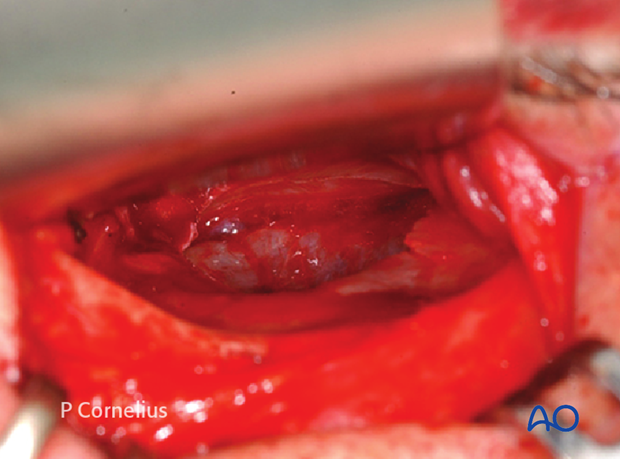
Periorbital Dissection of Inferior orbital wall/Orbital floor
1. Introduction
The most common fracture site inside the orbit is the inferior wall. Various fracture patters can occur and require an exposure of the bony ledges around the boundaries of a fracture or bony defect.
2. Anterior dissection
The periosteum at the infraorbital orbital margin is incised.
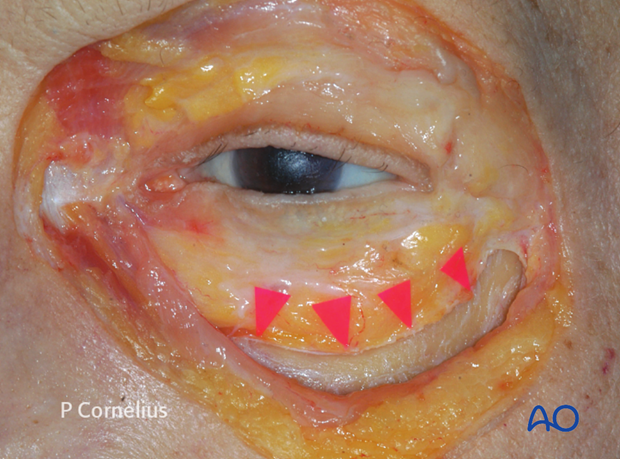
Sharp periosteal elevators are used to reflect the periorbita the full length of the incision over the top of the bony rim. This is begun inferolaterally below the arcus marginalis detaching the thick septal attachments in this region. The periorbita is then elevated to start the exposure of the orbital floor as demonstrated in the anatomical specimen.
Note: at this stage the inferior conjunctival/lower lid retractor flap is sewn temporarily to the upper eyelid margin to protect the cornea against abrasion in transconjunctival approaches.
Note: It is essential to use sharp periosteal elevators to prevent tearing of the periorbita. A sharp elevator maintains a surgical plane more easily than a dull one and strips off the periosteum cleanly.
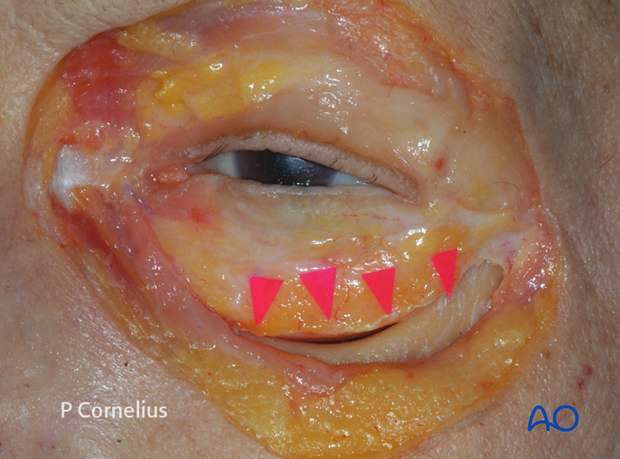
The periorbita is then elevated from the underlying bone with a sweeping motion of the periosteal elevator in a lateromedial direction. A second periosteal elevator is helpful for the retraction of tissue at this stage.
