MIO - K-wire fixation (tongue type)
1. Principles
General indications for surgery
Some patients with fractures are obvious surgical candidates. Others present with medical contraindications to open surgery, or local soft-tissue contraindications to open surgery. Examples would be older diabetics, or medically unwell patients who have a significant calcaneal deformity but have a contraindication to a more invasive procedure.

Choice of treatment method
Younger patients in good health, good soft tissues with uncompromised healing potential and significantly displaced fractures have an undisputed indication to open reduction and internal fixation. At the other end of the spectrum are patients who have significant co-morbidities, or who are elderly, or who have risk factors, like smoking, are considered to be too high a risk for a formal open reduction and internal fixation.
It is in this latter patient group that minimally invasive techniques are most useful.

Fracture indications for minimally invasive surgical techniques
When a fracture changes foot morphology, normal gait would be compromised, therefore surgery is indicated in order to restore normal anatomy and normal biomechanical relationships. Such restoration leads to normal gait.
If the fracture is extraarticular, absolutely anatomical reduction is not necessary because we are not dealing with an articular surface. In these situations, indirect reduction techniques and minimally invasive surgical stabilization methods can be used. One can employ these techniques also in patients in whom, under normal circumstances, an open reduction could be performed, but who are unwell, or have other risk factors which mitigate against full open surgery.
A basic principle is always to obtain accurate joint reductions. However, medical contraindications are of greater importance, as indicated by an infection rate in calcaneal fracture surgery upwards of 15% in diabetics, older unwell patients, or heavy smokers.
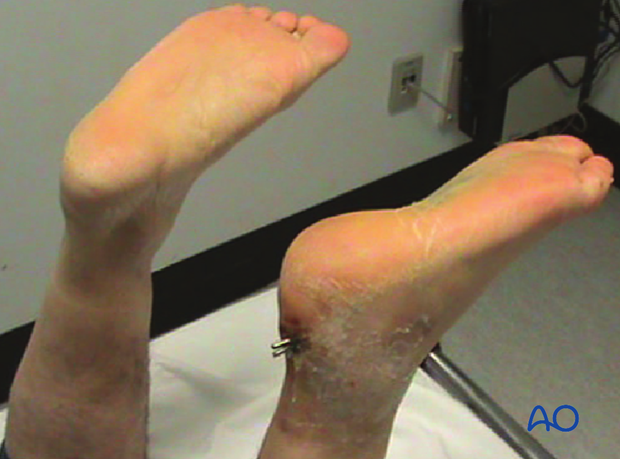
This image shows a 63-year old diabetic with a displaced intraarticular tongue-type calcaneal fracture.
2. Fracture investigation
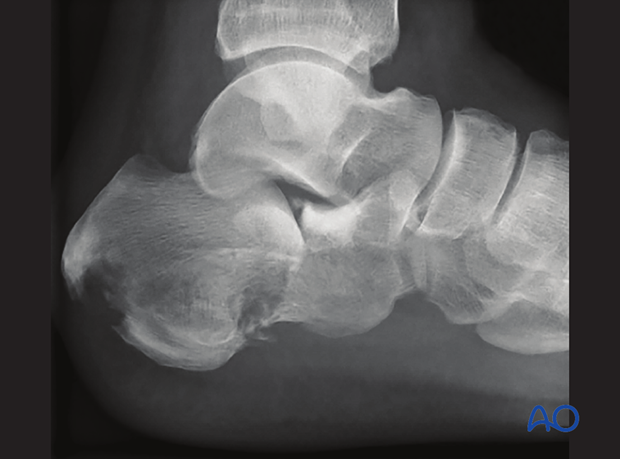
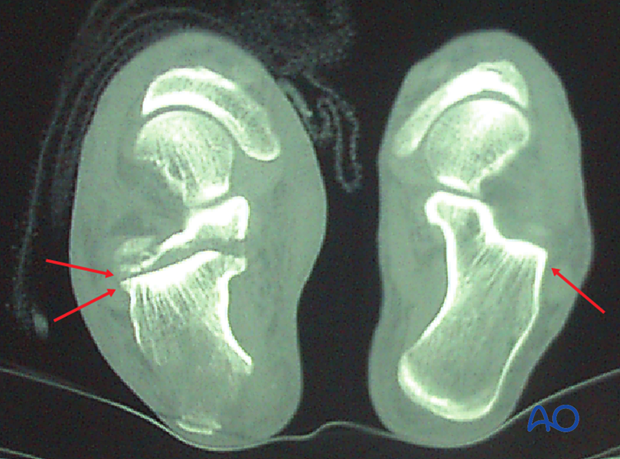
The CT of this tongue-type intraarticular fracture indicates that this case is perfect for percutaneous pin fixation. It is one large posterior facet piece with an intact anterior calcaneal tuberosity. It also demonstrates that the posterior facet is impacted about 15 mm and would benefit greatly from a reduction maneuver. If this patient was not a candidate for open reduction, this CT scan helps determine that minimal invasive techniques would be a nice solution for the problem.
