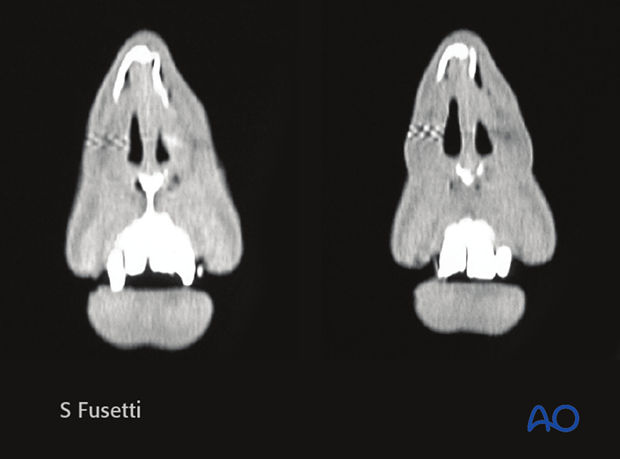
Examination of patients with nasal bone fractures
Diagnosis should be made with history of the patient, physical examination and imaging. The direction and strength of the impact should be noted. Preexisting nasal or septal deformities should also be considered. A history of nasal bleeding may indicate a mucosal laceration. Skin laceration over the nasal area may guide fracture diagnosis to the specific anatomical area.
Physical examination
The external nose should be examined via bimanual digital palpation.
Swelling may preclude proper assessment.
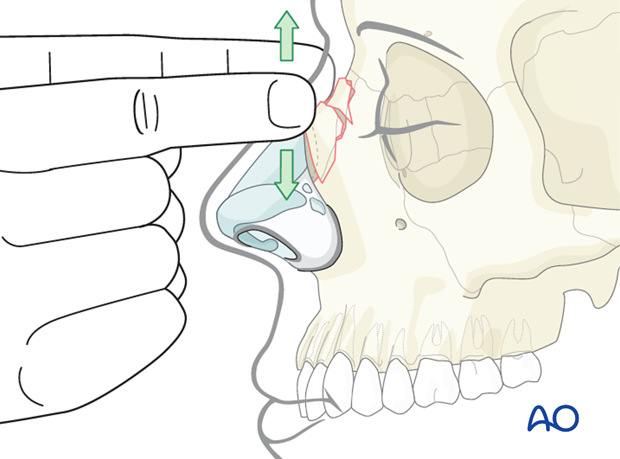
Steps, humps, and crepitus are all signs of nasal bone fractures.
Ecchymosis and/or the presence of a hematoma should also be noted.
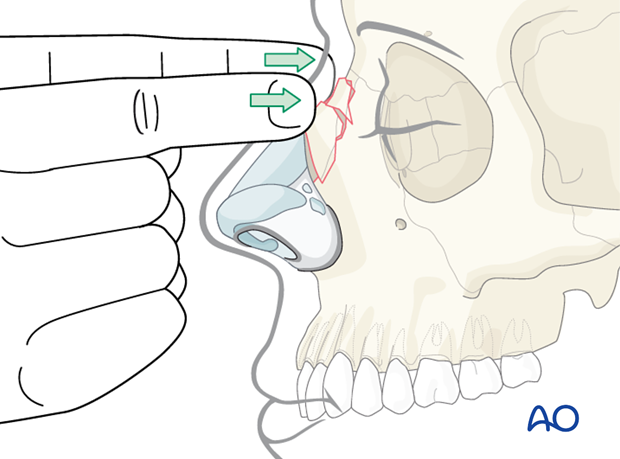
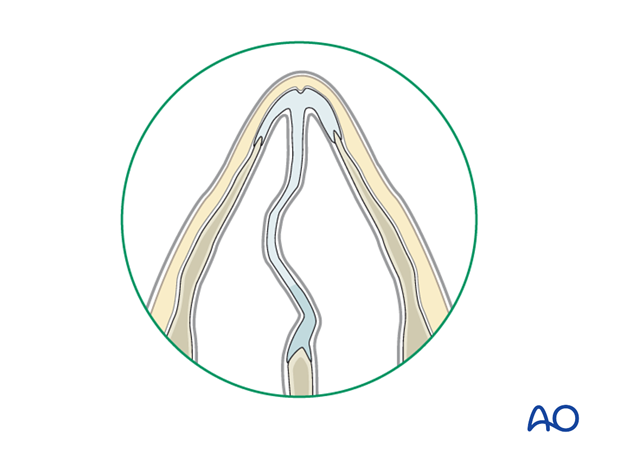
Intranasal anatomy should be assed using a nasal speculum, looking for a septal deviation, mucosal laceration and/or septal hematoma.
The presence of a significant septal hematoma requires immediate drainage.
Hematoma is diagnosed as follows:
- The main symptom is severe nasal obstruction
- On examination the septum appears swollen and boggy
- The swollen area should be palpated with a cotton-tipped applicator. If a hematoma is present it should be compressible.
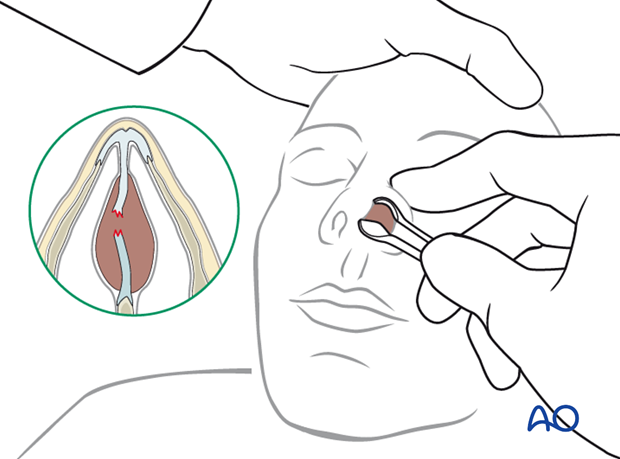
Preexisting septal deviation should be differentiated from traumatic fracture to the septum, if possible.
Imaging
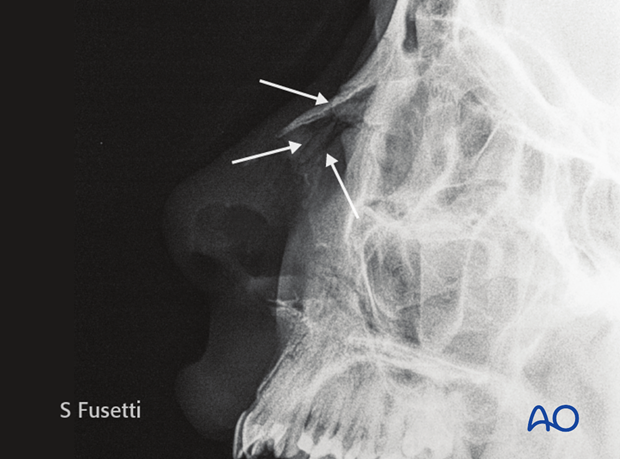
Most surgeons find plain films of the nose to be unhelpful.
The greatest weakness of plain films is their inability to assess the injury for correct management. The management of nasal bone fractures is based primarily on clinical assessment of appearance and function.
When CT scans are performed due to associated facial bone fractures they can be helpful to make a more accurate diagnosis of nasal bone fractures.