As the dissection continues posterolaterally the periorbital prolongations running into the anterior loop of the inferior orbital fissure are visualized.
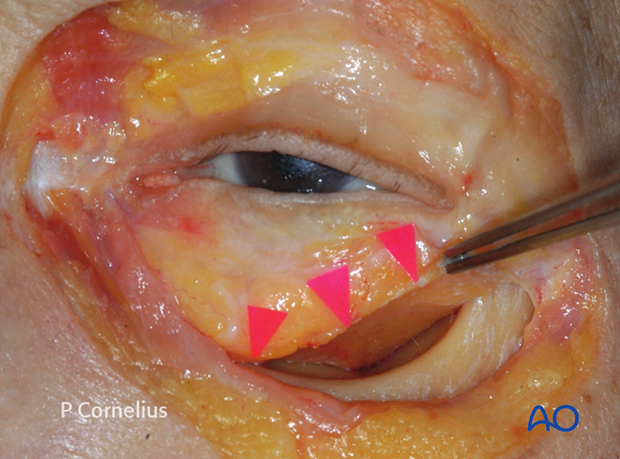
The periorbital dissection along the orbital floor proceeds posteriorly in a two-handed technique using a malleable ribbon retractor with a wide rounded tip and a periosteal elevator.
The ribbon retractor is bent in an S-shape, so that the non-dominant hand holding it can comfortably rest on the forehead of the patient while the dissection is carried on with instruments in the dominant hand.
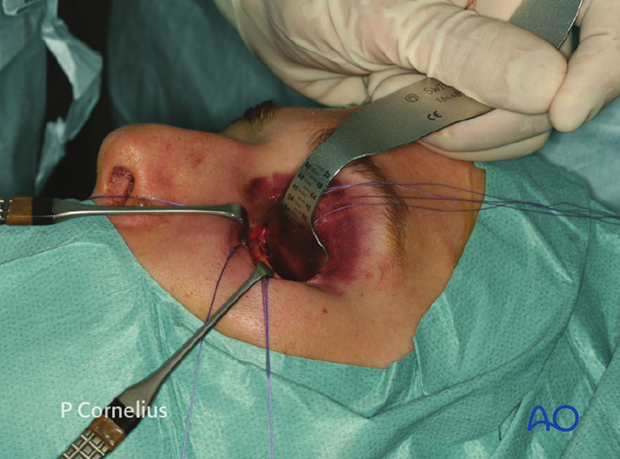
In order to ensure a clean periosteal dissection, the bony contours must be respected taking into account the concavity in the anterior region of the floor behind the orbital rim (‘postentry widening’). Here the periosteal dissection is initiated with the periosteal elevator introduced in an almost vertical direction to avoid entry into the periorbita.
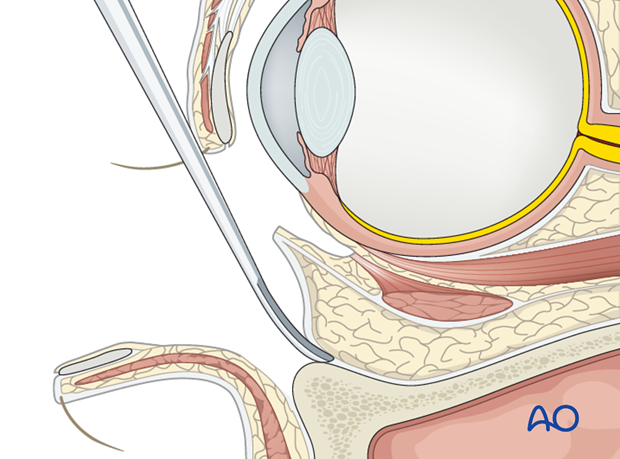
If the dissection is strictly kept in a subperiosteal plane, the origin of the inferior oblique muscle will not be directly visualized.
The muscle arises from a tiny bony depression lateral to the nasolacrimal canal and courses posterolaterally inferior to the rectus muscle. It then spreads out and inserts on the posterior temporal sphere of the globe.