3. Approach
For this procedure a minimally invasive posterior approach may be used.
4. Reduction
Preparation
With the patient in the lateral position, with image intensifier control, one inserts a Steinmann pin into the posterior superior portion of the calcaneal tuberosity and directs the pin forwards and downwards to avoid penetrating into the subtalar joint.
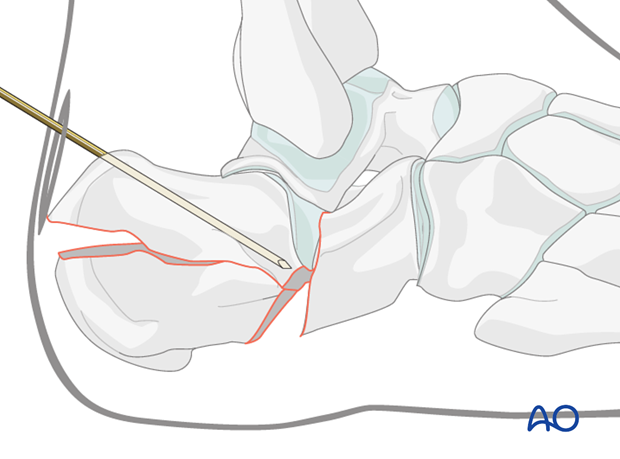
Elevate depression
Now, using the Gissane reduction maneuver, the Steinmann pin is forcibly pushed downwards so as to elevate its tip.
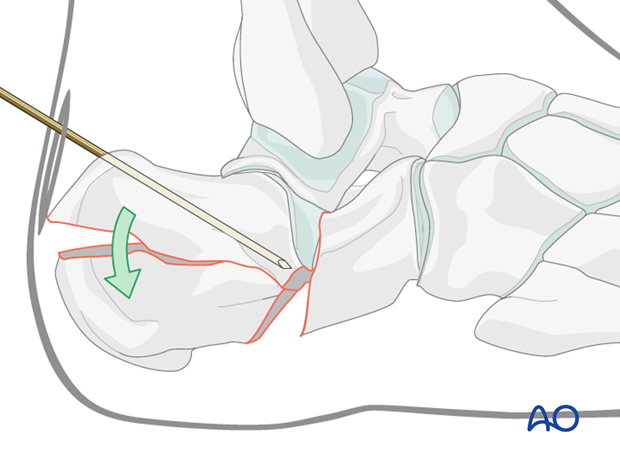
The pin is then advanced across the fracture into the anterior undisplaced portion of the os calcis. This is done only when the articular surface is reduced.
When difficulty is encountered in reducing the fracture by this maneuver, one can make a small incision below the anterior corner and then insert an elevator and pry upwards to reduce the fragment. Once reduced, the pin would be advanced anteriorly.
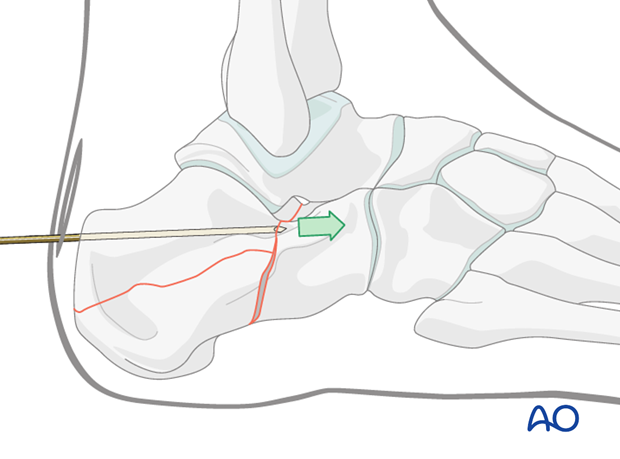
Maintenance of reduction
The single large pin is advanced into the anterior calcaneus under image intensification.
