Periorbital Dissection of Lateral Orbital Wall
1. Introduction
A complete exposure of the lateral wall in its boundaries from the lateral aspect of the inferior and superior orbital fissure over the greater wing of the sphenoid, the recurrent meningeal foramen and the zygomaticofrontal suture to the lateral orbital rim can easily be achieved from a superolateral access via a coronal approach.
An inferior approach via an extended lateral canthotomy or infraciliary approach will put restraints to reach the posterior borderline at the superior orbital fissure and the transition to the roof.
Either of these approaches is usually combined with the detachment of the lateral canthus (lateral cantholysis).
Moreover during the inferior approach, transsection of the soft-tissue contents of the inferior orbital fissure increases exposure of the lateral orbital wall.
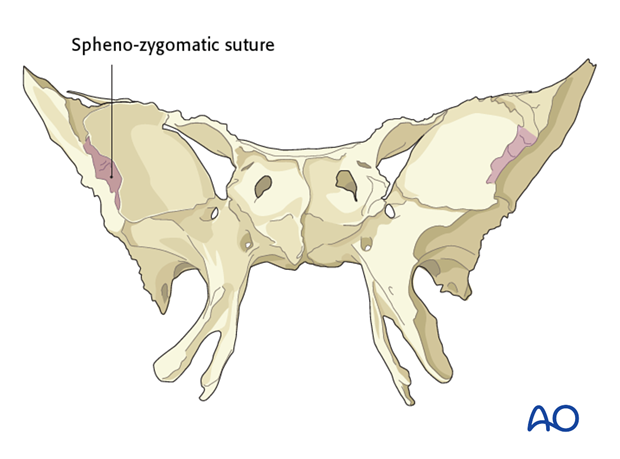
The lateral orbital wall encompasses the zygomatico-sphenoid suture line. This is regarded as the keystone for the reduction of complex zygoma fractures and aids in reestablishing the outer facial frame in complex midface fractures
With the exception of a minor post rim concavity and Whitnall‘s tubercle the lateral orbital wall is uniplanar. The zygomatico-sphenoid suture line is located in the thinnest portion between the orbital surface of the greater wing of the sphenoid and the orbital surface of the zygomatic bone.
Using the coronal approach the periorbita is raised with a periosteal elevator in the inferolateral direction after the periosteum at the orbital rims has been vertically incised and reflected.
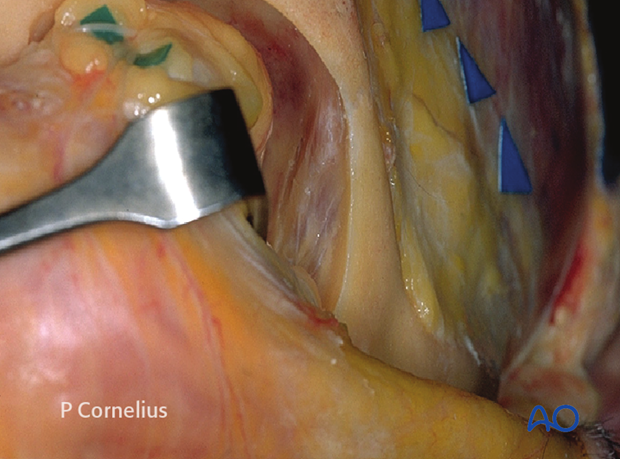
2. Inferolateral Aspect
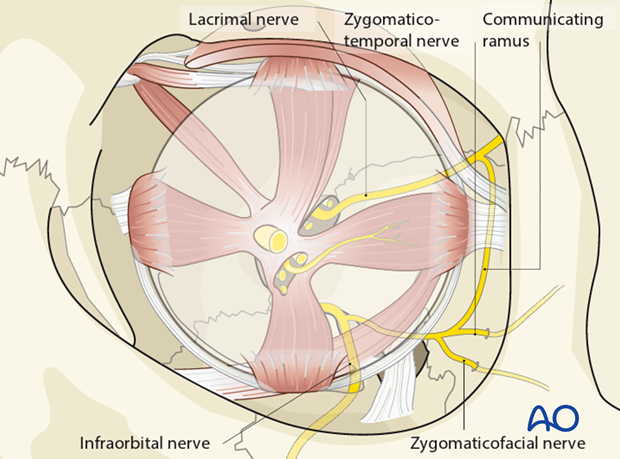
During the periorbital dissection of the inferior portion of the lateral orbital wall two branches of the sensory zygomatic nerve (branch of V2); the zygomaticotemporal and zygomaticofacial nerve are identified. They pierce the periorbital sac, traverse the opened subperiosteal space and exit the orbit laterally.