When using a retroseptal approach the muscle may be cut above its origin and reapproximated at the end of the procedure.
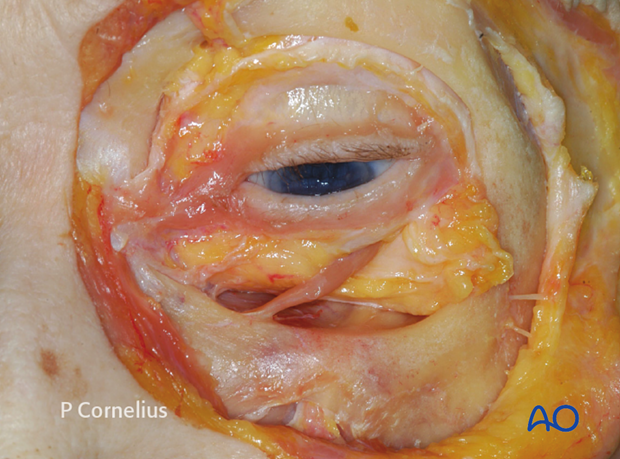
3. Infraorbital Neurovascular Bundle
Behind the transition between the anterior mid orbit the orbital floor slopes upwards giving rise to the posterior medial bulge and to a slightly convex bony platform in the posterior lateral portion adjacent to the inferior orbital fissure. The elevator is passed transversely sweeping medially and advancing along the inferior orbital fissure. The tip of the retractor is then placed more posteriorly.
During this maneuver the infraorbital neurovascular bundle can usually be visualized first shining through the thin bony roof of its canal. Then it becomes directly visible in the infraorbital groove. Fractures frequently expose varying portions of the infraorbital nerve in its sagittal course on the way from the infraorbital rim to the middle of the maxillary edge of the infraorbital fissure.
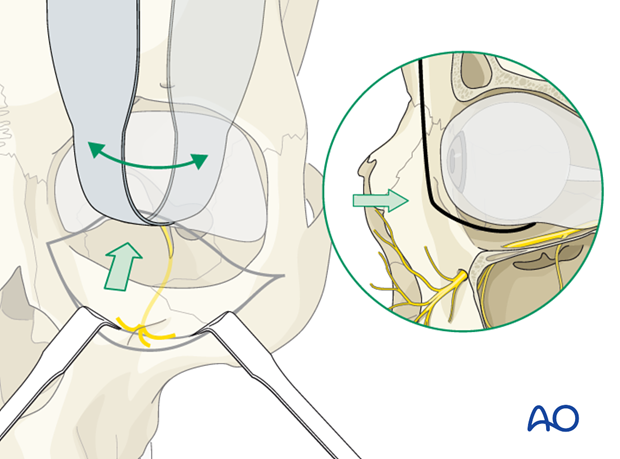
Depending on the amount and severity of comminution around the course of the infraorbital nerve, a bony decompression might be indicated. Early intervention is favorable for a return of normal sensory function.
Fragmentation at the posterior end of the orbital fissure downwards into the pterygopalatine fossa is demonstrated in the anatomical specimen. In this case nerve exploration via a transorbital route is very difficult and might require an inferior marginotomy or a transantral approach for decompression.
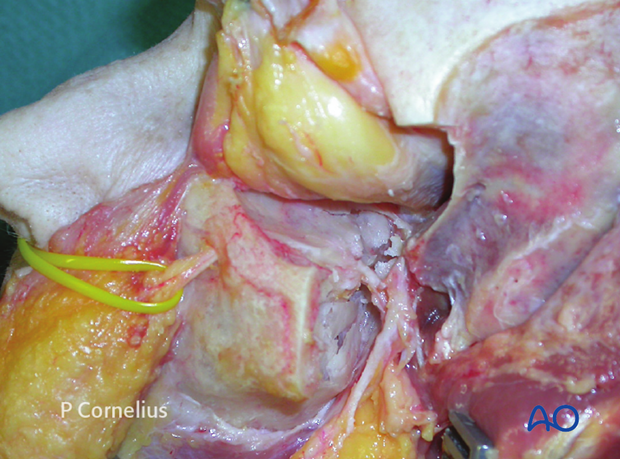
4. Extent of Periorbital Dissection
Taking into account the extent of a fracture or defect, the periorbital dissection stops at the medial border of the inferior orbital fissure leaving the soft tissue invagination intact.
