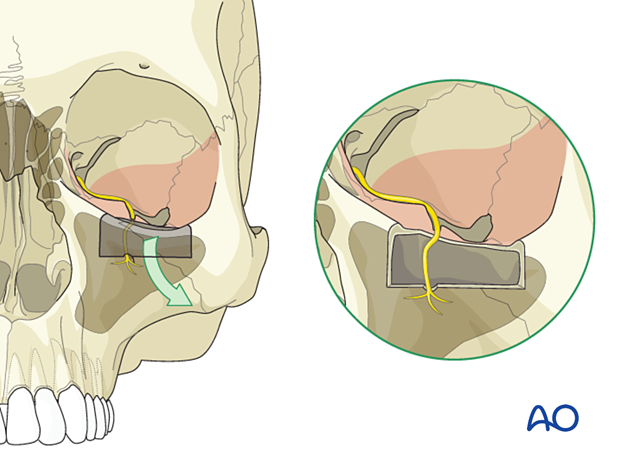
Adjunctive access procedures (orbitotomies)
1. Exposure of lateral orbital wall via temporal/infratemporal fossa approach
Cases of severe fragmentation/displacement of the zygomaticosphenoid junction involving the greater sphenoid wing result in the loss of this landmark of the skull base. Restoration of the posterior lateral orbit and the transition into the orbital apex can then be performed via a temporal/infratemporal fossa approach.
This approach risks temporal hollowing, caused by muscle and fat atrophy, which is challenging to correct. Therefore, an intraorbital approach through a coronal incision is preferred.
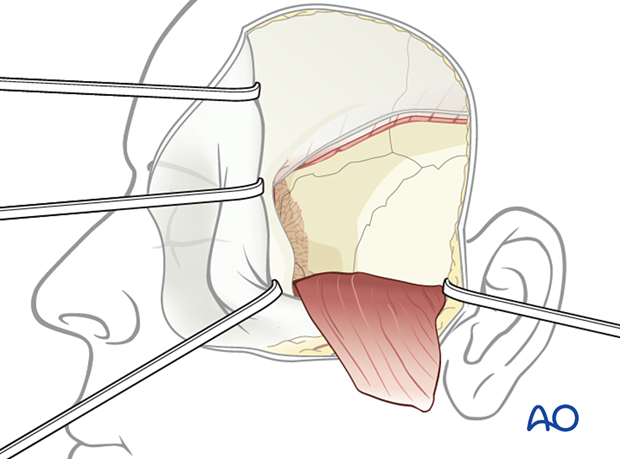
The zygoma and lateral wall of the orbit are exposed through a coronal approach.
The temporalis muscle is incised 1–1.5 cm below the superior temporal line leaving a cuff of muscle superiorly so that the muscle can be resutured to itself for a secure and aligned soft tissue closure.
Two approaches are possible: a limited approach and an extended approach. A limited approach through an upside down L-shaped incision in the muscle can be used for limited exposures. The muscle can be dissected leaving a small cuff of muscle attached to the frontal process of the zygoma for secure resuturing of soft tissue.
In the extended approach the entire temporal bone can be exposed by extending the incision posteriorly. A vertical incision in the preauricular area can be designed to avoid the temporal vessels and the entire muscle then becomes a vascularized flap with the incision extending vertically inferiorly to the zygomatic arch. The lateral orbital wall, temporal bone, and pterion are all exposed by the extended incision.
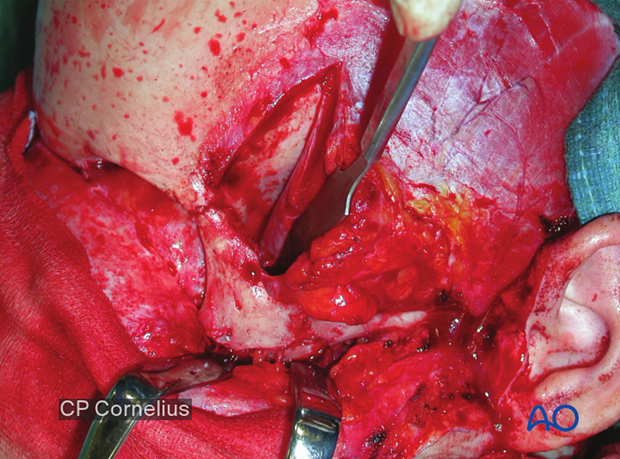
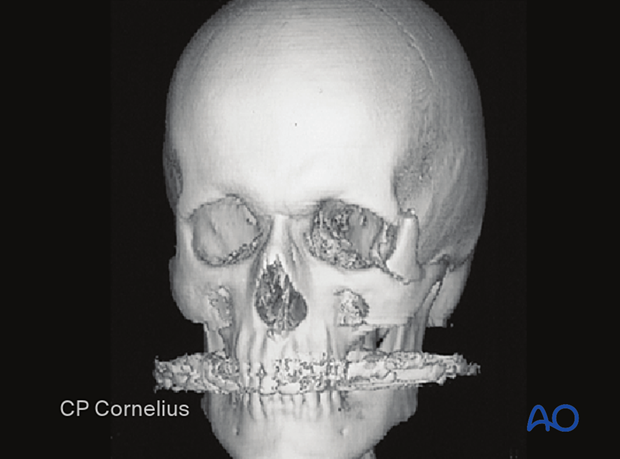
Clinical case demonstrating the exposure of the lateral orbital wall via a temporal/infratemporal approach.
