Treatment modalities
1. Introduction
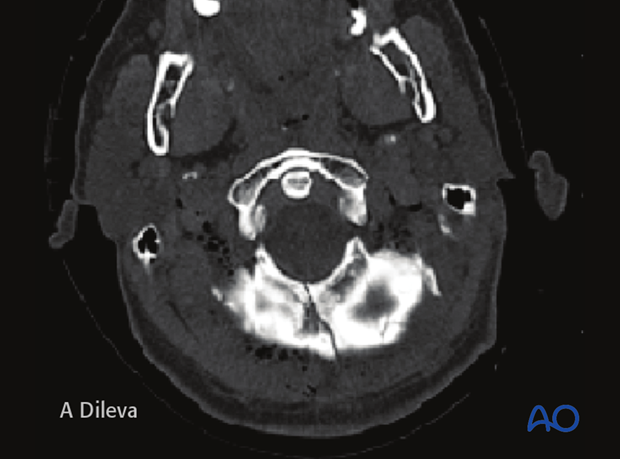
Fractures of the posterior skull base are rare and occur in only 5% of all skull base fractures. However, they require special attention because of their high mortality rate.
The three most important complications associated with posterior skull base fractures are:
- Brain stem compression due to mass effect (eg, epidural hematoma, or intracerebellar hematoma)
- Acute hydrocephalus due to occlusion of the 4th ventricle
- Craniocervical instability due to occipital condylar fractures
2. Approach
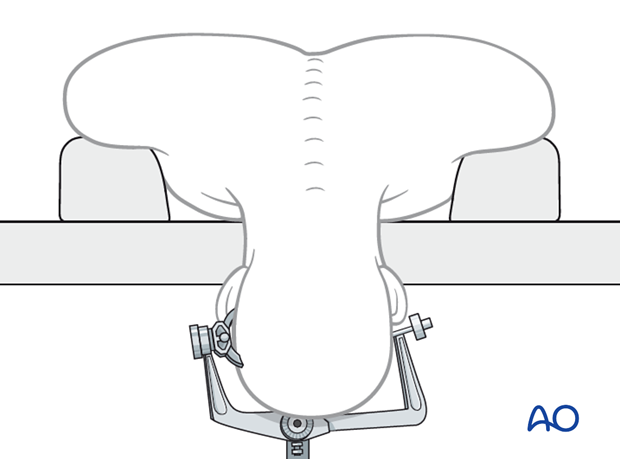
For this procedure the posterior skull base approach is normally used.
3. Treatment modalities in case of mass lesion of the posterior fossa
Epidural hematoma
Posterior fossa fractures associated with epidural hematoma need a big enough craniotomy to expose all of the bleeding areas. Use typical burr holes (usually only one is necessary).
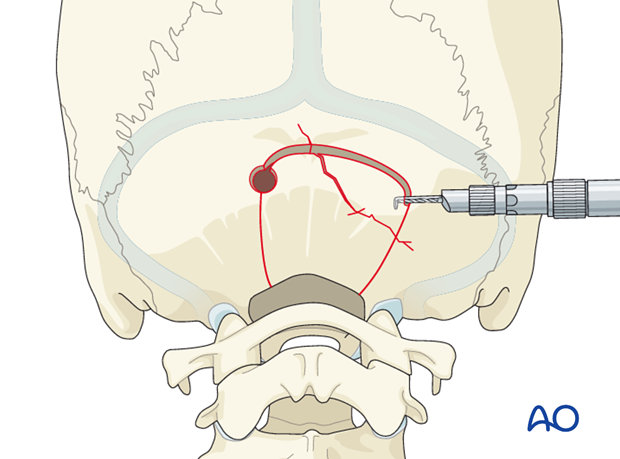
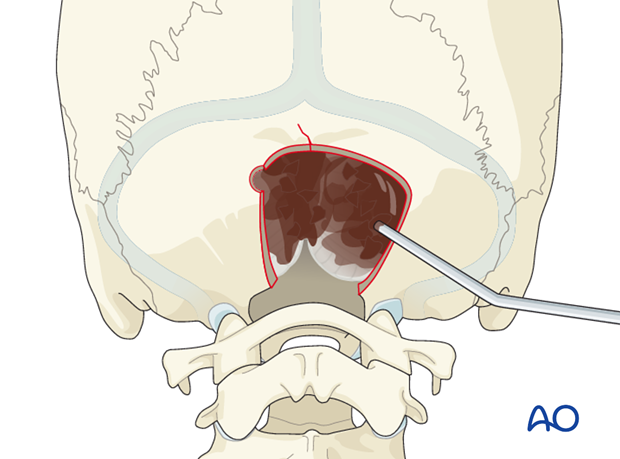
The epidural mass lesion is explored and removed by using a suction device and dissectors. The dura has to be examined and, in case of laceration, it is repaired in a water-tight fashion.