Laterally, the dissection is continued to the posterior edge of the floor to the orbital process of the palatine bone. The suture between the maxilla and the palatine bone is indistinguishable in the adult skull.
Medially the periorbital dissection (as shown in the anatomic specimen) extends to the zone over the internal orbital buttress where the orbital floor blends into the medial wall.
Note: Small vessel branches of the infraorbital artery must be divided by bipolar cauterization to achieve a clear plane of dissection when the periorbita is raised from the orbital floor. A constant communicating arterial branch is present between the infraorbital groove and the periorbita above the post entry zone and must be cauterized.
Diffuse bleeding is controlled by temporary packing with neurosurgical cottonoids or gelatin sponges soaked with a solution containing a diluted vasoconstrictor.
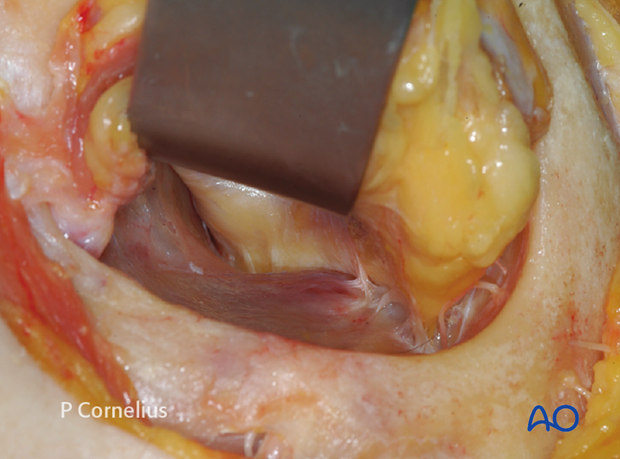
5. Inferior Orbital Fissure Soft-Tissue Contents
In many cases a periorbital dissection of the floor with a tunnel medial to the inferior orbital fissure will be sufficient.
For an extended access to the posterior orbital floor, the contents of the inferior orbital fissure must be addressed and transected to allow for this additional access.
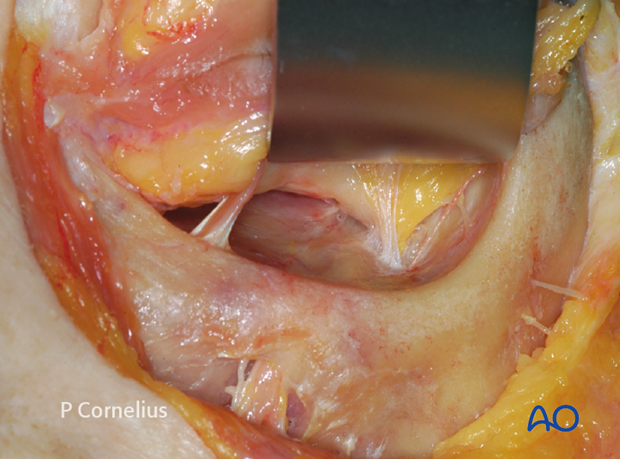
The transsection is prepared with a dissection along the inferior portion of the lateral orbital wall in order to create a second tunnel alongside the vertical soft-tissue partition.
The intervening soft tissue invagination is transected in a stepwise fashion using bipolar electrocautery and sharp dissection across the fissure above the level of Müller’s vestigial muscle, stripping the periorbita along the lateral edge of the inferior orbital fissure.
