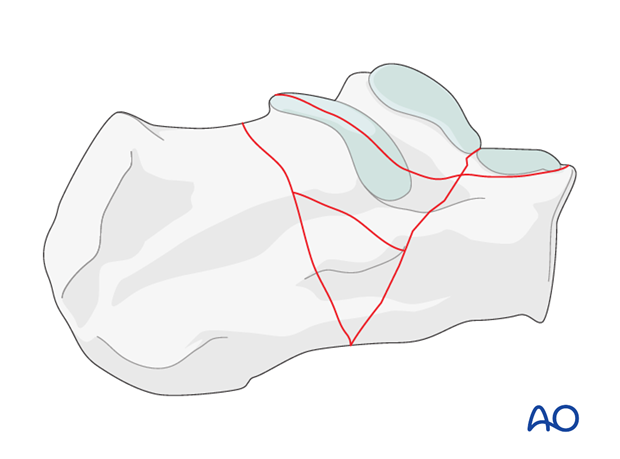
This fracture occurs as a result of the Achilles tendon, which is extremely strong, avulsing a posterior fragment which may be either intra- or extraarticular. Occasionally, it is completely extraarticular but deserves the same operative treatment and reduction. If it is not reduced accurately, weakness from Achilles tendon dysfunction will occur.
This drawing shows an open intraarticular “beak” fracture, requiring urgent operative reduction for reasons of soft-tissue sparing and joint reduction.
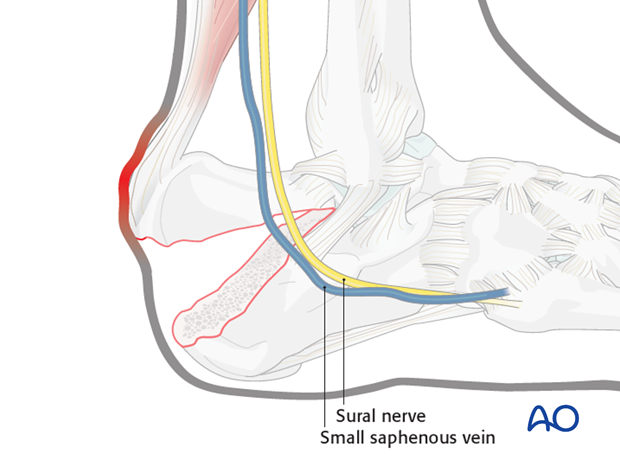
Indications for operative treatment
The surgeon must consider the patient and the fracture when making decisions about treatment.
Operative management is indicated in patients with beak fractures
- with displacement of more than a few millimeters posteriorly
- present or impending posterior soft-tissue compromise
- no medical contraindications to operative care.
If the patient is medically safe for surgery, then immediate operative reduction is indicated to prevent this from becoming an open fracture.
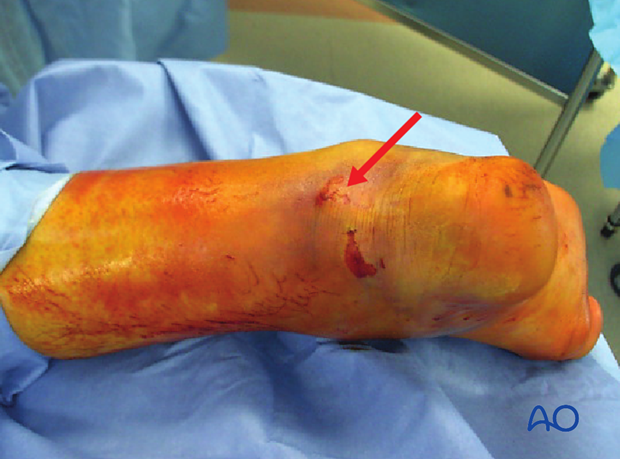
Skin necrosis will occur within 6 h if not reduced.
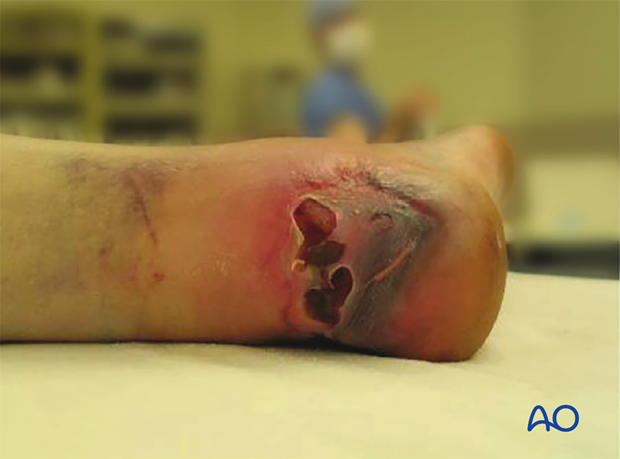
Patient compliance
Few injuries are more devastating or have more long-term impact on a patient’s life. Patient and family education is crucial for enabling the patient to understand the significance of this injury. Important factors such as limb elevation, limb range of motion, smoking cessation and medical wellness (example: diabetic insulin control) allow patients to successfully complete required care pathways.
