Fibula osteocutaneous flap harvest
1. Introduction
Design of flap
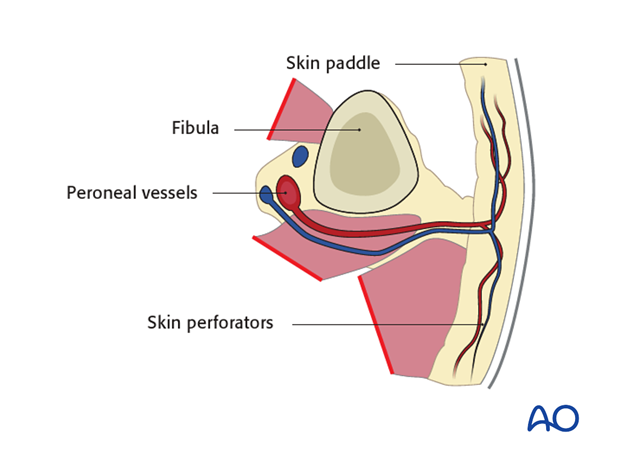
The harvested flap should include:
- Skin paddle
- the fibula
- the skin perforators
- the peroneal vessels
Longitudinally the flap should be harvested long enough to complete the reconstruction.
The skin flap can be harvested to a length varying from 10-30 cm and a width of 4-14 cm depending on the size of the patient.
The bone can be harvest to a length of 6 - 26 cm depending on the size of the patient.
Anatomy
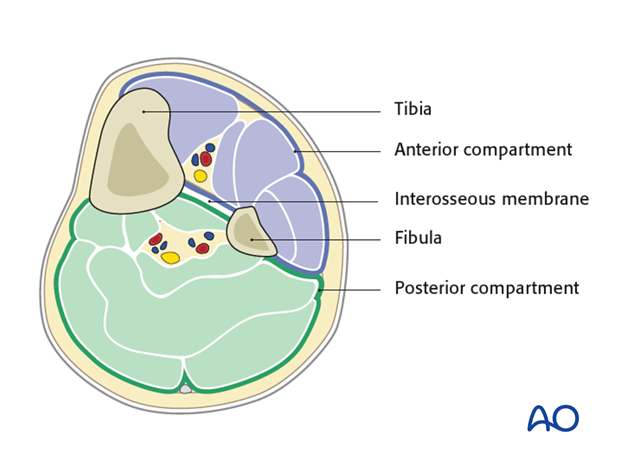
The cross section of the lower limb can be divided into two main compartments:
- Anterior compartment
- Anterior
- Lateral
- Posterior compartment
These compartments are divided by the interosseus membrane between the tibia and the fibula.
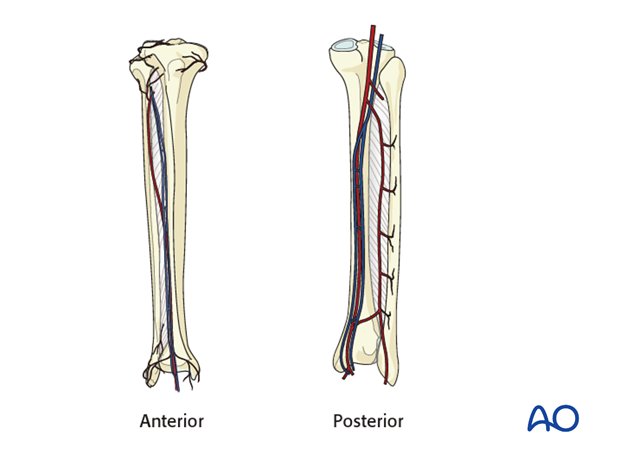
The vascular pedicle
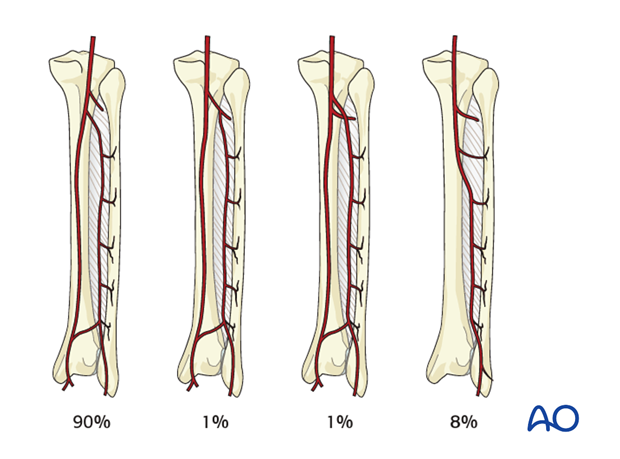
The vascular pedicle consists of the peroneal artery (1.0 -2.3 mm diameter) and venae comitantes (2-4 mm).