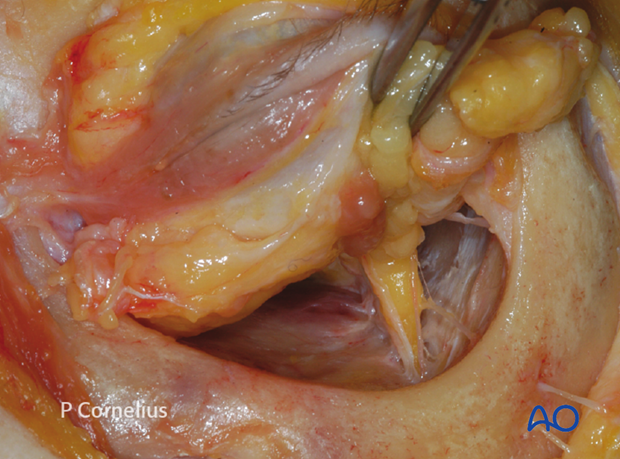
Note: The scalpel blade is turned perpendicular to the lateral orbital wall, to prevent it from intruding into the infratemporal/pterygopalatine fossa.
The surgeon must also be aware of the fact that transsection across the periorbital envelope at this level will result in prolapse of periorbital fat into the surgical field.
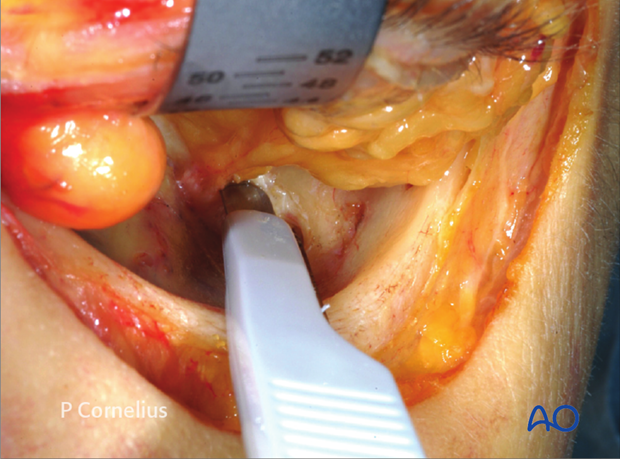
6. Extended Exposure
This illustration demonstrates the stripping of the periorbital layer from the inferior lateral orbital wall immediately adjacent to the inferior orbital fissure with a sharp elevator proceeding posteriorly.
The periorbital layer is thick in this zone, facilitating its elevation in a lateromedial direction to expose the posterior portion of the orbital floor.
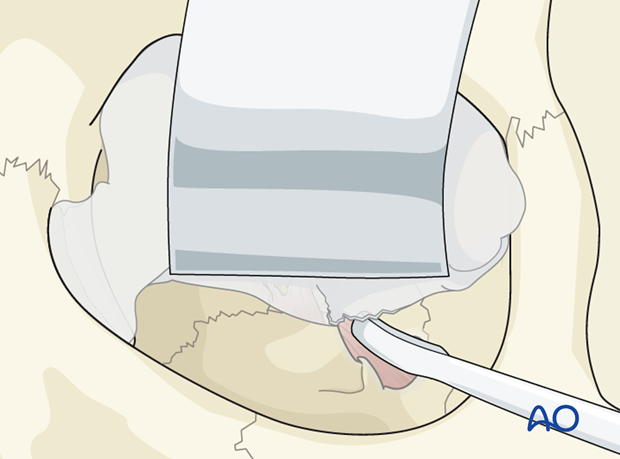
The subperiosteal dissection is continued using a periosteal or freer elevator in a lateromedial direction and lifted up and retracted by and by with the ribbon retractor until the entrance of the apex is reached.
The superior retraction increases the exposure of the lower orbital circumference allowing to visualize the most posterior edge of the orbital floor.
The infraorbital neurovascular bundle inside the infraorbital groove and canal now becomes visible over most of its course.
