Two jaw surgery
1. Introduction
Bimaxillary surgery is the combination of mandibular and maxillary osteotomies.
In one jaw surgery the occlusal plane of the mandible or the maxilla dictates the final position as only one jaw is going to be mobilized, whereas in bimaxillary surgery the occlusal plane can be altered and the jaws can be repositioned in three dimensions. Bimaxillary surgery requires an intermediate occlusal splint to help position the first jaw.
Bimaxillary surgery is usually required for facial asymmetries, combined anterior-posterior problems involving both jaws, vertical deformities and or transverse discrepancies, eg, apertognathia, open bite (dento-alveolar, skeletal base, combination of both) and crossbites.
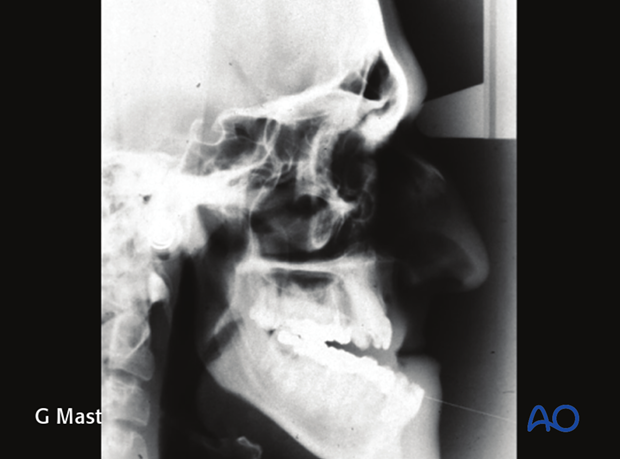
This X-ray show an extreme facial deformity with sagittal and vertical disorders associated with a wide skeletal anterior open bite.
This case is used to exemplify the principles of bimaxillary surgery.
2. Planning
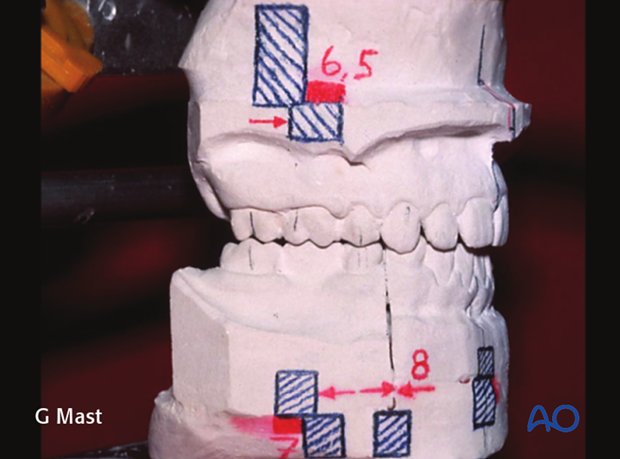
Surgical planning is performed on a semi adjustable articulator. The surgical plan is to advance the maxilla, to set back the mandible, and to perform a body ostectomy of the mandible to reduce the mandibular excess and close the open bite.

Completed model surgery showing the necessary movements and the desired postoperative occlusion.
3. First step maxillary correction
The maxilla is usually repositioned first using Le Fort I osteotomy and an intermediate splint. Internal fixation is then applied.
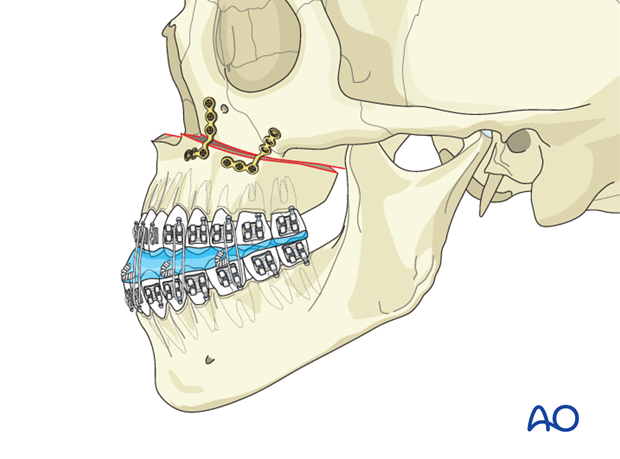
After stable fixation of the maxilla, the MMF and the intermediate splint are removed. A 5-piece mandibular osteotomy is performed with bilateral stepwise body osteotomies and bilateral sagittal split osteotomies (Obwegeser).
