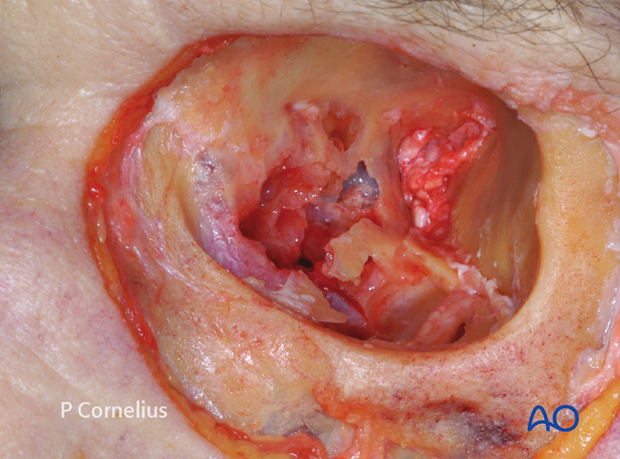
Periorbital dissection of medial wall
1. Introduction
Medial orbital wall fractures are less common than orbital floor fractures. They rarely occur as an isolated entity, but are found in association with orbital floor fractures or as a component of nasoorbitoethmoidal fractures.
According to the type of injury exposure of the medial orbital wall can be accomplished either via a limited small incision or an extended surgical approach (ie, the pre-/transcaruncular approach may be used instead of a coronal approach).
Both approaches have their specific advantages and pitfalls. The pre-/transcaruncular approach allows adequate access to the medial orbital wall and can be extended using a transconjunctival incision to expose the orbital floor. The attachments of the medial canthal apparatus and the lacrimal sac restrict the placement of retractors for the exposure of the anterior and superior portion of the medial wall.
If indicated a lateral canthotomy and inferolateral cantholysis can also be used to extend the approach to the lateral orbital wall.
This combination of the pre-/transcaruncular, the transconjunctival, and the lateral canthotomy provides access to three orbital walls in the medio inferolateral circumference of the orbital cavity through a single incision.
The coronal flap approach is much more invasive, since it is performed bilaterally and developed from a remote scalp incision. It is indicated to gain exposure of the medial orbital wall from above as well as the mediosuperolateral orbital rims, the bony glabella, radix of the nose, to the roof and the lateral orbital wall.
In combination with a lower eyelid approach it allows access to the entire orbital circumference.
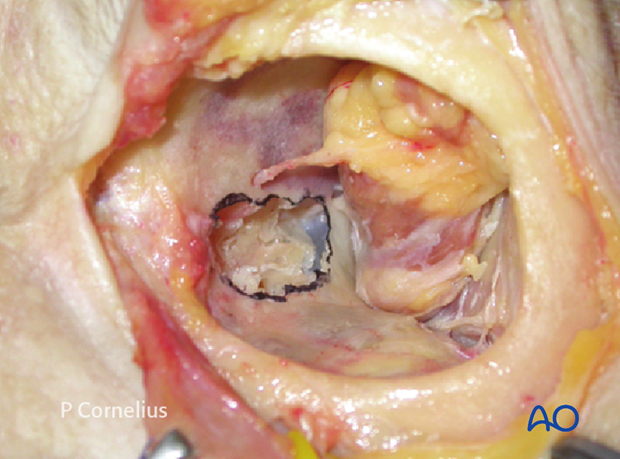
While the periorbital dissection of the medial wall via a coronal approach will interfere with the trochlea, the laterally extended pre-/transcaruncular incision has to get around the inferior oblique muscle (see anatomical specimen).
Irrespective of the approach care must be taken to avoid injury to the palpebral, medial canthal anatomical structures, and the lacrimal apparatus. Therefore the posterior lacrimal crest is the landmark for the anterior limit of the medial wall dissection.
In the process of dissecting along the medial wall damage to the very thin lamina papyracea must be avoided.