The zygomaticotemporal nerve can ascend in a groove on the lateral orbital wall and will enter a canal in the orbital surface of the zygoma, leading to the temporal fossa.
The zygomaticofacial nerve also runs through a canal in the zygoma and exits laterally over the prominence of the zygomatic body.
The periorbital dissection of the lateral orbital wall either from a superior or inferior access usually requires division of these two sensory branches of the zygomatic nerve, causing loss of sensation to the skin over their distribution in the area of the lateral orbital margin and the prominence of the zygomatic body.
The zygomaticofacial nerve is sometimes replaced by an infraorbital nerve branch.
3. Exposure of the Zygomaticosphenoid Suture
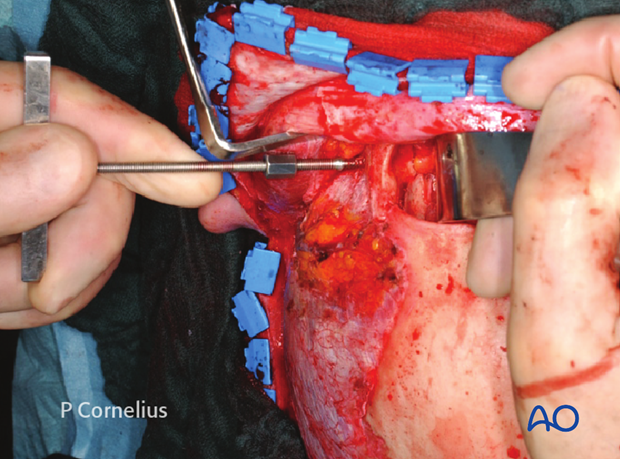
Clinical example of a subperiosteal exposure of the zygomaticosphenoid suture-line via a coronal approach in a Le Fort III type midfacial fracture pattern.
The zygoma is realigned by means of a Carroll-Girard Screw inserted into the zygomatic body under direct control of its articulation to the skull base at the zygomaticosphenoid suture.
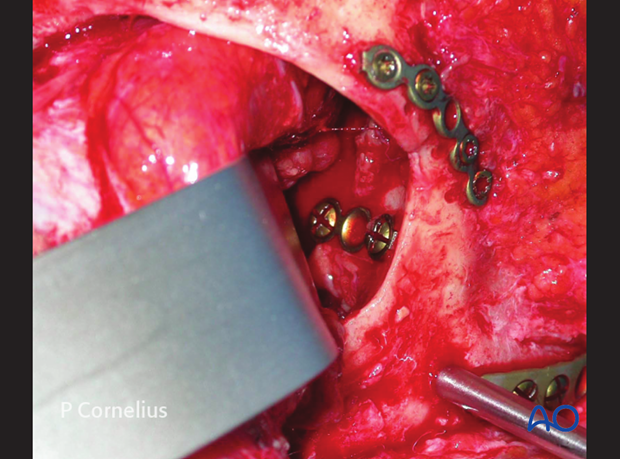
The periorbital dissection of the lateral orbital wall via a coronal approach allows for a plate osteosynthesis inside the orbit.
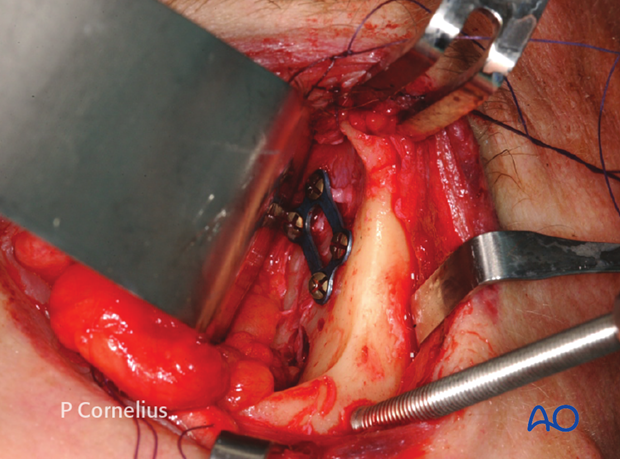
An extended exposure of the lateral orbital wall via a lower eyelid swing approach and complete detachment of the lateral canthus also provides adequate access to the zygomaticosphenoid suture line for the placement of an osteosynthesis across this bony junction.