The main anatomical structures are shown from both an anterior and posterior view.
The skin perforators originate from the peroneal artery, pass along the lateral septum located at the posterior border of the fibula and supplies the lateral skin of the lower limb. The majority of the perforators are located at the inferomedial part of the fibula
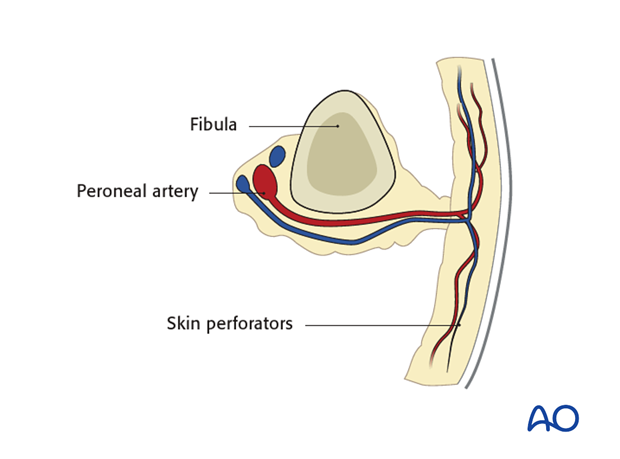
The illustration to the left show the most common variation of the peroneal artery.
The use of a fibular free flap is contraindicated in patients with inadequate anterior or posterior tibia vessels in order to avoid compromise of the blood supply to the foot.
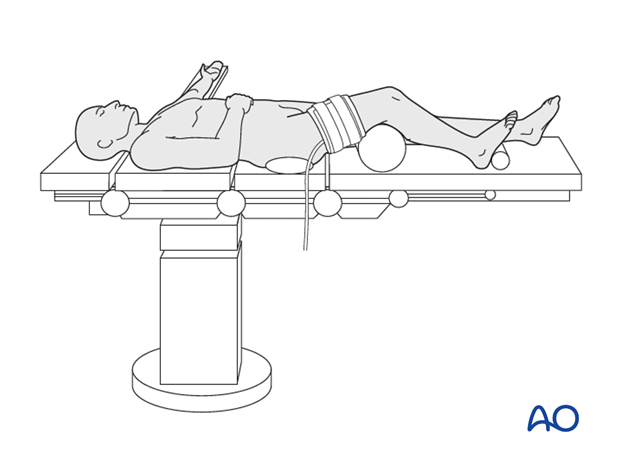
2. Flap harvest
If a tourniquet is used, it is placed at the middle of the thigh and inflated (up to 90 minutes) to twice the systolic pressure.
The fibular head and the lateral malleolus are marked. An outline of the skin incision is then inscribed using a surgical marker.
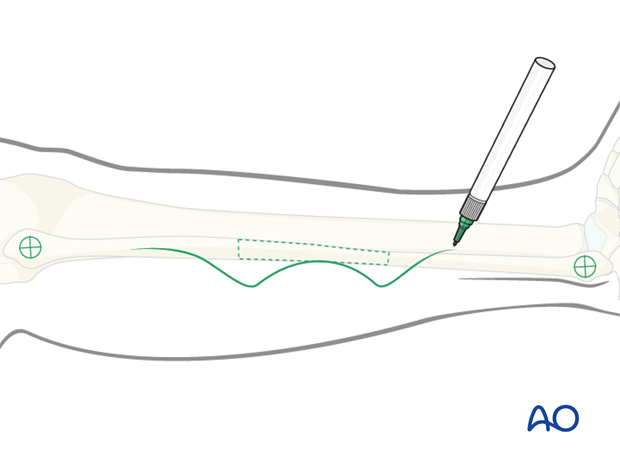
The incision is outlined starting 2 cm inferior to the fibular head (to avoid damage to the common peroneal nerve).
The shape of the incision may be curved or a straight line. This author prefers a S-shaped incision.