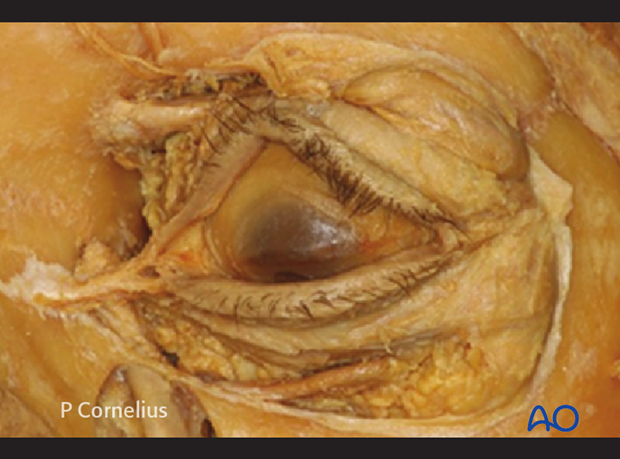
2. Inferior Route
Using a pre-/transcaruncular incision, the periorbita is incised posterior to the insertion of Horner’s muscle along the posterior lacrimal crest from within the periorbital sac (extraconal orbital space). The incision is made in a vertical direction either with a scalpel or with spreading motions of a sharp pointed scissors. The dissection is continued posteriorly underneath the periorbita using a periosteal elevator. The path of dissection along the medial orbital wall starts inferiorly and turns superiorly to create a subperiosteal cavity for the insertion of a malleable ribbon retractor. The anterior ethmoidal neurovascular bundle is the first transverse structure encountered at the upper limit of the operative field. The anterior ethmoidal neurovascular bundle marks the ethmoid roof and the ethmoid-frontal suture line. The periorbital dissection is continued posteriorly along this suture line until the posterior ethmoidal neuro-vascular bundle is exposed.
The posterior neuro-vascular bundle is a critical landmark indicating the posterior limit of the medial wall dissection. The ethmoid-sphenoidal suture line and the sphenoid body are not exposed under clinical conditions, since they lie at the base of the orbital apex.
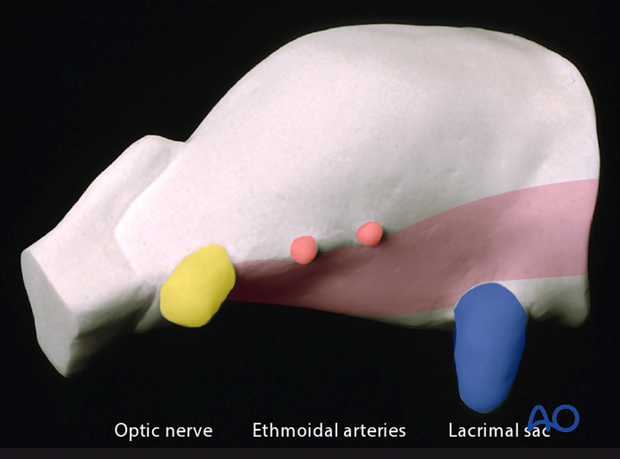
In the anatomical specimen these bony structures are dissected free to demonstrate the dense topographic relationship to the optic nerve exit.
Note: Vigorous retraction with a ribbon retractor may affect the globe and/or the optic nerve function. Intermittent relaxation of the retractor permits vascular reperfusion and may prevent complications. It is strongly recommended that the operating surgeon holds the retractor during the periorbital dissection of medial wall.
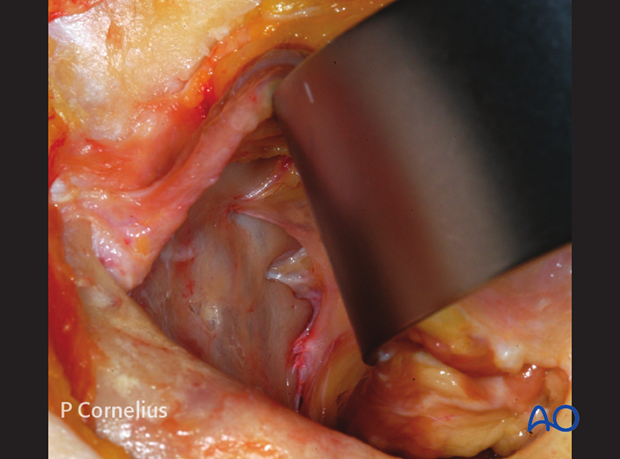
3. Superior Route
Via the coronal approach the superomedial and medial periorbita can is stripped including the trochlear region following the release of the supraorbital nerve and the reflection of the periosteum over the supraorbital margin.