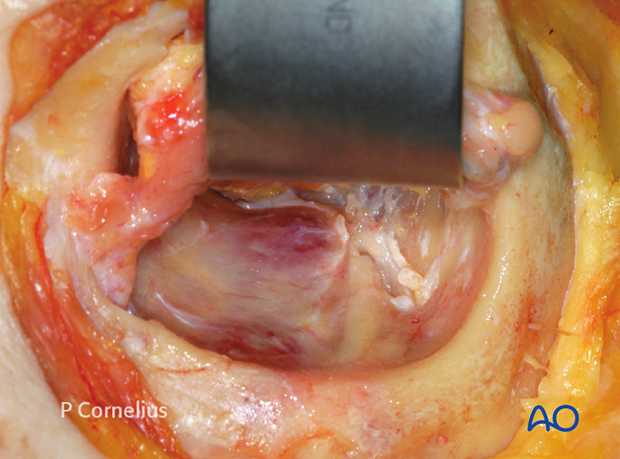
7. Contents of the Inferior Orbital Fissure
The inferior orbital fissure contains the following anatomical structures:
- Nerves
- Sensory (V2) : infraorbital, zygomatico-, (temporal, facial)
- Parasympathetic: (pterygopalatine ganglion)
- Vessels
- Infraorbital artery (maxillary artery)
- Infraorbital vein (pterygoid plexus)
- Müllers vestigial orbital muscle
Transection of the vessels usually does not have serious consequences. However a reduced venous outflow to the pterygopalatine plexus can contribute to orbital vascular congestion.
Note: Soft tissues passing through the inferior orbital fissure should not be confused with orbital soft tissues prolapsing into the maxillary antrum.
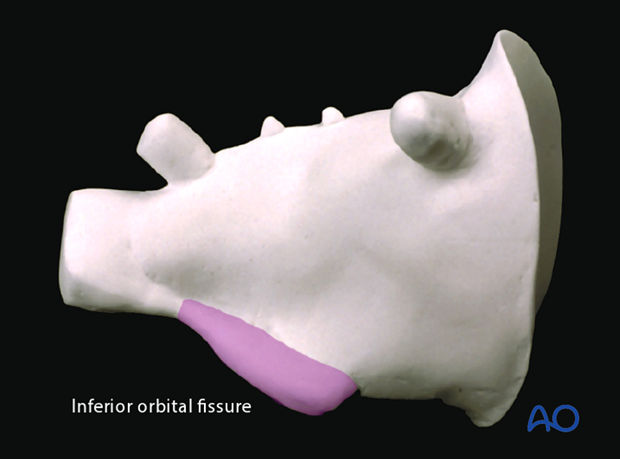
The infraorbital nerve enters the infraorbital groove as it courses from its outlet at the foramen rotundum in the pterygopalatine fossa at a level well below the orbital floor. Therefore the only area where the nerve is at risk for transsection is at it's entry into the infraorbital groove.
The relationship between the infraorbital nerve and the soft-tissue strands going through the infraorbital fissure is demonstrated in this anatomic dissection. The zygoma and the lateral orbital wall have been removed. The lateral recess of the maxillary sinus is opened.
The soft-tissues strands passing the inferior orbital fissure are a continuation of Bichat’s buccal fat pad into the orbit as shown in the anatomic specimen.
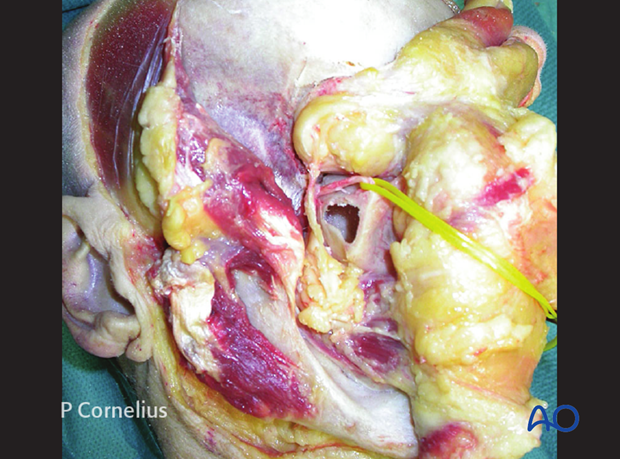
This anatomic dissection shows the orbital floor and the course of the infraorbital nerve after bone removal from an inferior transantral view.