In case of significant brain swelling, the bone flap is not replaced at this time. In those cases the bone flap is stored in a freezer (-72°C) and replaced at the time of a second procedure, usually 3-6 months after primary surgery.
When there is no swelling, the bone flap is replaced and fixed in the primary surgery.
Subdural hematoma
In case of subdural hematoma of the posterior fossa, the dura is opened directly above the hematoma in an X-shaped incision.
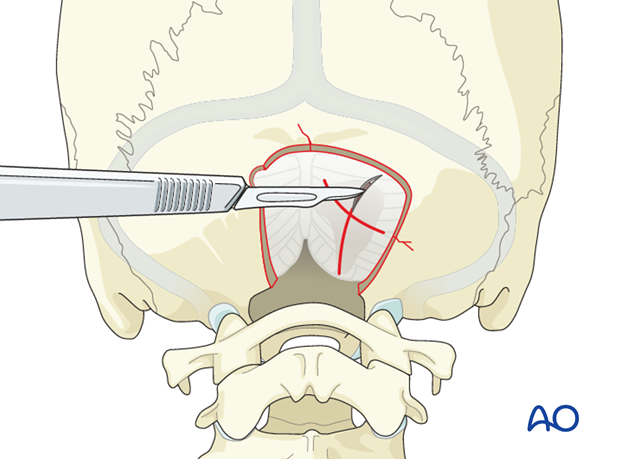
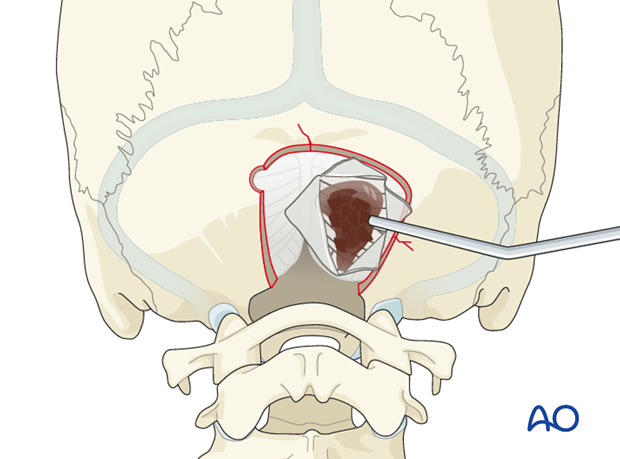
The subdural hematoma is evacuated using suction and dissectors taking care to avoid injury to the cerebellar cortex.
When the swelling is severe, an extended duraplasty is performed and the bone flap is not replaced at this time.
4. Aftercare following open management of skull base fractures
General postoperative care
- Intensive care 24 hours
- Hospitalization 5-8 days (to rule out reoccurrence of CSF leak)
- The use of broad-spectrum antibiotics during and after the procedure for the next 5-7 days is recommended.
- Radiologic control examinations are performed routinely the next day after leaving the intensive care unit.
- Patient follow-up after discharge. The patient is seen 4 weeks after, and if necessary, for the long-term follow-up a year postoperatively.