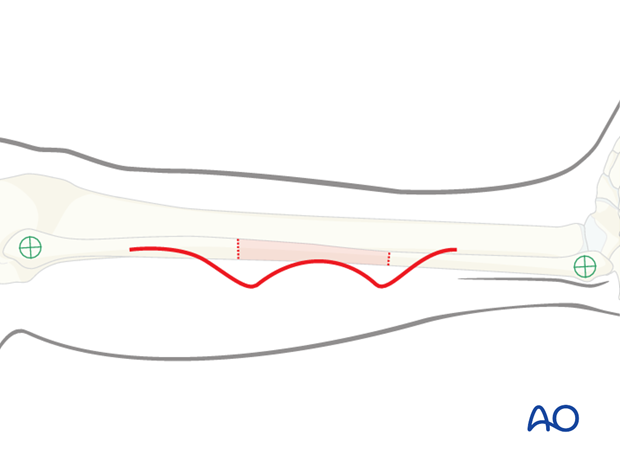
Anterior compartment dissection
The skin is incised down to the deep fascia of the skin and a subfacial elevation of the skin is made to identify the perforators to the skin.
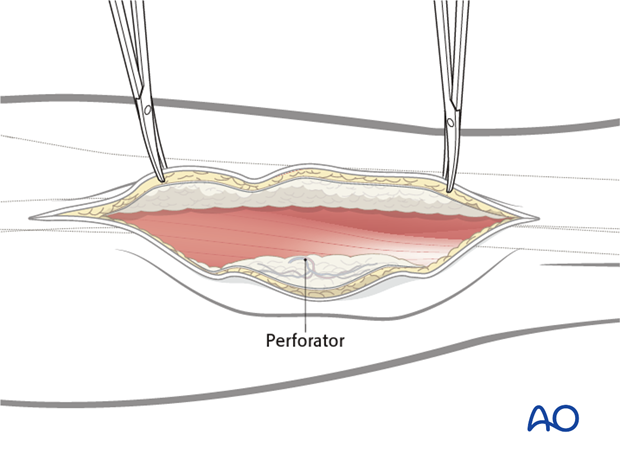
Once the perforators are identified, the skin paddle is outlined, centered over the perforators.
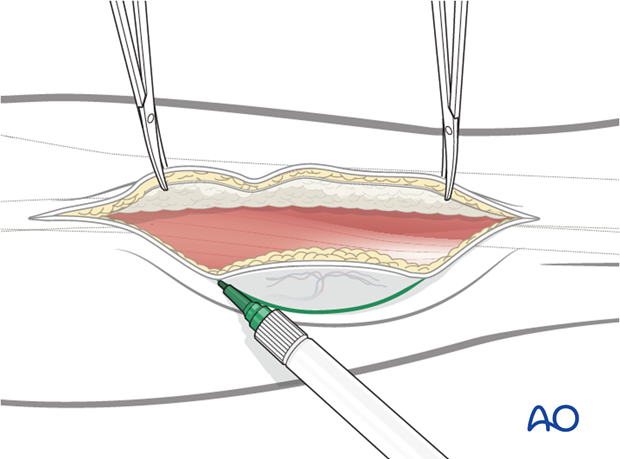
The peroneal muscles are elevated from the periosteum of the fibula and retracted anteriorly to expose the fibular bone. Care should be taken to preserve the periosteum over the bone, especially in the area of the perforator.
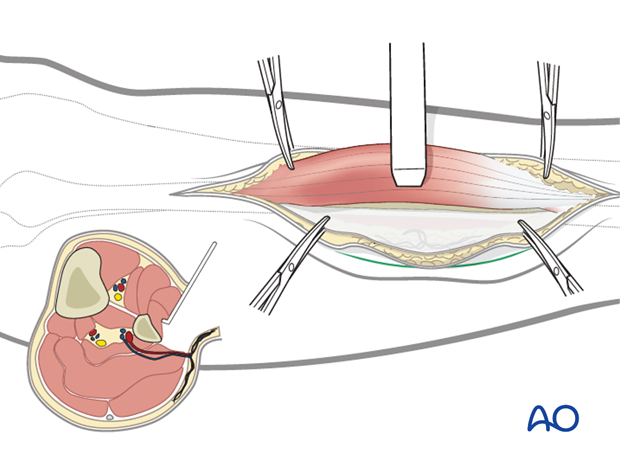
Sharp dissection is then carried to the interosseous membrane leaving a thin layer of the extensor hallucis longus and the extensor digitorum longus attached to the fibula.