Note: A lateral canthopexy must be performed at the conclusion of the procedure to reattach the lateral canthal ligament.
4. Deep Dissection
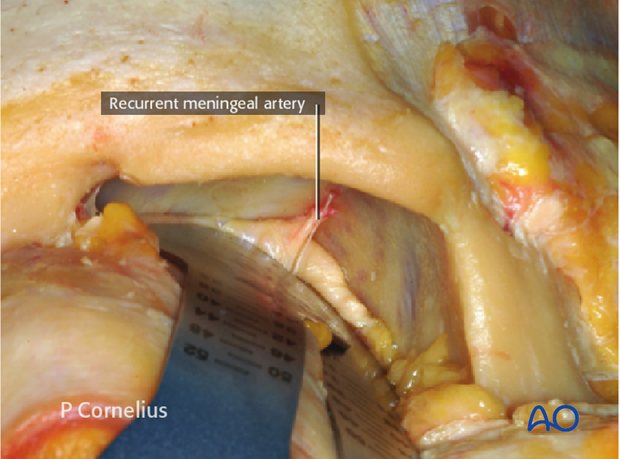
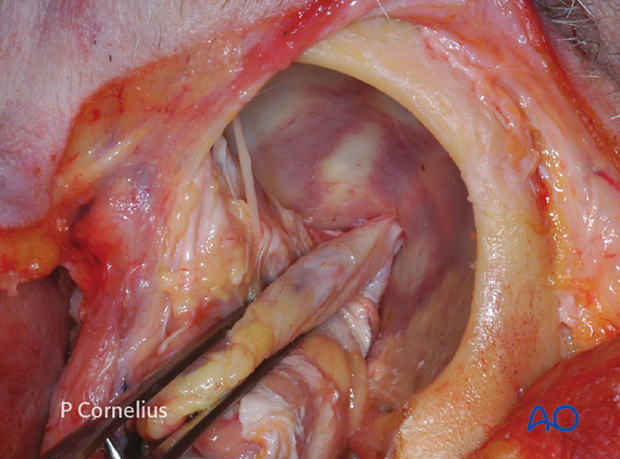
When necessary the periorbital dissection proceeds posteriorly to the temporal side of the orbital apex, until the periorbital/dural soft-tissue reflection at the lateral aspect of the superior orbital fissure is identified, as demonstrated in the anatomical specimen.
The recurrent meningeal artery passing through the periorbita to its respective foramen along the sphenofrontal suture line is encountered during the deep dissection.
Inferiorly the lateral border of the inferior orbital fissure will come into view.
5. Contents of the Superior Orbital Fissure
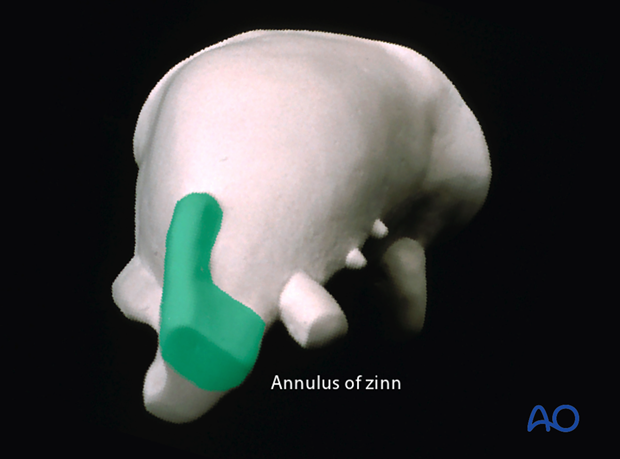
Reminder: the superior orbital fissure is divided by the anulus of Zinn (insertional bands of the lateral rectus muscle) into two compartments.
The lateral or extraconal compartment transmits the following structures:
- Nerves
- Motor: trochlear (CN IV)
- Sensory (CN V1): frontal, lacrimal
- Vessels
- Superior ophthalmic veins
The medial or intraconal compartment transmits the following structures:
- Nerves
- Motor: oculomotor (CNIII) upper and lower division, abducent (CN VI)
- Sensory (CN V1): nasociliary
- Sympathetic fibres
- Vessels
- Superior ophthalmic veins
In a strict periorbital dissection everything outside the superior orbital fissure and the Anulus of Zinn is safe against iatrogenic damage.