To simplify the workflow the periorbital dissection of the roof and the medial orbital wall are then combined. The anterior ethmoid neurovascular bundle can be identified by the area where the periorbita tents outward from the foramen as shown.
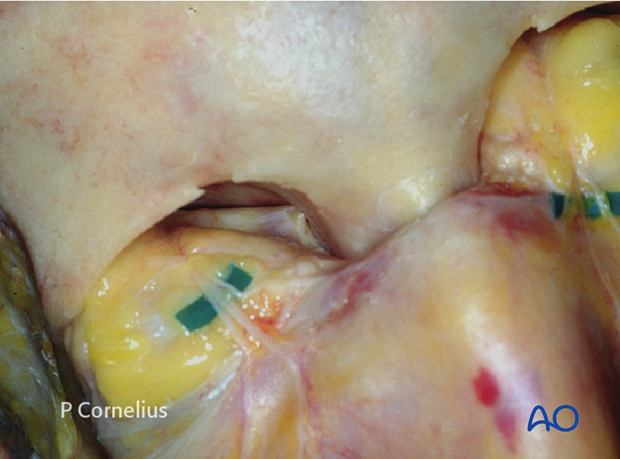
The periorbital dissection proceeds towards the apex of the orbit following the ethmoid-frontal suture line. This provides broad access to the posterior ethmoidal (neuro)-vascular bundle. The periorbital strands from the posterior ethmoid foramen may connect laterally to the recurrent meningeal artery foramen inside the greater wing of the sphenoid as demonstrated in this specimen.
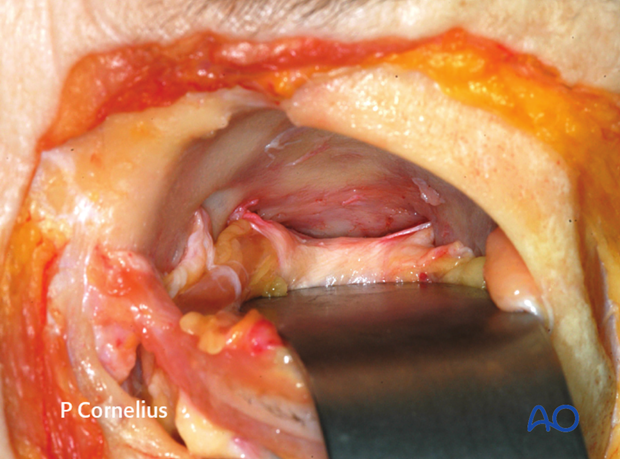
4. Ligature of Ethmoidal Neurovascular Bundles
The anterior ethmoid and posterior ethmoidal vessels can be cauterized using bipolar cautery or clipped and sectioned in order to extend the surgical exposure. Use of electrocautery in the vicinity of the optic nerve must be avoided. The posterior ethmoidal artery is usually clipped to avoid thermal injury to the optic nerve.
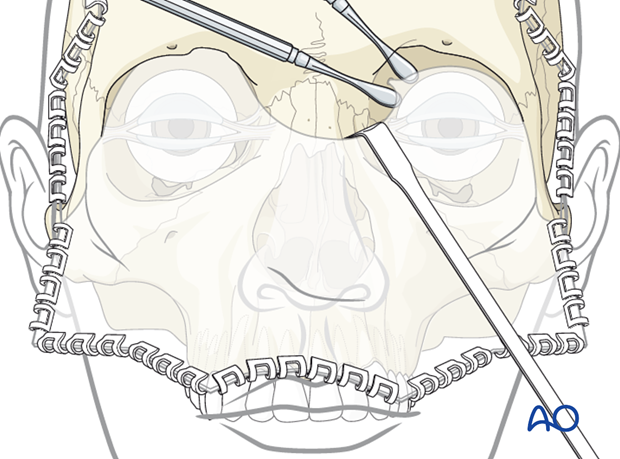
The anterior ethmoidal vessels are retracted out of the foramen allowing for cauterization or titanium clip ligation.