The temporalis muscle is elevated below the superior temporal line and retracted to expose the lateral orbital wall.
In most cases, the extensive approach is not necessary for provision of orbital exposure alone.
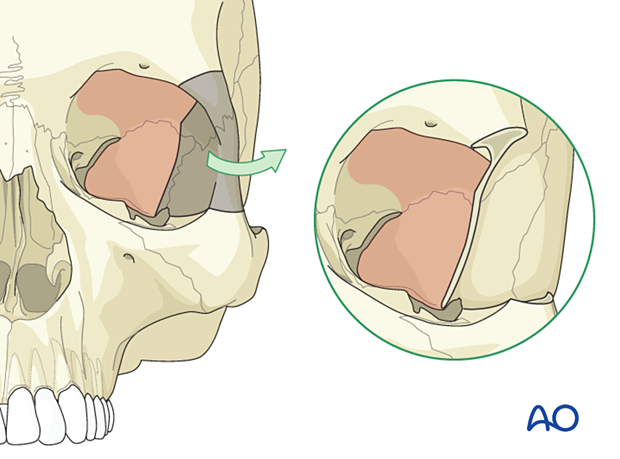
2. Lateral marginotomy
Lateral, superior, and inferior marginotomies facilitate exposure of the posterior orbit.
Temporary removal of the lateral orbital rim and the adjacent orbital wall is rarely required for the reduction and fixation of orbital fractures but can be a useful maneuver to decompress a retrobulbar hemorrhage with compartmentalization inside the periorbital sac. The preferred maneuver for the decompression of an infraorbital hemorrhage is a complete lateral canthotomy followed by release of the lower lid and the septum from the canthus. Removal of reconstruction materials, such as those used in the orbital floor reconstruction and removal of hardware used in the reduction adds further significant decompression, allowing the bone fragments to decompress externally.
The CT scan is from a case with an orbital floor fracture, where loss of vision was fully reversed after the osteotomy and outfracture of the lateral wall. In general, the specific cause of visual loss is attended to first, such as optic canal decompression, and further manipulation is then pursued during secondary maneuvers to add further release.
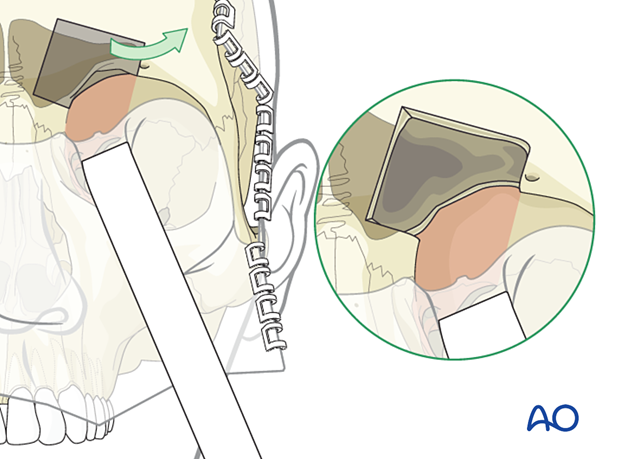
3. Superomedial marginotomy
The superior marginotomy removes portions of the superior orbital rim, such as the superomedial portion. This includes the anterior wall of the frontal sinus and detaches the superior oblique just inside the superior orbital rim. The supraorbital nerve must be released from its foramen if present. The lateral cut goes beyond the midpoint of the roof, generally encompassing the lateral recess of the frontal sinus which is highly variable. This approach, which includes a portion of the upper medial orbital rim, provides subcranial access to the orbital apex, the frontoethmoidal transition, and the entire medial orbital wall.
In particular, the visualization along the medial wall is greatly facilitated by removing the medial superior and upper rim through this subcranial extension.
4. Inferior marginotomy
The inferior marginotomy is indicated for the secondary repair of challenging fractures where the orbital soft tissue has significantly displaced into the maxillary sinus. Removal of the rim and the anterior wall of the upper maxillary sinus provides wide simultaneous access to the lower orbit and upper maxillary sinus and the lower circumference of the mid and posterior orbital floor. This exposure facilitates dissection and elevation of the periorbita from scarred orbital bone fragments and soft tissue which has prolapsed into the maxillary sinus.
Moreover, the infraorbital nerve can be explored, to allow performance of an external neurolysis.