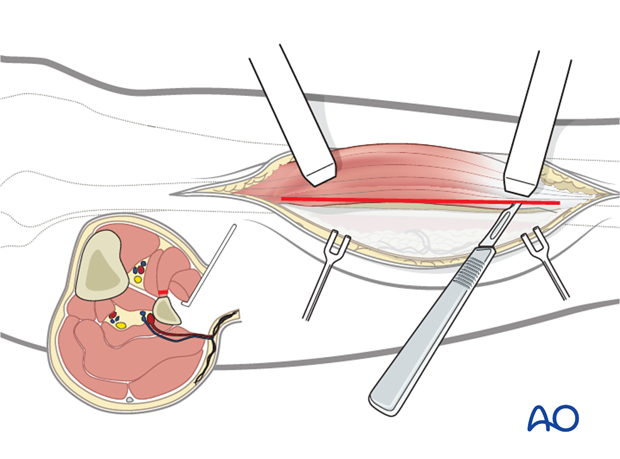
Osteotomies
Subperiosteal dissection is performed 360° around the fibula at the osteotomy sites.
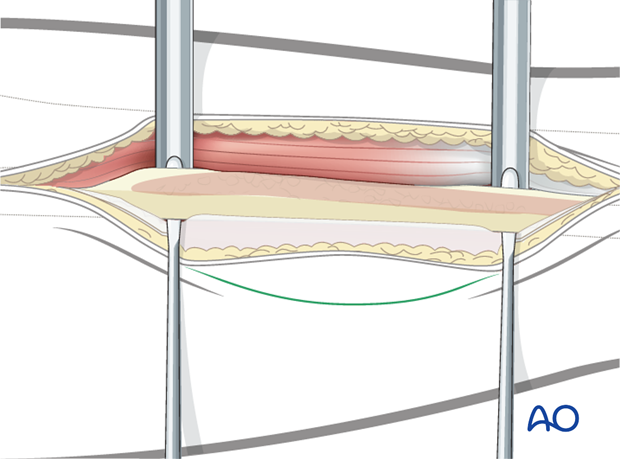
While protecting the peroneal vessel with a periosteal elevator, an osteotomy is then carried out from posterior to anterior using a giggly saw or a sagittal saw.
Alternatively the osteotomy may be performed form anterior to posterior. In this case care has to be taken not to compromise the vascular pedicle.
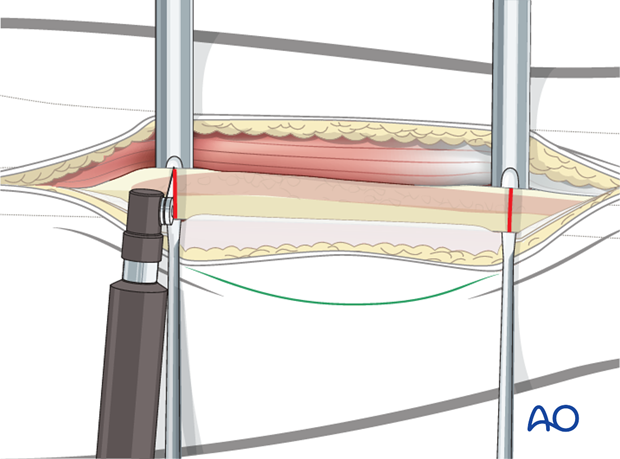
The interosseous membrane is cut
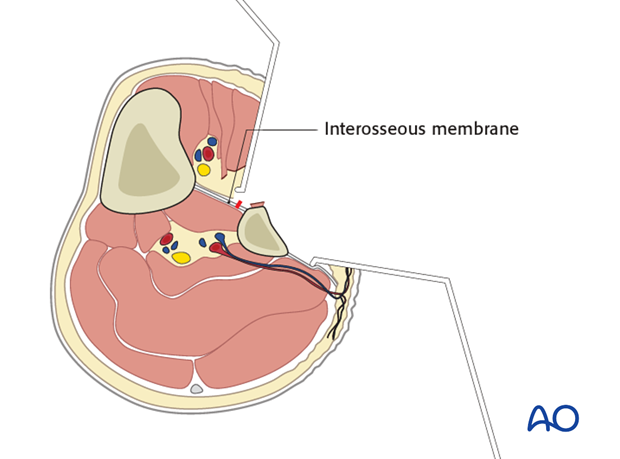
Dissection of the posterior compartment
The posterior tibialis is divided to expose the pedicle.