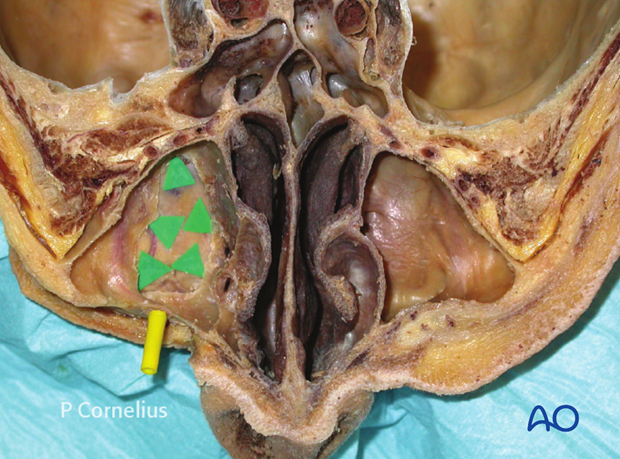
The soft-tissue contents of the inferior orbital fissure are located between the latero dorsal wall of maxillary sinus and the greater wings of the sphenoid. The sectioned vessels within the soft-tissue strand going through the fissure can be seen as labeled.
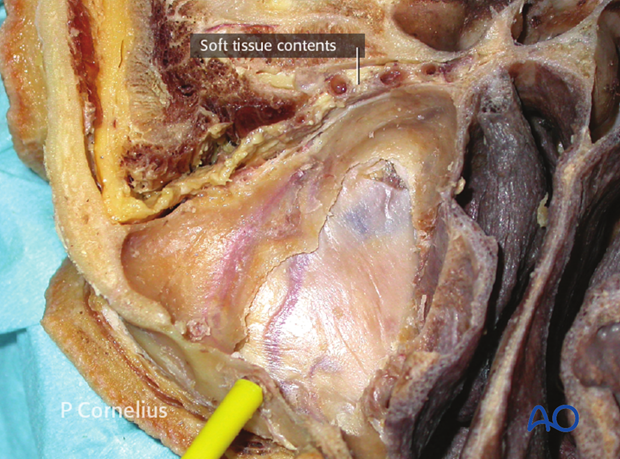
8. Posterior End
In trauma the periorbital dissection along the orbital floor stops at the far end of the posterior lateral promontory.
At this level the coronal cross section of the orbital cavity starts to take a triangular shape. The intraoperative topography can be easily correlated with the CT imaging using this landmark region.
The periorbital dissection of the orbital floor should not proceed to the bony confluence between the superior and inferior orbital fissures. This will intrude into the orbital apex with a high risk of entering the superior orbital fissure resulting in nerve injury inside the muscle cone.
The infraorbital nerve on its course between the outlet at the foramen rotundum underneath the bony confluence and the entry into the infraorbital groove is also protected, if the dissection does not go into the posterior extent of the inferior orbital fissure.
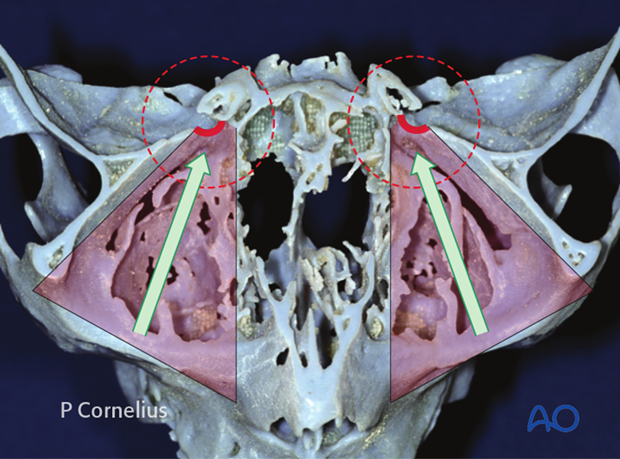
9. Posterior Bony ledge
This anatomical specimen shows the residual posterior bony ledge after an artificial fracture of the orbital floor extending posteriorly.
The posterior lateral promontory is still intact as is the rest of the floor edge to the infraorbital fissure. The defect allows for a view of the most posterior and superior recess of the maxillary sinus underneath the posterior bony strut. The mucosal lining of the sinus has been retracted downwards to allow better visualization.