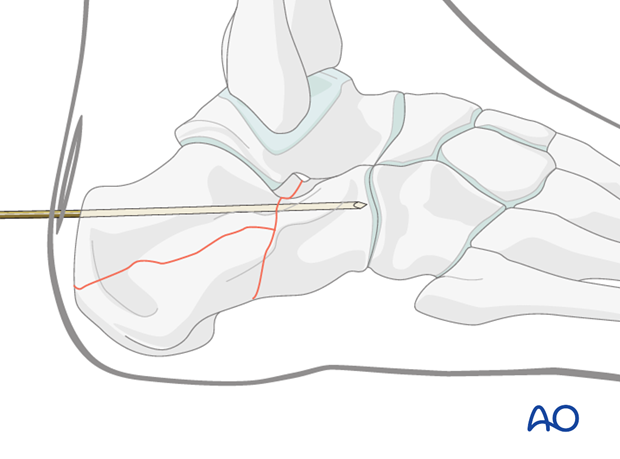
More fixation may supplement the single large pin.
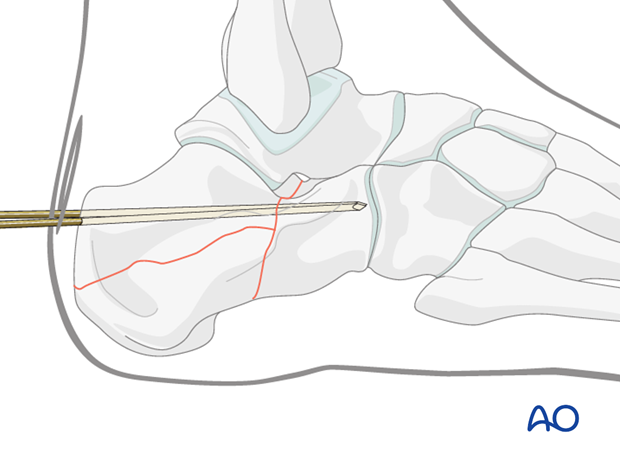
5. Fixation
In this elderly diabetic, minimally invasive surgery allowed for accurate joint reduction and correction of the bone morphology. Stability was achieved with percutaneous pins.
6. Aftertreatment
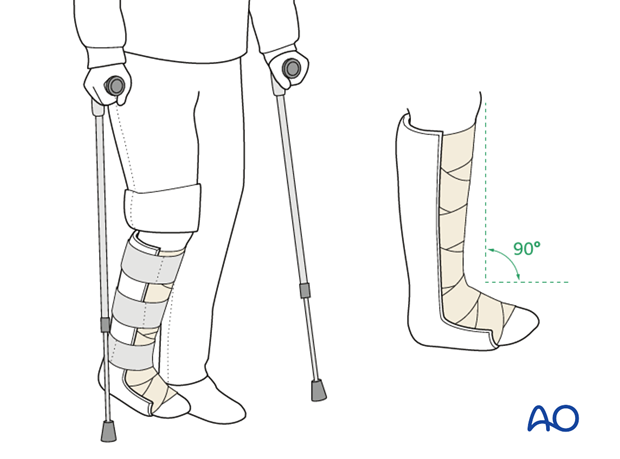
Initially, the patient’s foot and ankle are kept in a well-padded posterior splint that maintains the foot in a neutral position.
The leg should be elevated intermittently through the first number of weeks. The ankle joint is put through range-of-motion exercises as soon as possible, usually by 2-5 days. Normal bathing and washing prevents pin-track infections.
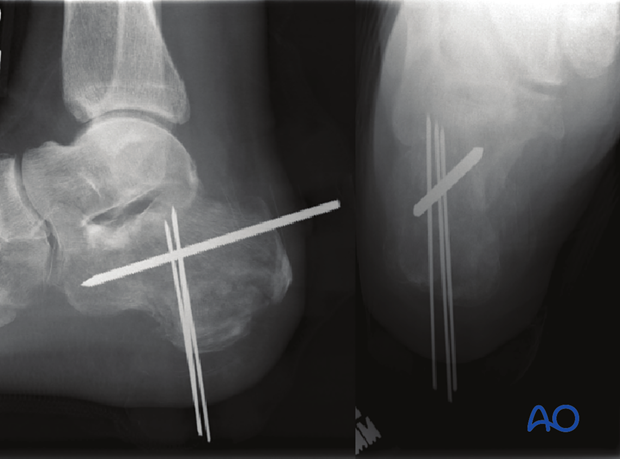
Pin removal is not before 6 weeks. Image at left shows pins at 6 weeks before removal.
Weight bearing is delayed until pin removal after 6 weeks.
Radiography including lateral and axial views is obtained at 6,12 and 26 weeks.