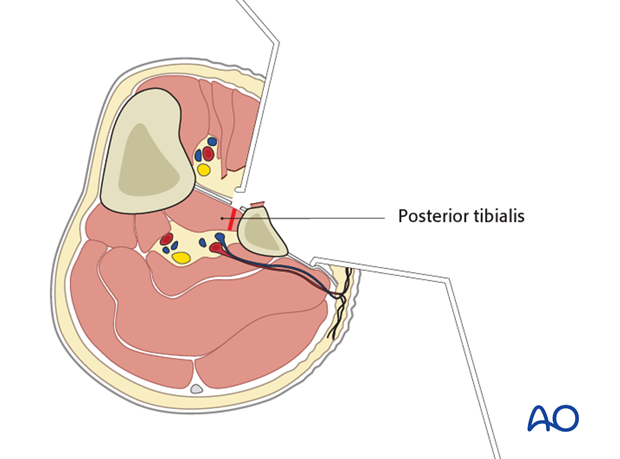
The osteotomized bone segment is retracted laterally to expose the peroneal vessels.
The distal branches of the pedicle is now identified and ligated.
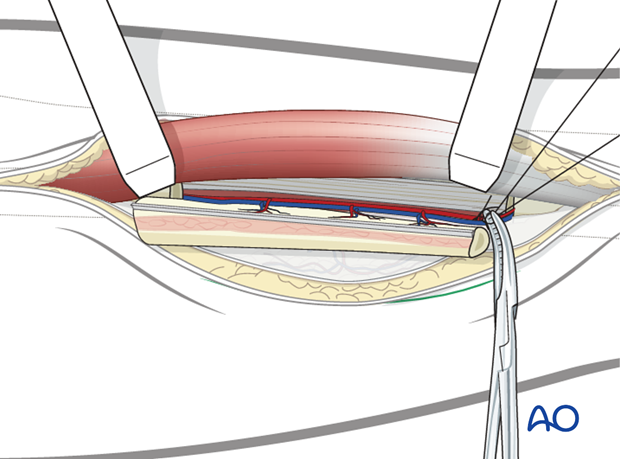
When harvesting an osteocutaneous flap, the posterolateral skin incision is now made down to the fascia and a subfascial elevation of the skin from the soleus muscle is made. Care has to be taken to protect the perforators from the peroneal artery during this step.
If the skin flap is not needed, the skin perforators can be sacrificed.
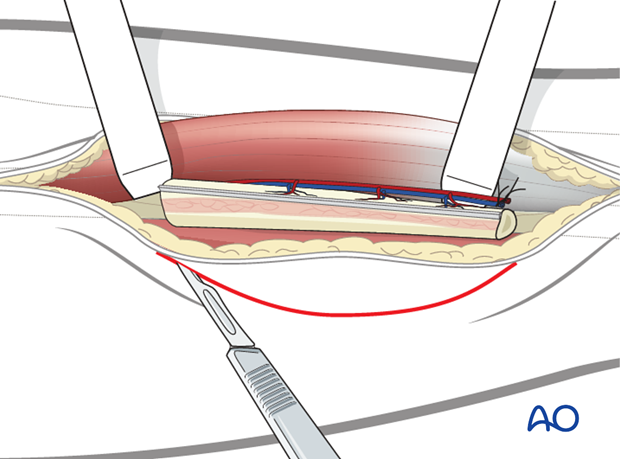
While retracting the bone segment, the flexor hallucis is transected from inferior to superior leaving a thin muscle cuff in order to protect the vascular pedicle.