Note the course of the exposed infraorbital nerve.
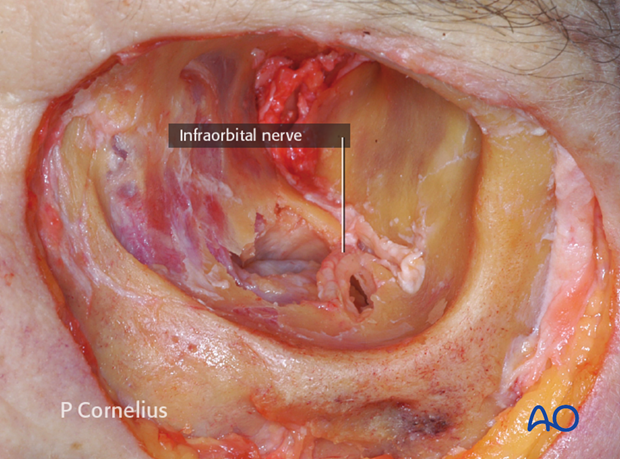
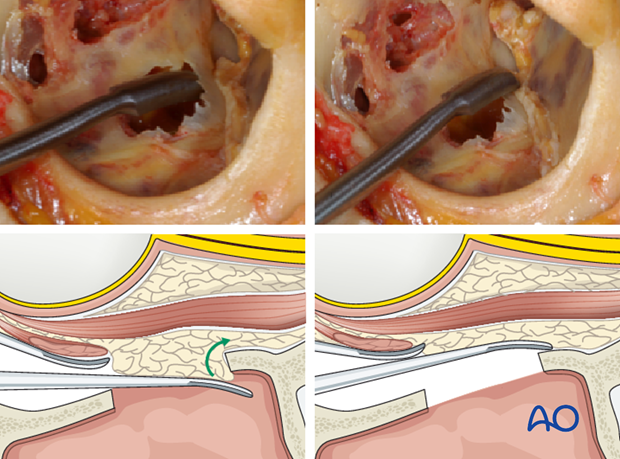
If the view during the posterior dissection of the orbital floor is obstructed by prolapsing fat or soft tissues, it is often helpful to identify the posterior recess of the maxillary sinus using a periosteal elevator and to gauge its depth as a reference.
From the recess of the maxillary sinus, the tip of the elevator can be carried over the fracture line onto the upper surface of the posterior bony ledge to open up a space for the periorbital dissection.
This will allow to lift up the soft tissue with a ribbon retractor exposing the posterior ledge of the orbital floor.
10. Clinical examples
Clinical example of a periorbital dissection (left orbit) along the whole periphery of a lamellar fracture in the medial orbital floor into the midorbit done without transsection of the soft-tissue contents of the inferior orbital fissure.
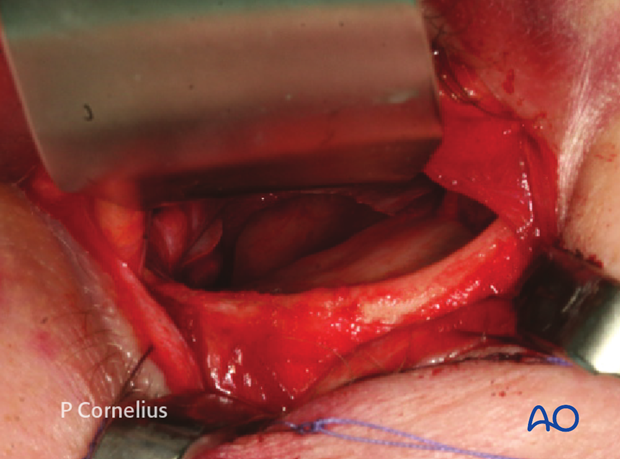
Clinical example of a periorbital dissection (right orbit) along the whole periphery of a lamellar fracture in the orbital floor reaching into the midorbit. The soft-tissue contents of the inferior orbital fissure have been transected.
One must ensure that no residual orbital soft tissues are prolapsing into the bony defect prior to implant placement for the reconstruction of the orbital floor.