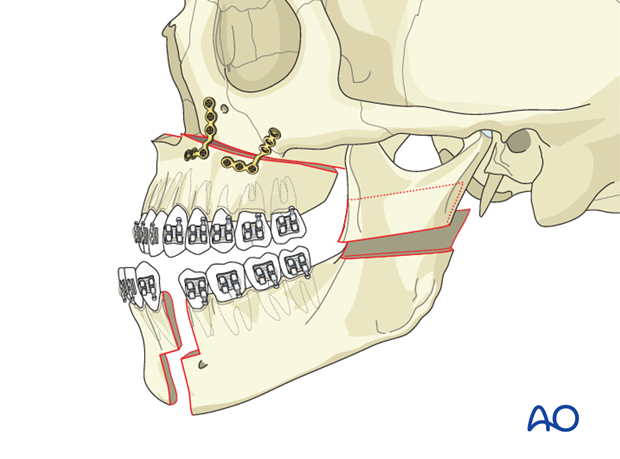
4. Second step mandibular correction
Internal fixation of the mandible is performed with the patient in MMF with the occlusion secured through the final splint.
Stable internal fixation allows for 3-dimensional fragment control and for a limited immediate postoperative function (soft diet).
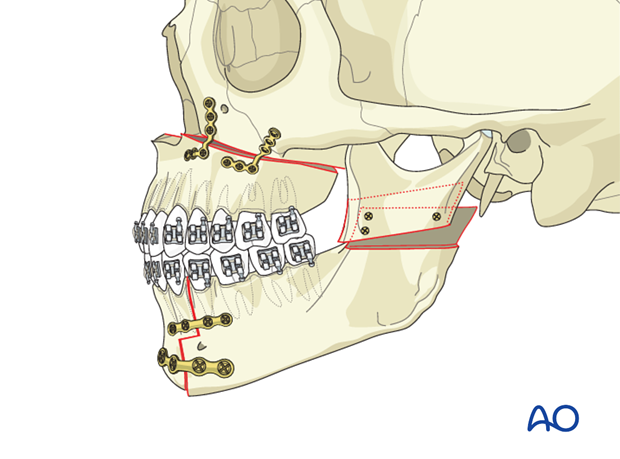
5. Case
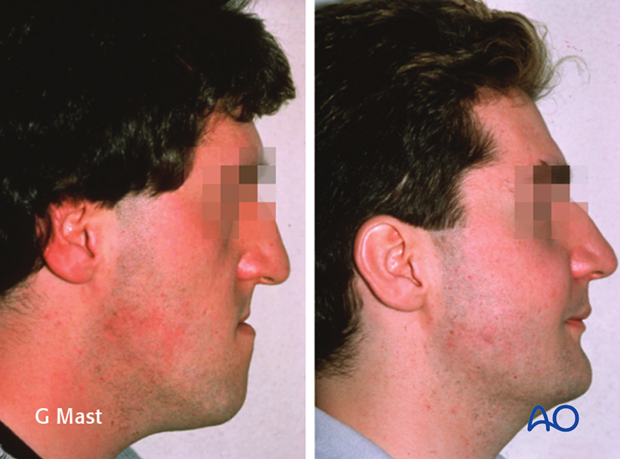
Change of facial dimensions from the frontal and…
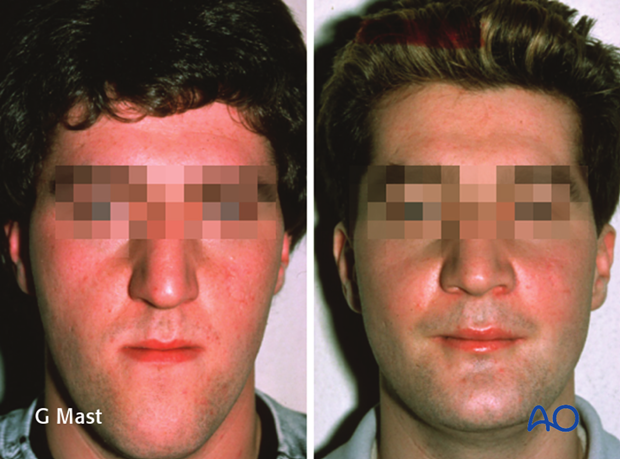
…lateral views.