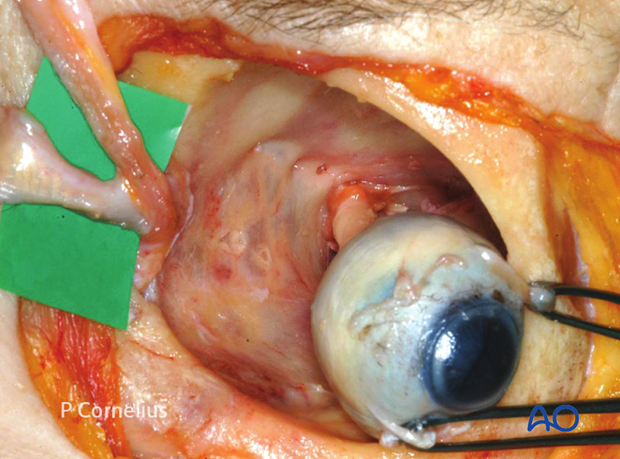
5. Ethmoidal Foramina/Optic Nerve
This anatomic anterolateral view of the medial orbital wall demonstrates the relationship between the ethmoidal foramina and the entrance of the optic nerve. The orbital contents apart from the globe and the optic nerve have been removed.
The tarsi are reflected medially to expose Horner’s muscle inserting along the posterior lacrimal crest.
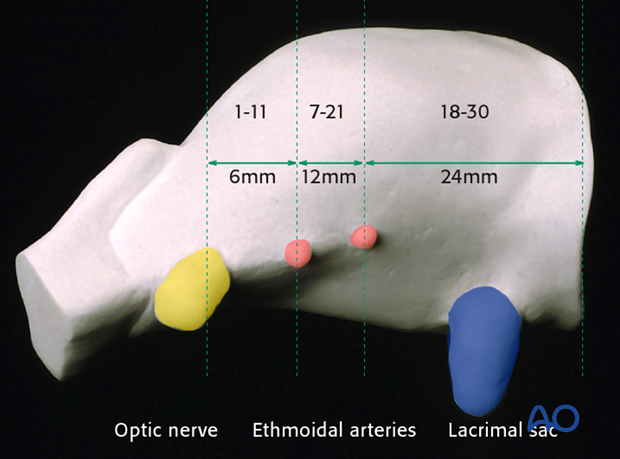
Once again the corresponding diagrammatic representation of the average distances between the orbital rim, the ethmoidal foramina and the optic nerve for convenient orientation.
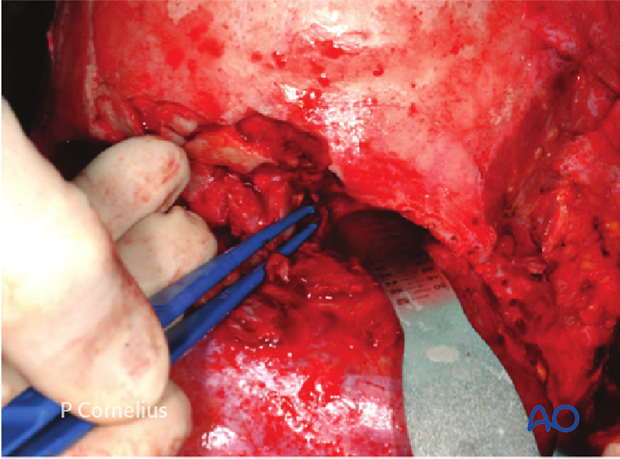
6. Internal Orbital Buttress
The inferior border of the medial orbital wall is defined by the ethmoid-maxillary suture line. The bony condensation along this line is made up essentially by the maxilla and represents an internal orbital buttress, which often remains intact in orbital trauma.
The internal orbital buttress (see the bone strut midway between the defects in the orbital floor and medial wall in the anatomic example) is further supported by the basal lamellae framework (ie, basal lamellae of the ethmoid bulla and the middle turbinate) and its honeycomb extensions inside the ethmoid.
The inferior limit of the periorbital dissection along the medial wall goes beyond this boundary and continues onto the posterior medial bulge.