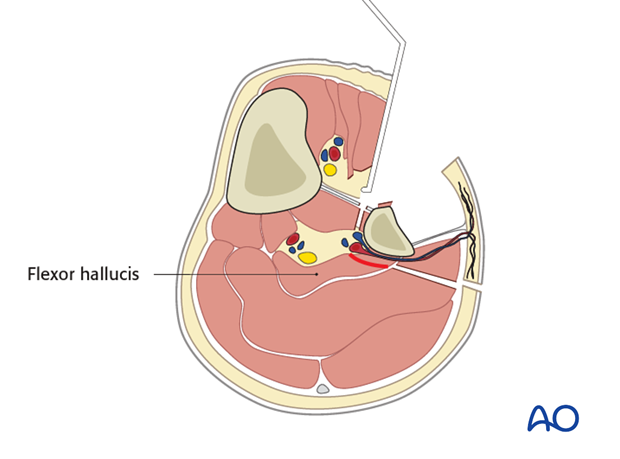
Pedicle dissection
The proximal pedicle could be dissected up to the bifurcation area of the posterior tibialis and the peroneal vessels.
If any major branches are found, it has to be verified whether it is the main blood supply to the lower limb. If it is not the main blood supply, it is ligated.
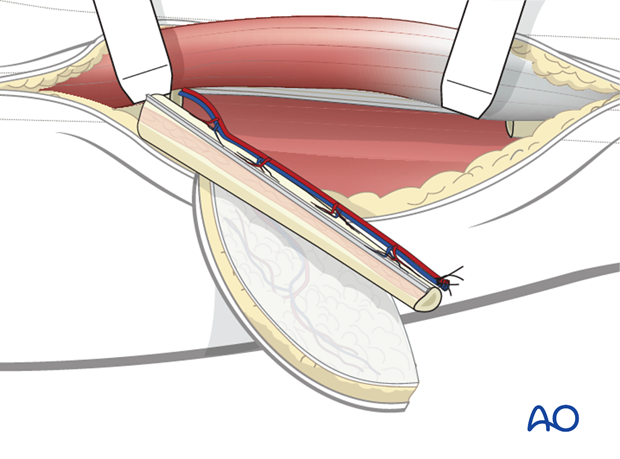
Verification of main blood supply
To verify that the blood supply to the foot is intact, the tourniquet is deflated and the proximal peroneal artery temporarily occluded with an artery clamp. The arterial oxygen saturation is then measured to verify adequate blood supply to the foot. Alternatively a pulse of the dorsal foot (dorsalis pedis) is found by palpation.
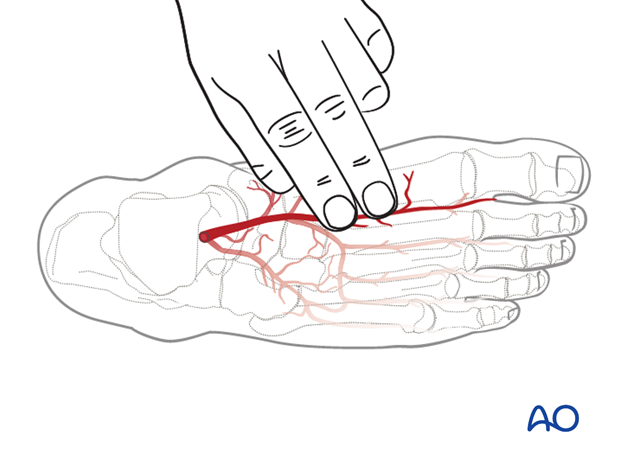
When the reconstruction site is ready, the pedicle can be transected. Pedicle length will be determined as required.
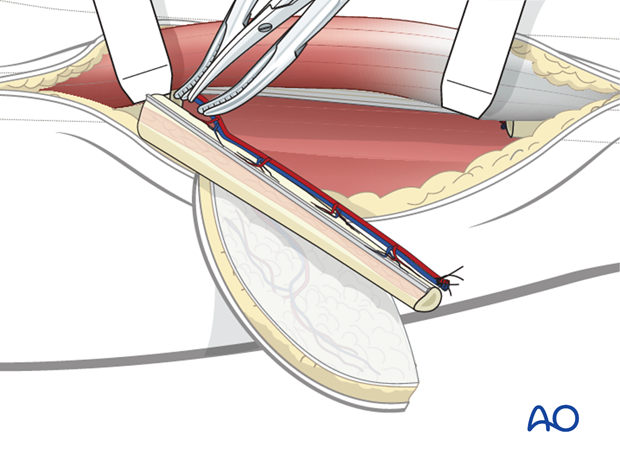
Closure
A drain is inserted and a subcutaneous undermining is performed to allow for wound closure.

If the skin paddle is narrow, primary closure of the skin can be accomplished as long as it is tension free.