Radiology
Radiographic views
Lateral ankle x-rays show the dramatic displacement of the posterior tuberosity of the calcaneus. This x-ray will demonstrate also whether or not this fracture extends into the subtalar joint, or is completely extraarticular, leaving the posterior facet uninvolved.

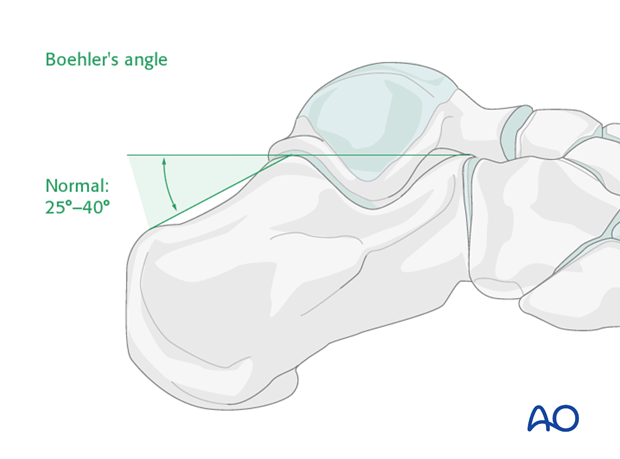
Böhler’s angle
A decrease in Böhler’s angle demonstrates the severity of joint injury and displacement (depression) as measured on the lateral x-ray. The normal angle is 25 degrees to 40 degrees. If this angle remains above 15 degrees, nonoperative care can be suggested.
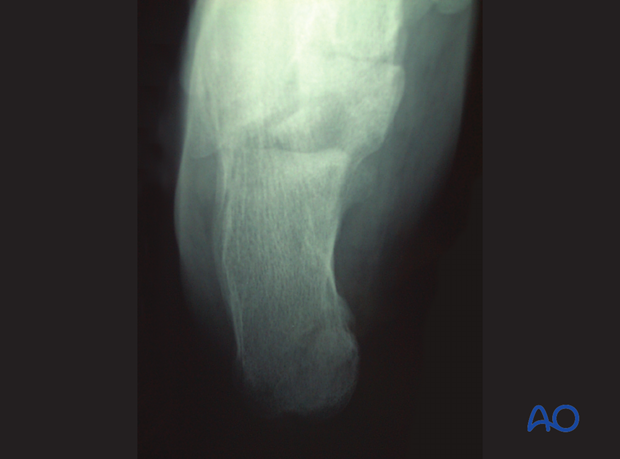
Axial view
This view is difficult to interpret because the displaced tuberosity hides the injury as it is in the plane of displacement.
Computed tomography
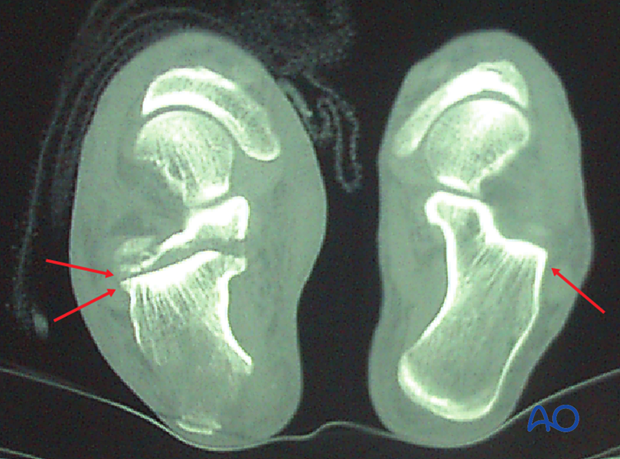
If there is time before skin compromise, a CT will be helpful to discern the exact amount of joint displacement. This CT shows a normal foot and an axial cut of a patient with a beak fracture, showing the double line of the articular surface which demonstrates the articular split.
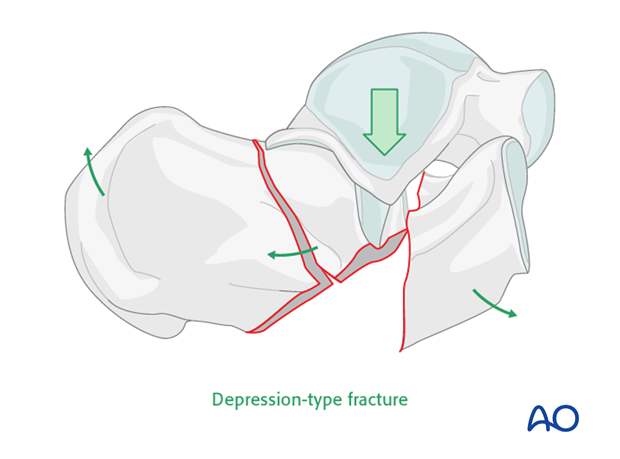
Essex-Lopresti classification
This classification was first published in 1951-52*. It is useful in separating the joint fractures into two types. We see first an example of a “joint depression” and in the lower image a “tongue type”. The joint depression is notorious for the degree of joint involvement and displacement.
* Essex-Lopresti P. The mechanism, reduction technique, and results in fractures of the os calcis, 1951-52. Br J Surg. 1952 Mar;39(157):395-419
Note that in the tongue-type fracture the fracture exits posteriorly, splitting the posterior portion into two. Different fixation techniques are required in order to reduce and stabilize this deformity.